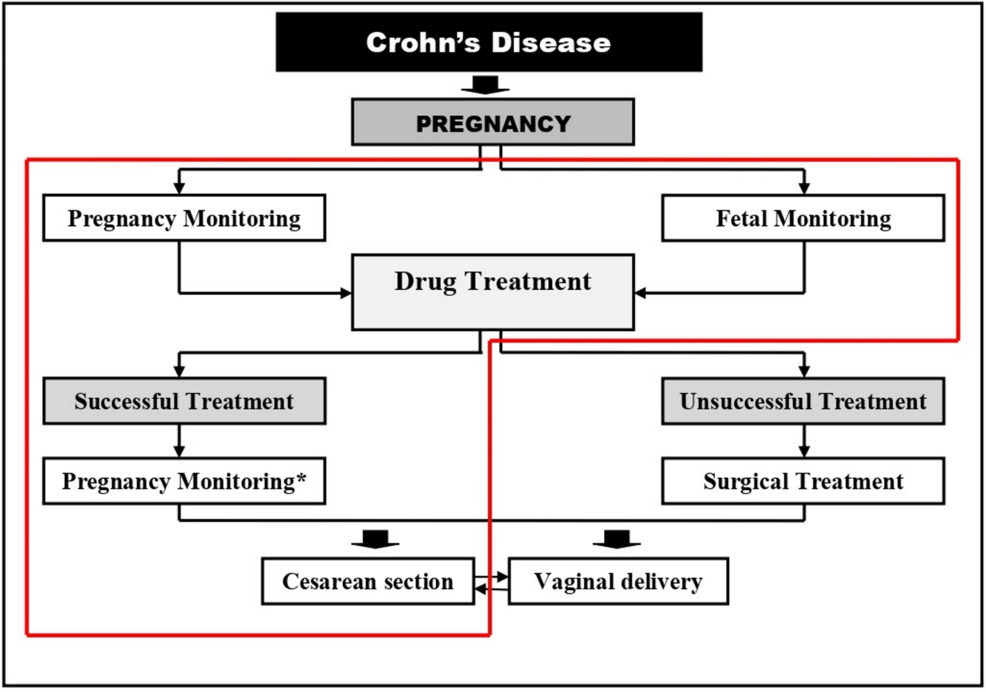
For many women living with Crohn’s disease, the dream of starting a family can be clouded by a complex history of flares, medications, and surgical interventions. The fear that a body already strained by chronic inflammation and prior intestinal surgery might not support a healthy pregnancy is a common, heavy burden.
Still, recent clinical evidence suggests that with a coordinated, multidisciplinary approach, a pregnancy with Crohn’s disease and prior intestinal surgery can lead to a successful and healthy outcome. A recent case report highlights the journey of a 28-year-old woman whose path to motherhood serves as a roadmap for others navigating the intersection of inflammatory bowel disease (IBD) and maternal health.
The case underscores a critical shift in gastroenterology: the move away from viewing IBD as a barrier to pregnancy and toward a strategy of aggressive remission management. By prioritizing stability before and during gestation, medical teams can significantly mitigate the risks traditionally associated with complex bowel histories.
Navigating a Complex Surgical History
The patient in the report had been battling Crohn’s disease since the age of 18, a decade of instability that eventually required an ileocecal resection—a surgical procedure to remove the end of the compact intestine and the beginning of the large intestine. For patients with such a history, pregnancy introduces specific anatomical and physiological challenges, including the risk of intestinal adhesions or nutrient malabsorption.
Despite these hurdles, the patient achieved a successful pregnancy. The key to her outcome was not the absence of disease, but the presence of deep remission. Clinical guidelines from the Crohn’s & Colitis Foundation emphasize that the most significant predictor of a positive pregnancy outcome is the disease activity level at the time of conception.
In this specific case, the patient’s history of prior intestinal surgery did not prevent a full-term pregnancy, provided that her nutritional status was monitored and her inflammatory markers remained low.
The Role of Biologic Therapy in Gestation
One of the most debated aspects of IBD pregnancy is the use of potent medications. For years, patients were often advised to discontinue medications out of fear of fetal impact. However, current medical consensus has pivoted: the risk of a disease flare during pregnancy is generally considered more dangerous to the fetus than the medications used to treat the disease.
The patient in the report was managed with Infliximab, a biologic therapy that targets tumor necrosis factor (TNF). Rather than stopping the medication, her care team maintained the therapy to ensure she remained in remission. This strategy is supported by data suggesting that maintaining biologic therapy reduces the likelihood of preterm birth and low birth weight, which are more frequently caused by active inflammation than by the drugs themselves.
Balancing Medication and Fetal Safety
The management of biologics during pregnancy typically follows a nuanced timeline to balance maternal health with neonatal considerations:
- Pre-conception: Achieving and documenting clinical remission.
- First and Second Trimesters: Continuing maintenance therapy to prevent flares.
- Third Trimester: In some cases, clinicians may adjust the timing of the final doses to reduce the concentration of the drug that crosses the placenta, thereby minimizing the risk of the infant developing transient neonatal antibodies.
The Power of the Multidisciplinary Care Team
A successful outcome in complex cases is rarely the result of a single doctor’s effort. The case report illustrates the necessity of a “team-based” approach, where communication between specialists is seamless. This ensures that the patient is not receiving conflicting advice, which can be a major source of stress for high-risk mothers.
The core team for a patient with Crohn’s and a surgical history typically includes:
- Gastroenterologist: To monitor bowel inflammation and manage biologic dosing.
- Obstetrician/Maternal-Fetal Medicine (MFM) Specialist: To handle high-risk prenatal care and monitor fetal growth.
- Registered Dietitian: To ensure the patient is absorbing critical nutrients like folic acid and B12, which can be compromised after an ileocecal resection.
- Mental Health Professional: To support the patient through the anxiety of chronic illness during pregnancy.
| Factor | Risk if Unmanaged | Management Strategy |
|---|---|---|
| Disease Activity | Preterm birth, low birth weight | Achieve remission before conception |
| Medication | Disease flare-up | Continue safe biologics (e.g., Infliximab) |
| Surgical History | Nutrient malabsorption | Nutritional screening and supplementation |
| Care Model | Fragmented treatment | Multidisciplinary team coordination |
What In other words for Future Patients
This case report serves as a vital piece of evidence for women who may feel their surgical history disqualifies them from a healthy pregnancy. It demonstrates that prior intestinal surgery is not a contraindication to motherhood, but rather a requirement for more meticulous planning.
The broader implication for public health is the need for better pre-conception counseling. When patients are empowered with the knowledge that biologics can be managed safely and that surgical histories can be navigated, they are more likely to seek the proactive care necessary for a healthy delivery.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Patients should consult their healthcare provider for personalized medical guidance regarding IBD and pregnancy.
The next step for clinicians in this field is the continued collection of long-term data on children born to mothers on biologic therapies, ensuring that the benefits of maternal remission translate into lifelong health for the child. Ongoing registries and longitudinal studies will provide the final confirmation of these safety profiles.
Do you have experience navigating a chronic illness during pregnancy? Share your story in the comments or share this article with someone who needs to know that a healthy outcome is possible.