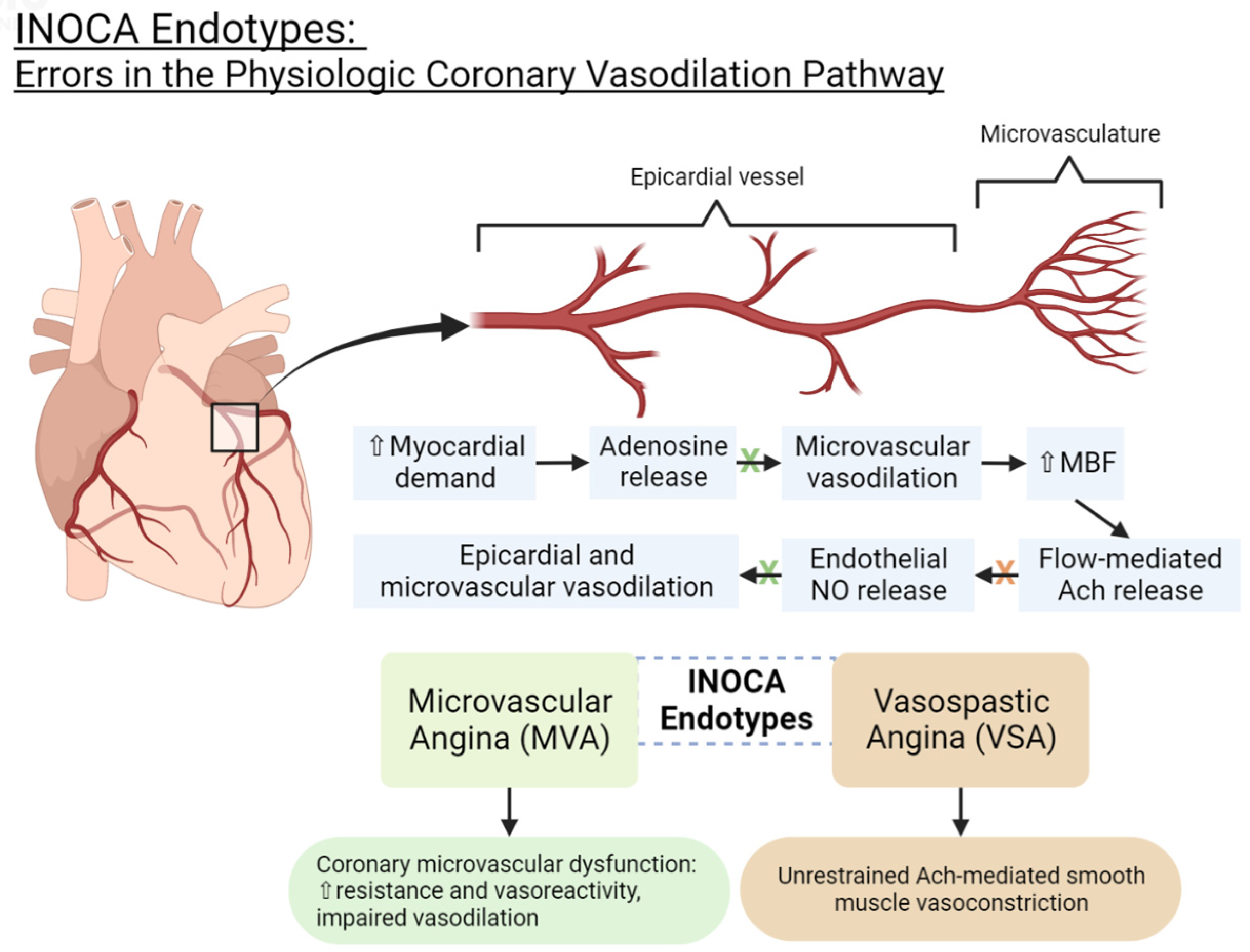
For patients experiencing chest pain but showing no obvious blockages in their coronary arteries, a comprehensive diagnostic workup—including advanced imaging and potentially invasive procedures—can yield significant diagnoses, according to recent findings. This approach is particularly relevant for individuals suspected of having Ischemic Coronary Non-Obstructive CAD (INOCA), a condition often underdiagnosed or attributed to non-cardiac causes.
The challenge with INOCA lies in its subtle presentation. Traditional angiography may appear normal, leading to a dismissal of cardiac concerns. However, research increasingly demonstrates that significant underlying pathology can be present. A thorough investigation, as highlighted in a recent Medscape report, can uncover conditions like coronary microvascular dysfunction, spontaneous coronary artery dissection (SCAD), or vasospasm—all of which can cause debilitating chest pain and increase cardiovascular risk.
Understanding the Diagnostic Yield
The impetus for a more aggressive diagnostic approach stems from the recognition that INOCA isn’t simply “chest pain with clean arteries.” A study published in the Journal of the American College of Cardiology: Cardiovascular Imaging, which informed the Medscape report, showed that a significant proportion of patients initially diagnosed with non-cardiac chest pain actually had identifiable coronary abnormalities when subjected to more advanced testing. Specifically, the research team found that a substantial percentage of patients had evidence of microvascular dysfunction, a condition where the minor blood vessels in the heart don’t function properly, restricting blood flow.
“For a long time, INOCA was a bit of a diagnostic dead end,” explains Dr. Alan Fraser, a cardiologist specializing in INOCA at the University of Edinburgh, in an interview with time.news. “We’d notify patients there was nothing wrong, but their symptoms were very real and significantly impacting their quality of life. Now, we have tools to look beyond the major arteries and identify the root cause of their pain.”
What Does a Comprehensive Workup Entail?
A comprehensive workup for suspected INOCA typically moves beyond standard angiography. Key components often include:
- Coronary CT Angiography (CCTA): This non-invasive imaging technique provides detailed images of the coronary arteries and can detect subtle plaque buildup or anatomical abnormalities.
- Cardiac MRI with Stress Testing: MRI can assess heart muscle function and blood flow during exercise or pharmacological stress, helping to identify areas of ischemia (reduced blood flow).
- Intracoronary Imaging and Functional Testing: In some cases, invasive procedures like intravascular ultrasound (IVUS) or fractional flow reserve (FFR) may be used to assess the function of the coronary microvasculature. FFR measures the pressure difference across a coronary artery stenosis, helping to determine if it’s significantly restricting blood flow.
- Vasospasm Challenge: This involves administering medications that can induce coronary artery spasm, allowing doctors to identify patients with vasospastic angina (Prinzmetal’s angina).
The choice of which tests to perform is individualized, based on the patient’s symptoms, risk factors and initial findings. The goal is to pinpoint the underlying mechanism causing the chest pain and guide appropriate treatment.
Who is at Risk for INOCA?
While anyone can experience chest pain, certain populations are more likely to be affected by INOCA. These include:
- Women: INOCA is disproportionately more common in women than in men.
- Individuals with Microvascular Disease Risk Factors: Conditions like diabetes, hypertension, high cholesterol, and autoimmune diseases can increase the risk of microvascular dysfunction.
- Younger Patients: SCAD, a potential cause of INOCA, is more frequently seen in younger women, particularly those who are pregnant or postpartum.
- Patients with Atypical Chest Pain: Individuals whose chest pain doesn’t fit the classic “angina” pattern may be more likely to have INOCA.
The Importance of Early Diagnosis and Treatment
Delaying diagnosis and treatment of INOCA can have serious consequences. Patients may continue to suffer from debilitating chest pain, leading to reduced quality of life and increased anxiety. INOCA is associated with an increased risk of adverse cardiovascular events, such as heart attack, and stroke. Research published in Circulation demonstrates a higher risk of major adverse cardiac events in patients with INOCA compared to those with obstructive coronary artery disease.
Treatment for INOCA is tailored to the underlying cause. For microvascular dysfunction, lifestyle modifications (diet, exercise, stress management) and medications to improve endothelial function may be recommended. For SCAD, management often involves conservative therapy with medications to control blood pressure and prevent further dissection. Vasospastic angina is typically treated with calcium channel blockers or nitrates to relax the coronary arteries.
Navigating the Diagnostic Process
If you’re experiencing chest pain and suspect you may have INOCA, it’s crucial to advocate for yourself and seek a comprehensive evaluation from a cardiologist experienced in this condition. Don’t hesitate to ask questions about the diagnostic tests being considered and the rationale behind them. A second opinion can likewise be valuable.
The landscape of INOCA diagnosis and treatment is evolving rapidly. Ongoing research is focused on developing new imaging techniques and therapies to improve outcomes for patients with this challenging condition. The American Heart Association has recently released scientific statements to guide clinicians in the diagnosis and management of INOCA, emphasizing the importance of a personalized approach.
The next step in improving care for INOCA patients will likely involve refining risk stratification tools and developing more targeted therapies based on the specific underlying mechanisms driving their symptoms. Further research is also needed to understand the long-term prognosis of INOCA and identify strategies to prevent adverse cardiovascular events.
Have you or a loved one been affected by INOCA? Share your experiences and thoughts in the comments below. Please also share this article with anyone who might find it helpful.
Disclaimer: This article is for informational purposes only and should not be considered medical advice. Please consult with a qualified healthcare professional for any health concerns or before making any decisions related to your health or treatment.