In the high-pressure environment of a cardiac arrest, the primary goal is simple: restart the heart. Yet, for patients with complex medical histories, the battle does not end with the return of a pulse. A recent clinical case highlights a dangerous diagnostic blind spot that occurs after successful resuscitation, where the signs of a stroke can be easily mistaken for the general brain damage caused by a lack of oxygen.
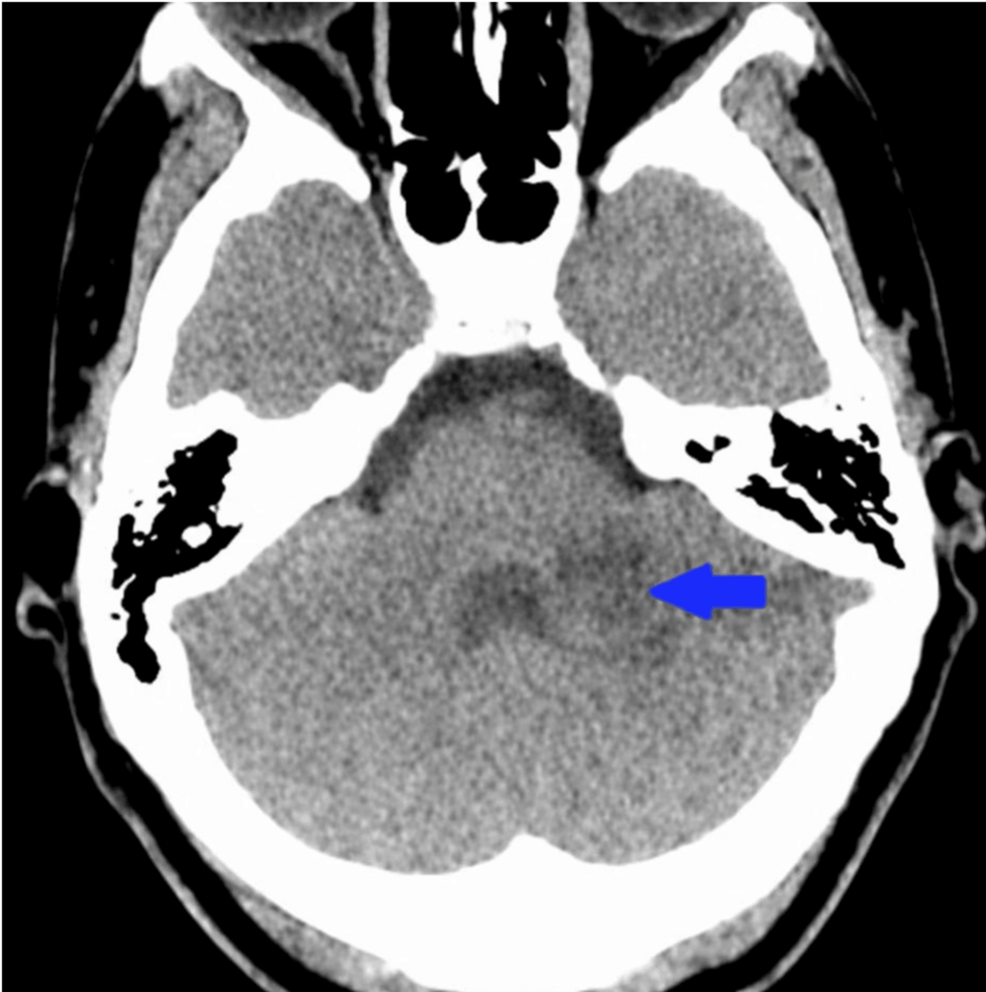
The case involved a 45-year-vintage man with end-stage heart failure and a history of cocaine use who suffered a pulseless electrical activity arrest in end-stage heart failure. Whereas medical teams successfully achieved a return of spontaneous circulation (ROSC), the patient’s subsequent neurological recovery was atypical. Instead of the expected global cognitive impairment seen after a cardiac arrest, the patient exhibited specific coordination failures and balance issues, revealing a hidden cerebellar infarction—a stroke in the back of the brain.
For clinicians, this scenario represents a significant diagnostic pitfall. In the immediate aftermath of a cardiac arrest, it is common to attribute neurological deficits to hypoxic-ischemic encephalopathy (HIE), the general damage caused when the brain is deprived of oxygen. When a patient presents with altered consciousness or motor dysfunction, the “global” explanation often takes precedence over the search for a “focal” cause, such as a localized stroke.
The Mechanics of Pulseless Electrical Activity
Unlike ventricular fibrillation, where the heart quivers chaotically, pulseless electrical activity (PEA) is a more deceptive state. In PEA, the heart’s electrical system continues to fire—the monitor shows a rhythm—but the muscle fails to contract effectively enough to pump blood to the rest of the body. It is essentially a mechanical failure despite an electrical signal.
In this patient’s case, the PEA was compounded by end-stage heart failure, characterized by a severely reduced ejection fraction of 15%. The American Heart Association notes that PEA is often the result of reversible causes, but in patients with chronic heart failure, the heart muscle is often too scarred or weak to respond to standard resuscitation efforts.
The situation was further complicated by cocaine-associated cardiotoxicity. Cocaine acts as a powerful vasoconstrictor, narrowing the arteries that supply the heart and brain. This not only increases the workload on an already failing heart but can likewise trigger myocardial necrosis—the death of heart tissue—and promote the formation of blood clots.
The Synergy of Risk: Cocaine and Heart Failure
The intersection of substance use and chronic cardiac disease creates a “perfect storm” for vascular events. Cocaine increases the risk of cardiovascular collapse through several mechanisms, including the stimulation of the sympathetic nervous system and the direct toxicity it exerts on cardiomyocytes.
When paired with end-stage heart failure, the risk of a thromboembolic event—where a clot travels from the heart to the brain—increases dramatically. In this patient, the combination of a low-flow state during the arrest and the pro-thrombotic environment created by cocaine use likely contributed to the cerebellar infarction.
Comparing Post-Arrest Neurological Complications
Distinguishing between global brain injury and a localized stroke is critical for determining the patient’s prognosis and subsequent care. The following table outlines the primary differences observed in post-resuscitation patients.
| Feature | Hypoxic-Ischemic Encephalopathy (HIE) | Focal Infarction (Stroke) |
|---|---|---|
| Scope of Damage | Global/Diffuse brain injury | Localized to a specific artery/region |
| Primary Symptoms | Coma, generalized confusion, myoclonus | Ataxia, unilateral weakness, specific aphasia |
| Imaging Findings | Diffuse edema or cortical necrosis | Defined area of ischemia (e.g., cerebellum) |
| Mechanism | Systemic lack of oxygen/perfusion | Vascular occlusion or embolism |
Identifying the Diagnostic Pitfall
The “pitfall” in this case occurred during the post-resuscitation phase. After ROSC, the patient did not immediately regain full consciousness, which is common in HIE. However, as he began to wake, he displayed ataxia—a lack of muscle coordination—and significant instability. Because the patient had just survived a major cardiac arrest, these symptoms were initially viewed as part of the broader recovery from oxygen deprivation.
It was only through targeted neuroimaging that the medical team discovered a cerebellar infarction. The cerebellum is responsible for motor control and balance; a stroke in this region produces distinct deficits that differ from the cognitive “fog” of HIE. According to the National Institute of Neurological Disorders and Stroke, cerebellar strokes can be particularly dangerous as they may lead to obstructive hydrocephalus or brainstem compression if not identified early.
This case underscores the necessity of maintaining a high index of suspicion for focal neurological injuries in post-arrest patients, especially those with risk factors like cocaine use or structural heart disease. When a patient’s neurological recovery is asymmetric or presents with focal deficits, imaging should be prioritized over the assumption of global injury.
Clinical Implications for Recovery
The discovery of the stroke changed the trajectory of the patient’s care. While HIE management focuses on temperature control and sedation to protect the brain, the management of an infarction requires a different approach, focusing on blood pressure stabilization and the prevention of further embolic events.
For the broader medical community, this case suggests that the “standard” post-arrest neurological assessment may be insufficient for high-risk populations. The integration of early MRI or CT angiography may be necessary for patients who exhibit focal signs, ensuring that treatable or manageable vascular events are not overlooked in the shadow of a cardiac arrest.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
The next step for clinicians in improving post-resuscitation outcomes involves the refinement of neuro-prognostication tools. Research is ongoing into the use of biomarkers and advanced imaging to better differentiate between various types of brain injury in the first 72 hours following ROSC, which will allow for more personalized rehabilitative strategies.
Do you believe post-arrest protocols should mandate early neuroimaging for all high-risk patients? Share your thoughts in the comments below.