A breast cancer diagnosis is rarely an isolated event. While the medical charts focus on tumor grade, receptor status and chemotherapy cycles, there is a parallel, invisible narrative unfolding within the home. For many women, the battle against malignancy is not fought in a vacuum, but within the complex architecture of a partnership.
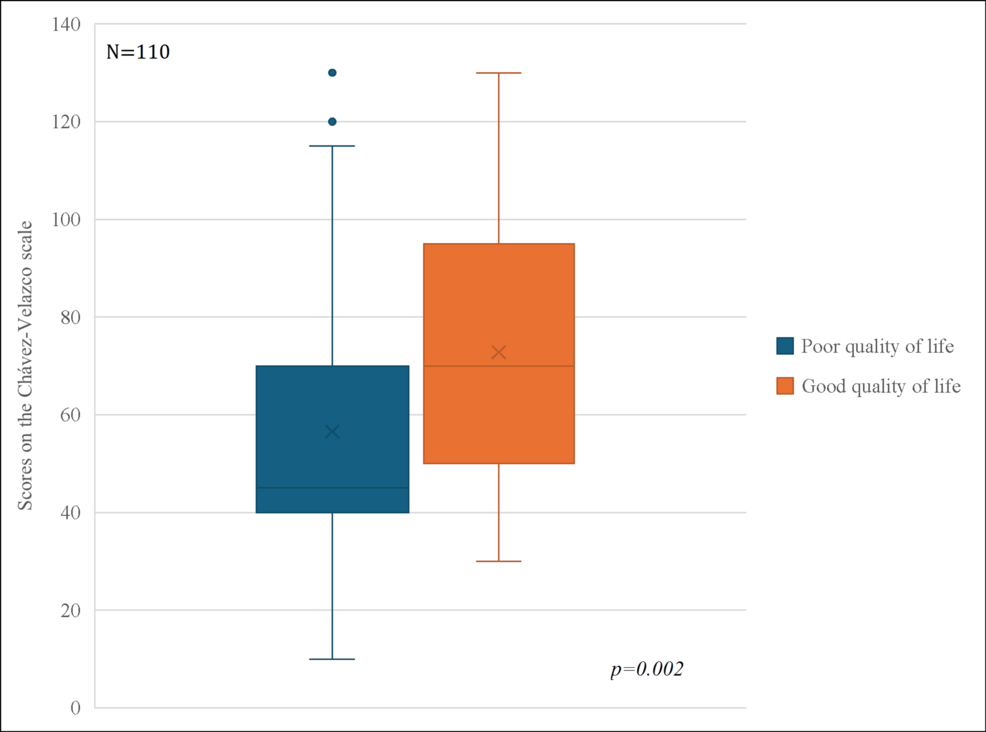
Recent research into the marital functionality and quality of life in breast cancer suggests that the health of a woman’s marriage is not merely a background detail—it is a critical determinant of her overall well-being. The data indicates a profound positive correlation between the stability and functionality of a marital relationship and the patient’s perceived quality of life, suggesting that emotional synergy at home can act as a buffer against the ravages of the disease.
As a physician, I have seen how clinical success—the shrinking of a tumor or the completion of radiation—does not always translate to a “recovered” patient. True recovery encompasses psychological, social, and emotional dimensions. When a partner provides consistent, functional support, the patient’s ability to navigate the trauma of diagnosis and the grueling nature of treatment improves significantly.
The Synergy of Support and Recovery
The “couple dimension” of cancer refers to the way a diagnosis reshapes the dynamics between partners. It is a period of extreme vulnerability where the roles of caregiver and patient blur. When marital functionality is high—characterized by open communication, mutual trust, and emotional intimacy—women tend to report lower levels of depression and anxiety.

Conversely, marital distress can exacerbate the physical and mental toll of the illness. The stress of a failing relationship creates a secondary trauma that competes for the patient’s limited emotional energy. In these cases, the home, which should be a sanctuary for healing, becomes another source of tension, potentially hindering the patient’s adherence to treatment and their overall resilience.
This relationship is not just about “being nice” to one another; it is about the practical application of psychosocial support. High-functioning couples are better equipped to manage the logistics of care, from coordinating transportation to appointments to managing the household during periods of intense fatigue. This structural support allows the patient to focus more fully on their physical recovery.
Identifying the Pillars of Marital Functionality
Research indicates that certain specific dynamics within a marriage contribute most significantly to a patient’s quality of life. These are not static traits but active behaviors that can be cultivated even after a diagnosis.
- Emotional Attunement: The ability of a partner to validate the patient’s fear and grief without attempting to “fix” it immediately.
- Adaptive Communication: Shifting how a couple talks about the illness, moving from avoidance or over-protection to honest, supportive dialogue.
- Maintenance of Intimacy: Navigating the changes in body image and sexual function that often accompany mastectomy or chemotherapy.
- Shared Coping: Approaching the cancer as a “we” problem rather than a “you” problem, which reduces the patient’s sense of isolation.
The impact of these dynamics is measurable. According to the National Cancer Institute, psychosocial interventions that target the couple rather than just the individual can lead to better long-term mental health outcomes for survivors.
Comparing Marital Dynamics in Cancer Care
| Relationship Dynamic | Typical Patient Experience | Impact on Quality of Life |
|---|---|---|
| High Functionality | Strong emotional validation, shared burden | Higher resilience, lower anxiety |
| Moderate Functionality | Inconsistent support, occasional conflict | Variable emotional stability |
| Low Functionality | Emotional isolation, increased caregiver stress | Higher risk of clinical depression |
The ‘Invisible Patient’ and the Caregiver Burden
To understand the couple dimension, we must acknowledge the partner as the “invisible patient.” While they are not the one undergoing surgery or chemotherapy, the spouse experiences a parallel trajectory of stress, fear, and exhaustion. When a spouse is overwhelmed or lacks the tools to cope, their distress often mirrors back onto the patient.
This creates a feedback loop: the patient feels guilty for being a burden, which leads to withdrawal, which in turn makes the partner feel disconnected. Breaking this cycle requires a shift in how oncology teams approach care. Rather than viewing the spouse as a mere companion or a source of history, clinicians are increasingly recognizing the need to integrate the partner into the therapeutic process.
The American Cancer Society emphasizes the importance of support systems, noting that social support is linked to better coping mechanisms and a higher likelihood of adhering to complex treatment regimens.
Moving Toward Couple-Centric Oncology
The evidence suggests that the medical community must move beyond the individual-centric model of care. If marital functionality is a primary driver of quality of life, then the “treatment” for breast cancer should include the relationship itself.
Practical steps for integrating this approach include:
- Couple-Based Counseling: Integrating therapists who specialize in medical trauma into the oncology team.
- Partner Education: Providing spouses with specific tools to communicate effectively and manage their own mental health.
- Intimacy Guidance: Addressing the sexual and physical changes of cancer treatment openly and clinically to reduce shame and disconnection.
When the partnership is fortified, the patient is not just surviving a disease; they are maintaining a life. The goal of cancer care is not merely the absence of disease, but the restoration of a functional, fulfilling existence.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Patients should consult with their healthcare provider or a licensed therapist for personalized care plans.
The next phase of integrated oncology involves the wider adoption of “couple-centric” protocols in clinical trials, focusing on how relational health impacts long-term survivorship markers. As more hospitals implement multidisciplinary psychosocial teams, the focus will likely shift toward standardized screening for marital distress as part of the initial diagnosis phase.
Do you believe healthcare providers should do more to support the partners of cancer patients? Share your thoughts and experiences in the comments below.