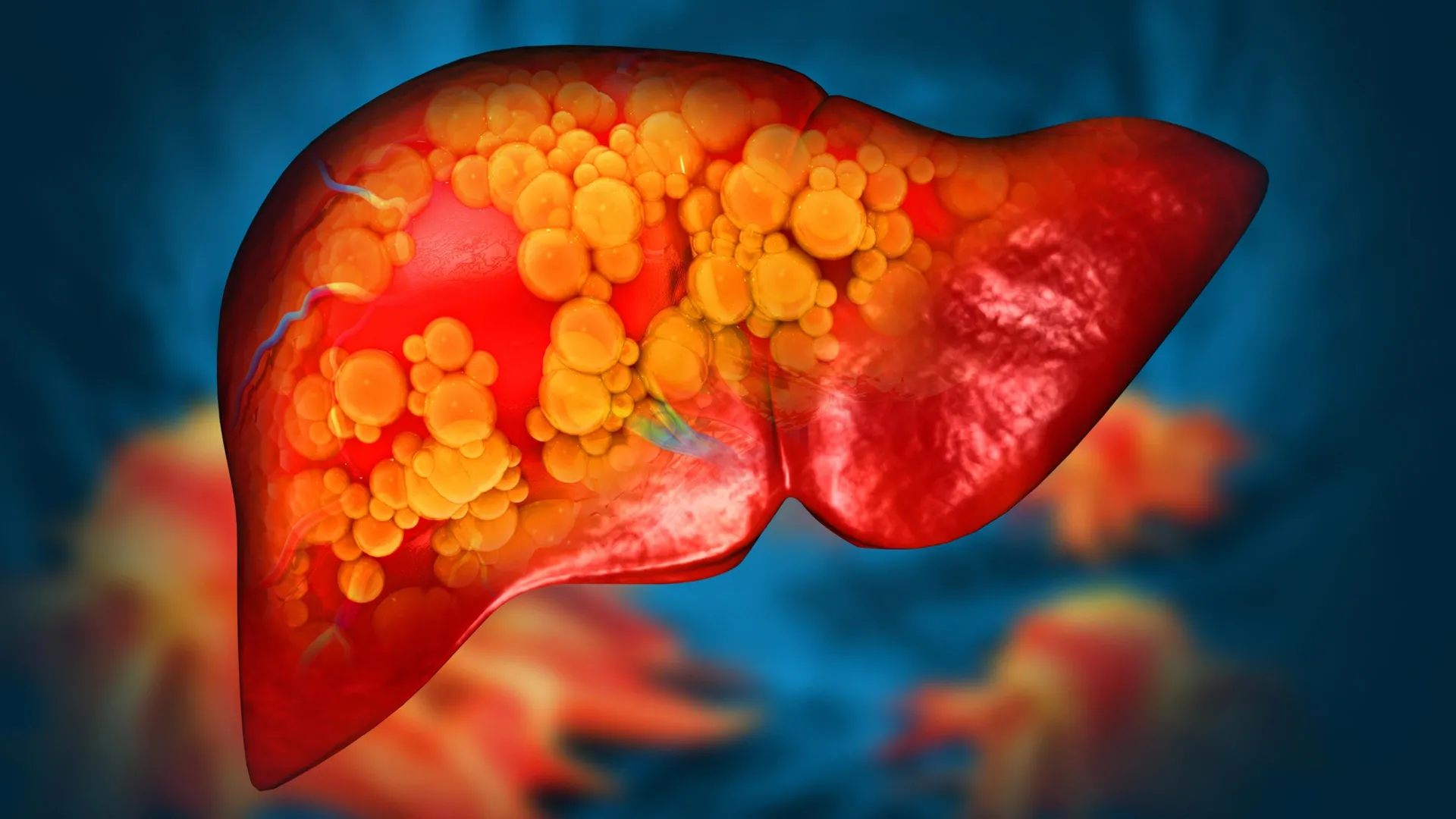
For many adults, the “weekend warrior” approach to alcohol consumption feels like a safe compromise. The logic is simple: if you abstain or drink lightly from Monday through Thursday, a few heavy nights on Friday or Saturday shouldn’t do much damage. But, new medical evidence suggests that this pattern of consumption may be far more dangerous than previously understood, particularly for those with underlying metabolic health issues.
Research published in Clinical Gastroenterology and Hepatology indicates that binge drinking just once a month may triple your risk of liver scarring for individuals living with metabolic dysfunction–associated steatotic liver disease (MASLD). The findings challenge a long-standing clinical focus on the total volume of alcohol consumed over time, suggesting instead that the pattern of drinking is a critical driver of liver damage.
The study reveals that people who engage in episodic heavy drinking—defined as four or more drinks in a single day for women and five or more for men, occurring at least once a month—face significantly higher odds of developing advanced liver fibrosis. Fibrosis is the medical term for the buildup of scar tissue in the liver, which, if left unchecked, can lead to cirrhosis and liver failure.
For those with MASLD, the risk is stark: episodic heavy drinkers were nearly three times more likely to experience advanced liver fibrosis than individuals who consumed the same total amount of alcohol spread out over several days or weeks.
The hidden prevalence of MASLD
To understand why these findings are so impactful, it is necessary to seem at the scale of MASLD. Once commonly referred to as non-alcoholic fatty liver disease (NAFLD), MASLD is currently the most common liver condition in the United States, affecting approximately one-in-three adults.

Unlike alcohol-related liver disease, MASLD is primarily driven by metabolic factors. It typically affects individuals with excess weight, obesity, or other metabolic conditions such as Type 2 diabetes, high blood pressure, or high cholesterol. While MASLD is not defined by alcohol use, the research suggests that alcohol acts as a powerful catalyst, accelerating the progression from simple fat accumulation to permanent scarring.
According to the study, nearly 16% of patients with MASLD reported engaging in episodic heavy drinking, while more than half of the general adult population included in the broader data set reported similar patterns. This overlap creates a high-risk intersection where metabolic vulnerability meets acute chemical stress.
How drinking patterns drive liver fibrosis
The distinction between “moderate” and “episodic” drinking is where the danger lies. Traditionally, physicians have screened patients based on their weekly or monthly totals. For example, moderate drinking is generally defined as seven drinks or fewer per week for women and 14 or less for men.
However, the data suggests that the liver reacts differently to a concentrated “hit” of alcohol than to a distributed amount. Dr. Brian P. Lee, a hepatologist and liver transplant specialist with Keck Medicine of USC and the study’s principal investigator, notes that this is a critical “wake-up call” for both patients and providers.
“Traditionally, physicians have tended to look at the total amount of alcohol consumed, not how it is consumed, when determining the risk to the liver,” Lee said. “Our research suggests that the public needs to be much more aware of the danger of occasional heavy drinking and should avoid it even if they drink moderately the rest of the time.”
From a physiological standpoint, consuming large amounts of alcohol in a single session can overwhelm the liver’s metabolic capacity. This surge triggers acute inflammation, which prompts the body to create scar tissue to repair the damage. In a liver already stressed by MASLD—where fat deposits have already created a baseline of inflammation—this additional insult can rapidly accelerate the path toward advanced fibrosis.
Comparing Alcohol Consumption Patterns
| Drinking Category | Definition (Women) | Definition (Men) | Impact on MASLD Patients |
|---|---|---|---|
| Moderate | &le. 7 drinks / week | ≤ 14 drinks / week | Baseline risk associated with metabolic health |
| Episodic Heavy | ≥ 4 drinks / day (1x month) | ≥ 5 drinks / day (1x month) | ~3x higher risk of advanced fibrosis |
| Chronic Heavy | High daily intake | High daily intake | Highest risk of alcohol-related liver disease |
The methodology behind the findings
The research team utilized a robust, nationally representative dataset from the National Health and Nutrition Examination Survey (NHANES). By analyzing data from more than 8,000 adults collected between 2017 and 2023, the researchers were able to isolate the effects of drinking patterns from other variables.
To ensure accuracy, the team compared people with MASLD who shared similar ages, sexes, and average weekly alcohol intake. By segmenting these individuals into episodic heavy drinkers and non-episodic drinkers, they were able to conclude that the timing of the alcohol consumption—rather than the total volume—was the variable driving the increased odds of liver scarring.
The study similarly noted a demographic trend: younger adults and men were more likely to report episodic heavy drinking. There was a dose-response relationship, meaning that the more drinks consumed during a single episode, the more severe the liver fibrosis tended to be.
A growing public health crisis
This research comes at a time when liver disease is on the rise across the U.S. Population. Alcohol-related liver disease has more than doubled in the last 20 years, a trend that Dr. Lee attributes to a “perfect storm” of factors. These include pandemic-era surges in alcohol consumption and an increase in the prevalence of obesity and diabetes, which are the primary drivers of MASLD.
While the study specifically focused on those with metabolic liver disease, the implications may extend to the general population. Since MASLD is so prevalent—affecting one-third of adults—a significant portion of the public may be unknowingly living with a liver that is hypersensitive to the effects of binge drinking.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
As the medical community continues to refine the definitions of liver disease, the next phase of research will likely focus on identifying early biomarkers that can predict which MASLD patients are most susceptible to alcohol-induced fibrosis. This could lead to more personalized screening protocols and targeted interventions for high-risk drinkers.
We invite you to share this article and join the conversation in the comments below about how we can better address metabolic health and alcohol awareness in our communities.