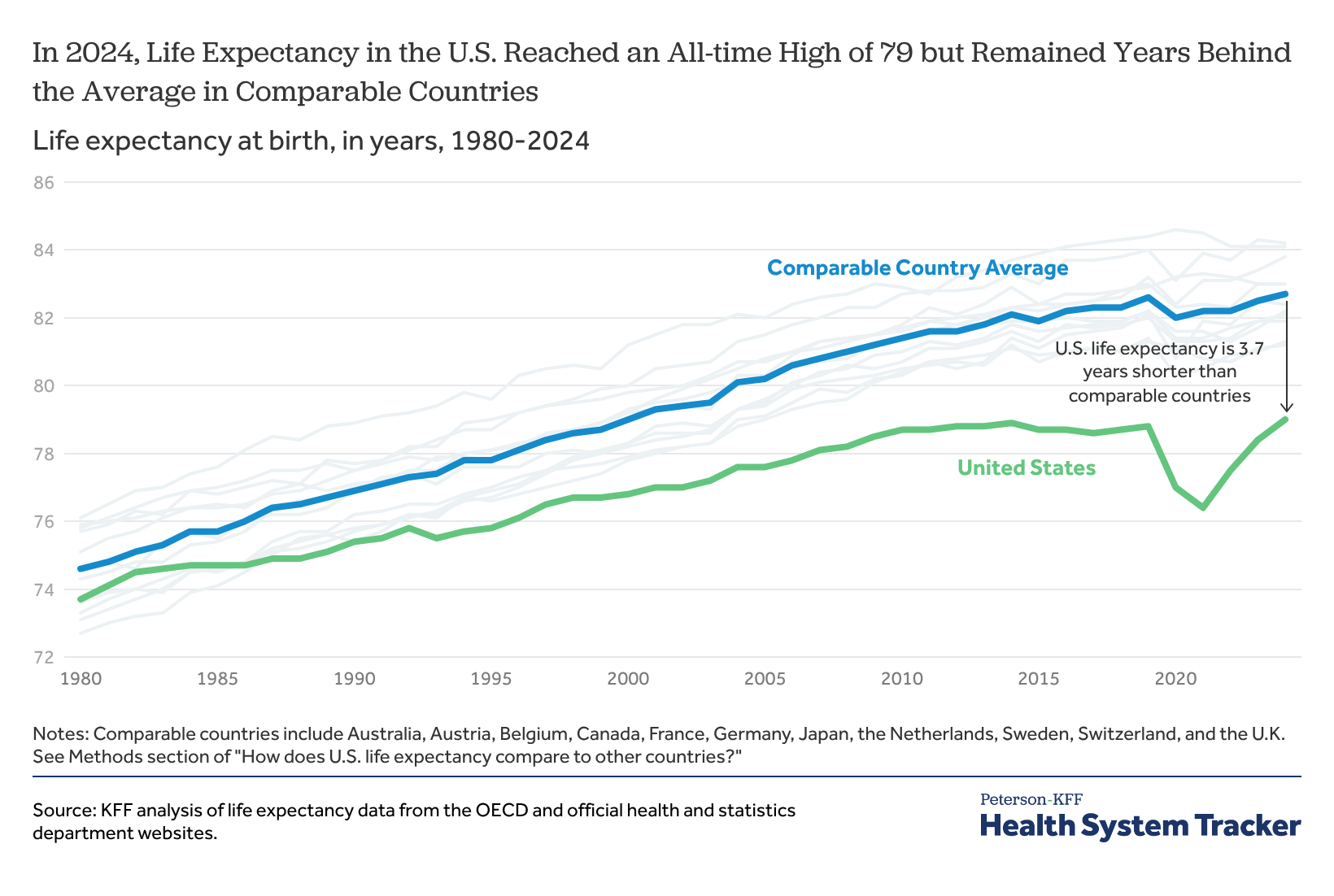
U.S. Life expectancy at birth has reached its highest-ever level, rising to 79.0 years in 2024, a slight increase of 0.6 years from the 78.4 years recorded in 2023. Although the upward trend suggests a recovery from the devastating impacts of the pandemic era, the milestone is tempered by a sobering reality: Americans continue to live significantly shorter lives than people in other wealthy, industrialized nations.
According to an analysis by the Peterson-KFF Health System Tracker, the average life expectancy across a group of comparable high-income countries stands at 82.7 years. This leaves a persistent gap of approximately 3.7 years between the U.S. And its global peers, raising critical questions about why the world’s largest economy struggles to match the longevity of other developed nations.
As a physician, I view these numbers not just as statistics, but as a reflection of systemic failures in public health and primary care. When we spot a multi-year gap in life expectancy among countries with similar wealth, it suggests that the issue isn’t a lack of resources, but rather how those resources are distributed and utilized to prevent premature death.
The Wealth Paradox: Spending More for Less
The disparity in how we U.S. Life expectancy compare to other countries is particularly striking when viewed alongside healthcare spending. The United States consistently spends more per capita on healthcare than any other nation, yet it frequently lags in basic health outcomes. This “wealth paradox” indicates that high-tech interventions and specialized care—areas where the U.S. Excels—cannot fully compensate for deficiencies in preventative medicine and social stability.

The comparison focuses on a cohort of similarly large and wealthy members of the Organisation for Economic Co-operation and Development (OECD), including Australia, Austria, Belgium, Canada, France, Germany, Japan, the Netherlands, Sweden, Switzerland, and the United Kingdom. In these nations, integrated health systems often prioritize primary care and universal access, which helps catch chronic conditions before they become fatal.
To visualize this gap, the following data highlights the variance between the U.S. And the average of its peer group:
| Region/Country Group | Life Expectancy at Birth | Difference from U.S. |
|---|---|---|
| United States | 79.0 years | — |
| Comparable OECD Average | 82.7 years | +3.7 years |
| Japan (Highest Peer) | Approx. 84+ years | +5.0+ years |
Identifying the Drivers of Premature Mortality
The gap in longevity is not driven by a single factor but by a convergence of “deaths of despair,” chronic disease, and systemic violence. While the 0.6-year increase in 2024 is a positive sign, it does not erase the structural vulnerabilities that keep U.S. Averages low.
One of the most significant contributors is the opioid epidemic. The U.S. Has faced a crisis of substance use disorders and accidental overdoses at a scale virtually unseen in other OECD nations. This has disproportionately lowered life expectancy among working-age adults, dragging down the national average.
Beyond substance use, the U.S. Struggles with higher rates of obesity and related metabolic syndromes, such as Type 2 diabetes and cardiovascular disease. While the medical system is highly capable of treating a heart attack or a stroke, it is less effective at preventing them through nutrition, urban planning, and accessible primary care. In contrast, many European peers have more robust public health frameworks that integrate diet and exercise into the fabric of daily life.
the U.S. Faces unique challenges regarding safety and maternal health. High rates of gun violence and a concerning trend of rising maternal mortality—particularly among Black women—contribute to a higher burden of preventable deaths that are far less common in countries like Canada or Switzerland.
What This Gap Means for Public Health
When we analyze who is most affected, the data reveals that the life expectancy gap is not distributed evenly. Socioeconomic status, race, and geography play massive roles. In many comparable OECD countries, the difference in life expectancy between the richest and poorest citizens is far narrower than it is in the United States.
This suggests that the U.S. Health system is highly efficient for those with premium insurance and high incomes, but fails those at the margins. The “highest-ever level” of 79.0 years is a victory for the average, but it masks deep inequities in how long different populations are expected to survive.
For those looking to dive deeper into the data, the Peterson-KFF chart collection provides a detailed breakdown of these trends across the OECD member states.
The Path Forward and Next Checkpoints
Closing the gap will require more than just medical breakthroughs; it will require addressing the social determinants of health—housing, food security, and environmental safety. The recent uptick in life expectancy indicates that the acute shocks of the early 2020s are receding, but the structural deficit remains.
Medical professionals and policymakers are now looking toward the next set of comprehensive data releases from the Centers for Disease Control and Prevention (CDC) and the World Health Organization (WHO), which will provide more granular detail on whether this recovery is consistent across all demographic groups or limited to specific populations.
Disclaimer: This article is provided for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
Do you consider the U.S. Can ever close the longevity gap with other wealthy nations? Share your thoughts in the comments or share this article to join the conversation.