Gallbladder surgery, a remarkably common procedure with roughly 750,000 cholecystectomies performed annually in the United States, carries a risk. Between 500 and 1,000 of those surgeries result in severe, unintended injuries to the bile ducts. Now, surgeons are increasingly turning to a decades-old dye, indocyanine green (ICG), and advanced imaging technology to improve safety and reduce these complications. The use of ICG, initially developed during World War II for photography and later approved by the FDA in 1959, is gaining traction as a tool for visualizing biliary anatomy during laparoscopic and robotic procedures.
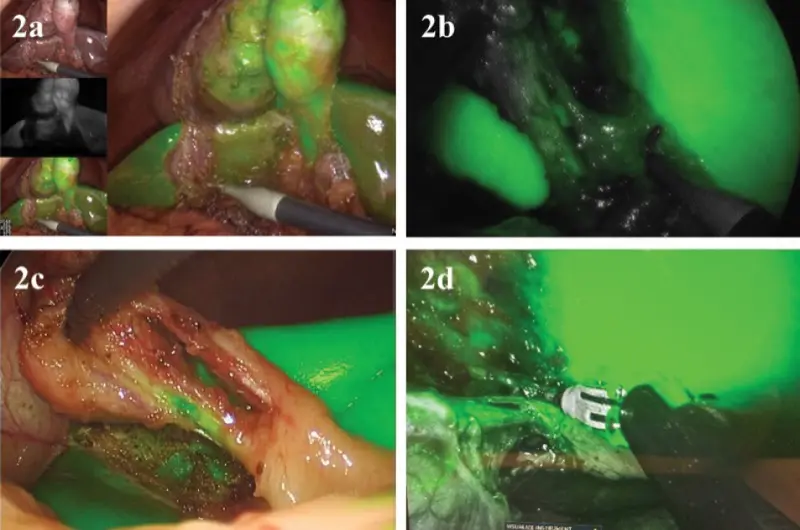
While ICG has been used in medical imaging since the 1980s—initially for liver function tests and retinal imaging—its application in biliary surgery is a more recent development. The dye fluoresces when exposed to near-infrared light, allowing surgeons to clearly identify the cystic duct and artery, crucial structures during gallbladder removal. This enhanced visualization is particularly valuable in complex cases or when anatomical variations are present. The potential to minimize harm in such a frequently performed operation is driving a growing interest in wider adoption of the technique.
Overcoming Barriers to Adoption
Despite the benefits, the integration of ICG into standard surgical practice hasn’t been seamless. Dr. Hugo Bonatti, a general surgeon and associate professor at the University of Maryland Medical Center in Baltimore, has been a vocal advocate for the technology. Speaking at the 2025 annual meeting of the Society of Laparoscopic and Robotic Surgeons/Minimally Invasive Surgery (MIS) Week, Dr. Bonatti highlighted that institutional hurdles and, importantly, surgeon attitudes often limit its use. “Adding safety to gallbladder removal seems like a ‘righteous goal,’” he stated, emphasizing the potential impact of this relatively simple addition to the surgical workflow.
Dr. Bonatti recently reviewed his experience with 349 consecutive laparoscopic and robotic cholecystectomies performed at four hospitals in Maryland—representing a range of settings from rural to urban—to assess ICG uptake. He found that ICG cholangiography was used in 108 cases (31%) and a three-port surgical approach was utilized in 85% of cases. His research also revealed variability in access to robotic platforms and ICG availability across different institutions. Some centers had no access to robotic surgery, while others had limited or restricted access. Similarly, ICG was not consistently available, sometimes being limited to trial periods.
Evaluating Different Imaging Systems
The technology used to visualize the ICG fluorescence also plays a role in its effectiveness. Dr. Bonatti’s study compared several systems, including the SPY Elite (Stryker), Pinpoint (Stryker), and older versions of the SPY and Firefly (Intuitive) systems. He found that Pinpoint offered the best performance, though it requires a 10-mm camera. The newer SPY system, utilizing a 5-mm camera with fusion mode, was also highly rated. The older SPY and Firefly systems, lacking fusion mode, were ranked lower in terms of overall performance.
Dr. Bonatti has also streamlined the ICG administration process, reducing the volume used from 3 to 5 mL to just 1 mL, administered at the time of induction. This simplifies logistics, avoiding delays and challenges associated with pharmacy ordering and nursing or anesthesiology staff application in the post-anesthesia care unit (PACU).
A Call for Enhanced Training
The potential benefits of ICG extend beyond improved visualization. Dr. Bonatti believes that incorporating ICG near-infrared light cholangiography into surgical residency training is crucial. “It makes it safer and faster to identify the structures in many cases of laparoscopic/robotic cholecystectomy,” he explained. He anticipates that major surgical societies will soon issue statements promoting its use. This sentiment is echoed by Dr. Ceana Nezhat, a gynecologic surgeon and medical director of Nezhat Medical Center in Atlanta, who has been a long-time proponent of fluorescence image-guided surgery, using these agents on a near-daily basis for 15 years. Dr. Nezhat notes that broader acceptance hinges on surgeons’ willingness to embrace new technologies. “I haven’t really experienced institutional resistance, but people tend to adhere to the old way of doing things,” she said.
The growing popularity of ICG and similar technologies extends beyond general surgery, with increasing applications in urology and oncology. Yet, the pace of adoption remains uneven. Access to robotic platforms and the availability of ICG itself continue to be limiting factors in some institutions.
Looking Ahead
As ICG technology continues to evolve and become more accessible, its role in minimizing complications during cholecystectomy is likely to expand. The development of advanced fusion modes in newer imaging systems, like the da Vinci 5 platform, further enhances visualization and precision. The ongoing research and advocacy efforts of surgeons like Dr. Bonatti are paving the way for wider implementation and, safer surgical outcomes for patients undergoing gallbladder removal. The Society of Laparoscopic and Robotic Surgeons is expected to release updated guidelines on the use of ICG in biliary surgery at their next annual meeting in 2026.
This article is for informational purposes only and does not constitute medical advice. Always consult with a qualified healthcare professional for any health concerns or before making any decisions related to your health or treatment.
Have thoughts on the evolving role of ICG in surgery? Share your comments below, and please share this article with your network.