The landscape of obesity treatment has shifted dramatically with the rise of GLP-1 medications for weight loss, turning what was once a struggle of willpower into a manageable biological challenge. Drugs like semaglutide and tirzepatide have moved beyond the clinic and into the cultural zeitgeist, promising rapid weight reduction for millions. However, as a physician, I have observed that the conversation often focuses on the number on the scale while ignoring the composition of the weight being lost.
While the efficacy of these medications in reducing overall body mass is well-documented, the biological trade-off is significant. Rapid weight loss induced by GLP-1 receptor agonists often includes a substantial loss of lean muscle mass, a phenomenon that can lead to metabolic slowdown and increased frailty if not aggressively managed. The goal of medical weight loss is not simply a lower number, but the preservation of metabolic health and functional strength.
Understanding the distinction between fat loss and weight loss is critical for anyone utilizing these therapies. When the body enters a steep caloric deficit—exacerbated by the potent appetite suppression of these drugs—it may catabolize muscle tissue for energy. This process, if left unchecked, can result in “sarcopenic obesity,” where a person has a lower weight but a higher percentage of body fat and lower muscle mass than they had previously.
The Biological Mechanism of Satiety
GLP-1 (glucagon-like peptide-1) is a hormone naturally produced in the gut. It serves several key functions: it stimulates insulin secretion, inhibits glucagon and slows gastric emptying. By mimicking this hormone, medications such as Wegovy and Zepbound signal the brain’s hypothalamus to increase feelings of fullness and decrease hunger signals.
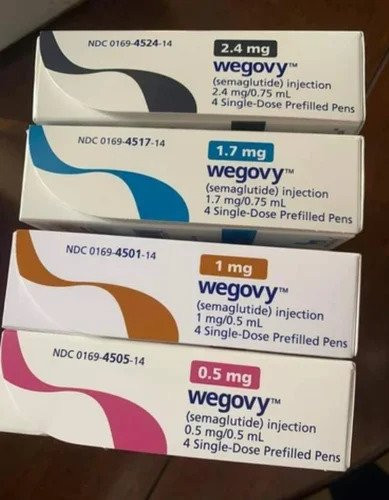
This pharmacological intervention effectively “quiets” the food noise that often plagues individuals with chronic obesity. However, the very efficiency of this suppression is what creates the risk of muscle wasting. Because patients often eat far fewer calories than their bodies require for basic maintenance, the body begins to break down skeletal muscle to meet its amino acid needs.
The difference between the primary medications lies in their targets. Semaglutide targets only the GLP-1 receptor, while tirzepatide is a dual agonist, targeting both GLP-1 and GIP (glucose-dependent insulinotropic polypeptide) receptors. According to clinical data, this dual action can lead to even greater weight reduction, but it similarly necessitates a strict focus on lean body mass preservation via the FDA.
Mitigating Muscle Loss Through Nutrition and Training
To prevent the loss of lean body mass, the clinical approach must shift from “eating less” to “eating specifically.” The most critical intervention is a significant increase in protein intake. Protein provides the necessary building blocks (amino acids) to maintain muscle tissue even while the body is in a fat-burning state.
Medical guidelines generally suggest that patients on GLP-1 therapies prioritize protein at every meal. Because appetite is suppressed, patients must be intentional about consuming high-quality proteins—such as lean meats, fish, legumes, or whey supplements—before they perceive full. Without this intentionality, the caloric deficit becomes too extreme, and muscle loss accelerates.
Equally important is the implementation of resistance training. Cardiovascular exercise is beneficial for heart health, but only strength training—lifting weights, using resistance bands, or bodyweight exercises—signals the body to retain muscle. When a muscle is challenged, the body receives a chemical signal that the tissue is necessary for survival, which helps protect it from being burned as fuel.
Essential Strategies for GLP-1 Users
- Prioritize Protein: Aim for higher protein targets to counteract the natural catabolic state of rapid weight loss.
- Strength Training: Engage in resistance exercises at least two to three times per week.
- Hydration and Electrolytes: Slowed gastric emptying can affect nutrient absorption; maintaining hydration is vital.
- Gradual Titration: Following the prescribed dosage ramp-up to minimize gastrointestinal side effects like nausea and vomiting.
Comparing Leading GLP-1 Therapies
While both semaglutide and tirzepatide are highly effective, they differ slightly in their pharmacological profile and typical outcomes.
| Medication | Active Ingredient | Primary Target | Common Brand Names |
|---|---|---|---|
| Semaglutide | Semaglutide | GLP-1 Receptor | Ozempic, Wegovy |
| Tirzepatide | Tirzepatide | GLP-1 & GIP Receptors | Mounjaro, Zepbound |
Long-term Considerations and Metabolic Health
The ultimate goal of using GLP-1 medications for weight loss is to achieve a sustainable metabolic state. One of the primary concerns among clinicians is the “rebound effect.” If a patient loses a significant amount of muscle during their treatment, their basal metabolic rate (BMR)—the number of calories they burn at rest—drops. This makes it significantly easier to regain weight once the medication is tapered or stopped.
Maintaining muscle mass essentially “protects” the metabolism. By keeping the BMR higher, patients are better positioned to maintain their weight loss through lifestyle interventions after the pharmacological phase of treatment. This shift in focus from “weight loss” to “body recomposition” is what separates a temporary fix from a long-term health transformation.
Patients should also be aware of potential side effects. While most are transient, such as nausea or constipation, some individuals may experience more severe gastrointestinal issues. Regular monitoring by a healthcare provider is essential to ensure that the medication is working in harmony with the patient’s overall health profile as outlined by Mayo Clinic.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition or treatment.
As clinical trials continue, the next major checkpoint for these therapies will be the study of their long-term effects on cardiovascular health and the potential for permanent metabolic reprogramming. Further data is expected from ongoing longitudinal studies regarding the durability of weight loss and the efficacy of various “exit strategies” for patients transitioning off the medication.
We invite you to share your experiences with metabolic health and weight management in the comments below or share this guide with someone beginning their journey.