Navigating pneumonia treatment requires a careful balance between swift action and targeted therapy. While standard protocols exist, the evolving landscape of antibiotic resistance, particularly with methicillin-resistant Staphylococcus aureus (MRSA), demands ongoing evaluation. Recent discussion highlights the increasing availability of treatment options for MRSA, but reinforces the importance of reserving broad-spectrum, empirical MRSA coverage for patients presenting with specific risk factors or a confirmed infection. This nuanced approach aims to optimize patient outcomes while minimizing the development of further antibiotic resistance.
Community-acquired pneumonia (CAP) remains a significant public health concern, responsible for a substantial number of hospitalizations and deaths annually. The Centers for Disease Control and Prevention estimates that approximately 1 million adults in the U.S. Are hospitalized with pneumonia each year. Traditionally, treatment guidelines focused on covering common bacterial pathogens like Streptococcus pneumoniae. However, the rise of antibiotic-resistant strains, including MRSA, has complicated the clinical picture. The core principle remains: avoid unnecessary broad-spectrum antibiotic utilize to curb the spread of resistance.
Understanding the MRSA Challenge in Pneumonia
MRSA, often associated with hospital-acquired infections, is increasingly recognized as a cause of CAP, though still less common than other bacterial causes. Identifying patients at high risk for MRSA pneumonia is crucial. These risk factors include a prior MRSA infection, recent hospitalization, residence in a long-term care facility, intravenous drug use, and known colonization with MRSA. The Infectious Diseases Society of America (IDSA) provides detailed guidelines on CAP management, emphasizing risk stratification.
The debate surrounding empirical MRSA coverage – initiating treatment that includes MRSA-active antibiotics before lab results confirm the presence of the bacteria – centers on balancing the potential benefits of early treatment against the risks of unnecessary antibiotic exposure. Overuse of antibiotics contributes to the development of resistance, making future infections harder to treat. Broad-spectrum antibiotics can disrupt the gut microbiome, leading to secondary infections like Clostridioides difficile.
Expanding Treatment Options, Refining Strategy
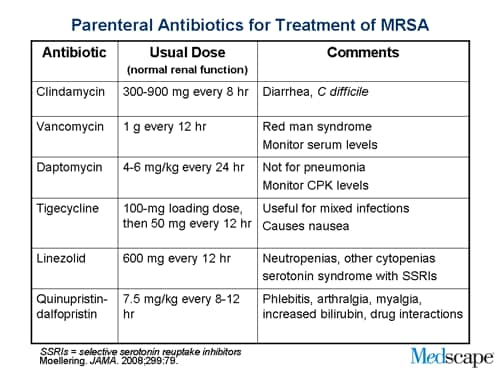
The authors of the original research acknowledge the expanding therapeutic options available to combat MRSA. Newer antibiotics, such as ceftaroline, telavancin, and dalbavancin, offer alternative treatment avenues. However, they emphasize that the availability of these options doesn’t negate the require for a targeted approach. “This increase in treatment options does not change the core principle that empirical MRSA coverage should be reserved for patients with clearly defined risk factors or confirmed infection,” they state.
The key is accurate diagnosis. Rapid diagnostic tests, while not yet universally available, are becoming increasingly important in identifying the causative agent of pneumonia. These tests can help clinicians determine whether MRSA is present and guide antibiotic selection. Molecular diagnostic assays, for example, can detect MRSA DNA in respiratory samples within hours, allowing for more precise treatment decisions.
The Role of Diagnostic Stewardship
Diagnostic stewardship, a parallel concept to antibiotic stewardship, focuses on optimizing the use of diagnostic tests. This involves selecting the most appropriate tests, interpreting results accurately, and using the information to guide treatment decisions. Implementing robust diagnostic stewardship programs can help reduce unnecessary antibiotic use and improve patient outcomes.
advancements in imaging techniques, such as chest CT scans, can help differentiate between bacterial and viral pneumonia, and identify complications like empyema (pus in the pleural space), which may require more aggressive intervention. However, imaging alone cannot definitively identify the causative organism.
What This Means for Patients and Providers
For patients, this means open communication with their healthcare providers is paramount. Discussing any relevant medical history, including prior infections, hospitalizations, and antibiotic use, can help clinicians assess risk factors for MRSA pneumonia. Understanding the rationale behind treatment decisions and asking questions about potential side effects are also important.
For healthcare providers, this underscores the need for adherence to evidence-based guidelines and a commitment to antibiotic stewardship. Careful consideration of risk factors, appropriate use of diagnostic tests, and judicious selection of antibiotics are essential for optimizing patient care and preserving the effectiveness of these life-saving medications. The focus should be on tailoring treatment to the individual patient, rather than adopting a one-size-fits-all approach.
The ongoing evolution of antibiotic resistance necessitates continuous monitoring of local resistance patterns and adaptation of treatment strategies accordingly. Public health surveillance programs play a vital role in tracking the spread of MRSA and other antibiotic-resistant organisms, informing clinical practice and guiding public health interventions.
Looking ahead, further research is needed to develop recent diagnostic tools and therapeutic strategies for MRSA pneumonia. Investigating novel approaches, such as phage therapy and immunotherapy, may offer promising alternatives to traditional antibiotics. The next major update to the IDSA/American Thoracic Society guidelines on CAP is expected in late 2025, incorporating the latest research findings and clinical recommendations.
This information is for general knowledge and informational purposes only, and does not constitute medical advice. It is essential to consult with a qualified healthcare professional for any health concerns or before making any decisions related to your health or treatment.
Have thoughts on this evolving approach to pneumonia treatment? Share your comments below, and please share this article with your network.