For decades, the medical approach to Crohn’s disease has focused primarily on extinguishing the “fire” of inflammation. While modern biologics and steroids have grow highly effective at reducing this immune response, a stubborn and debilitating complication often remains: the scar tissue left behind.
A recent Crohn’s disease fibrosis breakthrough led by researchers at the University of Edinburgh has finally identified the cellular trigger responsible for this scarring, offering a potential roadmap for treatments that do more than just manage inflammation. By uncovering how specific immune cells drive the production of excessive collagen, scientists may now be able to develop therapies that prevent or even slow the progression of intestinal fibrosis.
Fibrosis is a severe complication of this chronic inflammatory bowel disease, occurring when the body’s attempt to heal inflamed tissue goes into overdrive. This results in a buildup of collagen that thickens and stiffens the bowel wall, leading to “strictures”—narrowed sections of the intestine that can block the flow of digestive contents. For many patients, these blockages are surgical emergencies, yet current medications are largely powerless to reverse the scarring once it has formed.
The Gap in Current Crohn’s Care
The distinction between inflammation and fibrosis is critical. Most current Crohn’s therapies target the active immune response to stop the gut from attacking itself. Still, fibrosis is a structural change. Once the bowel wall becomes scarred, reducing inflammation does not necessarily “un-scar” the tissue.
Dr. Shahida Din, a consultant gastroenterologist at NHS Lothian and honorary senior clinical lecturer at the University of Edinburgh, explains that this has been a significant hurdle in patient care. “Fibrosis remains one of the most challenging complications of Crohn’s disease because current treatments primarily target inflammation rather than the scarring itself,” Din said. “Understanding the cellular signalling pathways that link immune activity to collagen production could facilitate guide the development of therapies aimed at preventing or slowing fibrosis.”
Without a way to target the fibrosis directly, many patients fall into a cycle of recurring strictures and repeated surgeries, as the disease often returns to the same sites, causing new scars to form.
Mapping the Cellular Trigger
To identify the source of the scarring, the research team focused on the ileum—the final section of the small intestine, where Crohn’s most frequently manifests. By analyzing both archived and fresh intestinal tissue samples, they examined the different layers of the bowel wall.
The team discovered that the submucosa, a deeper layer of the bowel wall, exhibited particularly high levels of scarring. This suggests that the early stages of fibrosis may be rooted deeper in the tissue than previously understood. To pinpoint the exact cause, the researchers employed a high-resolution technique called single-cell RNA sequencing, which allows scientists to study the gene activity of individual cells.
The findings revealed a complex “conversation” between three types of cells:
- Crohn’s Lymphoid Aggregates: Clusters of immune cells that act as the primary drivers.
- Endothelial Cells: Cells that line the blood vessels, which were found to form distinctive structures surrounding the immune clusters.
- Collagen-Producing Cells: The cells that actually build the scar tissue.
The research suggests that the lymphoid aggregates signal the endothelial cells, which in turn stimulate the collagen-producing cells to create the excessive scar tissue. Dr. Michael Glinka, a research fellow at the University of Edinburgh, noted that these interactions were previously unrecognized. “By combining traditional pathology with single-cell transcriptomics, we were able to confirm these changes using two independent approaches and uncover biological signalling pathways that may provide new therapeutic targets,” Glinka said.
The Human Cost of Intestinal Scarring
For patients, the biological “signaling pathways” translate into a grueling reality of pain and hospital visits. Maureen Dalgleish, a 65-year-old retired primary school teacher from Edinburgh, has lived with Crohn’s since her diagnosis in 1988. Over nearly four decades, the disease has forced her through four separate surgeries—in 2001, 2006, 2013, and 2025—to remove scarred portions of her bowel.

Dalgleish describes the exhaustion of living with a condition that can put your life “on hold.” Before her most recent surgery, she suffered from debilitating abdominal spasms, nausea, and fever, sometimes leading to loss of consciousness. To manage her symptoms, she has spent long periods on liquid or heavily restricted diets.
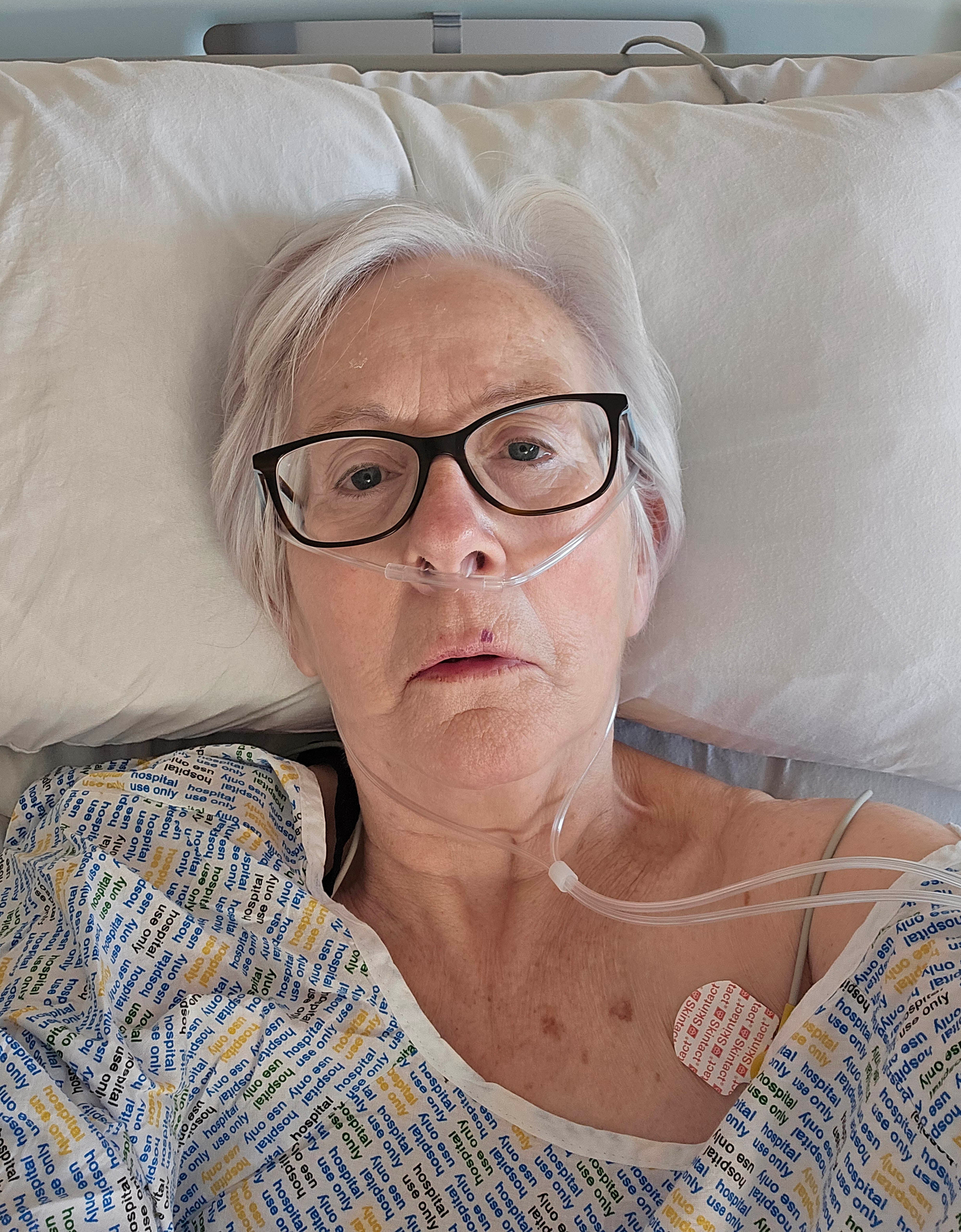
Dalgleish donated tissue from her surgery to the University of Edinburgh team, hoping the research would spare others from the same cycle of surgery and relapse. “The idea of having medication to control or stop the fibrosis would be amazing,” she said. “Although I realise it probably won’t benefit me personally, this research could potentially be a complete game-changer for others like me.”
The Path Toward New Therapies
The study, published in The Journal of Pathology, was supported by a UK-wide collaboration and funding from the Leona M and Harry B Helmsley Charitable Trust. While the discovery is in the early stages, it provides a specific molecular target that pharmaceutical researchers can now aim for.
Catherine Winsor, director of service, research and evidence at the charity Crohn’s & Colitis UK, emphasized the emotional and physical weight of this discovery. “People who live with Crohn’s often inform us how much fibrosis and scarring can affect their lives, yet it’s something current treatments don’t address,” Winsor said. “It brings real hope that, in the future, we might be able to treat not just inflammation, but the lasting damage Crohn’s can cause.”
| Focus Area | Inflammation (Current Care) | Fibrosis (Research Goal) |
|---|---|---|
| Primary Target | Overactive immune response | Excess collagen production |
| Goal | Reduce swelling and ulcers | Prevent/reverse bowel narrowing |
| Clinical Outcome | Symptom remission | Avoidance of strictures/surgery |
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Patients should consult with a healthcare provider for diagnosis and treatment of Crohn’s disease.
The next phase of this research will likely involve testing whether the identified signaling pathways can be interrupted in laboratory models before moving toward clinical trials. As researchers refine these therapeutic targets, the goal is to move beyond surgical removal of scarred tissue toward a medical intervention that stops the scarring process in its tracks.
We desire to hear from you. Have you or a loved one dealt with the challenges of Crohn’s-related fibrosis? Share your experience in the comments below.