The global effort to eliminate guinea worm disease has reached a critical juncture, with human cases plummeting to a historic low of just 10 cases in 2023. For decades, the campaign has operated on a singular, ambitious goal: to craft this debilitating parasite the second human disease in history to be completely eradicated.
Since the World Health Organization certified the eradication of smallpox in 1980, no other human illness has been entirely wiped from the earth. The pursuit of a second eradication represents one of the most challenging frontiers in public health, requiring a combination of rigorous surveillance, behavioral change, and an understanding of complex biological reservoirs.
As a physician, I have seen how “neglected tropical diseases” often fall through the cracks of global funding. However, the fight against Dracunculiasis—the medical term for guinea worm—is unique because there is no vaccine and no medicine to cure the infection. The only way to stop the disease is to break the cycle of transmission by preventing people from drinking contaminated water.
The Mechanics of a Persistent Parasite
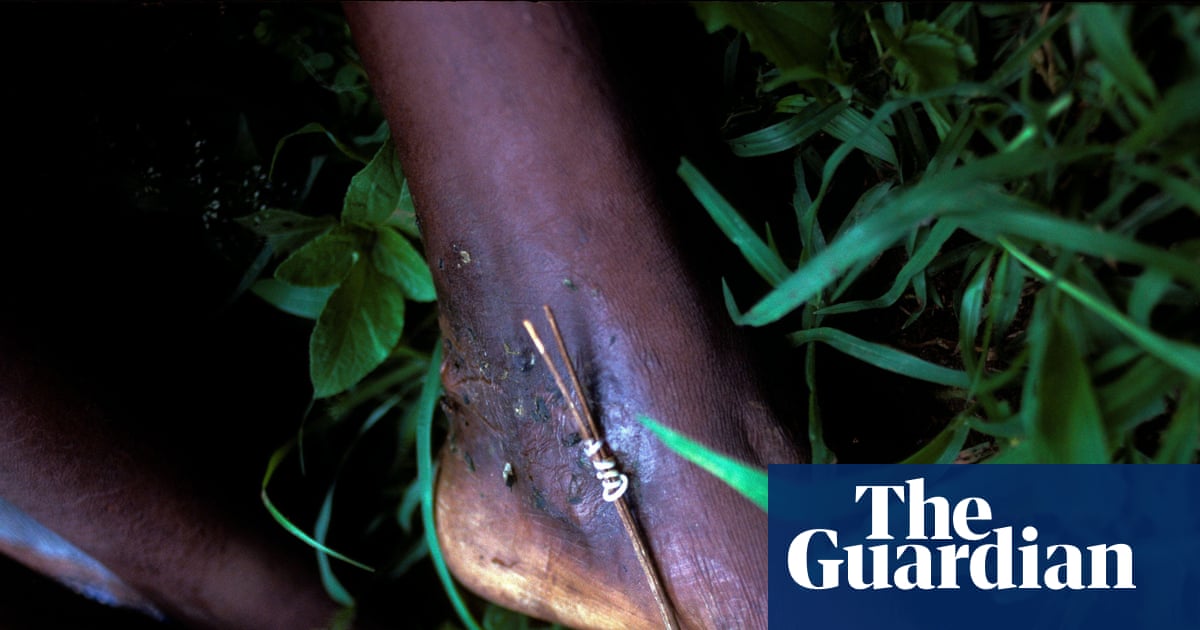
Guinea worm is caused by a nematode parasite that enters the human body when a person drinks water containing microscopic water fleas (copepods) infected with larvae. Over the course of a year, the worm matures and migrates through the body. When the female worm is ready to release its larvae, it creates a painful blister, typically on the lower leg, and emerges slowly over several weeks.

The debilitating nature of the disease is not just the pain of the worm’s exit, but the secondary infections that often occur. Because the process is so unhurried, victims are often unable to work or attend school for months, trapping families in cycles of poverty. The transmission cycle is completed when the infected person submerges the blister in water to soothe the burning sensation, releasing the larvae back into the environment to be eaten by water fleas.
According to David Molyneux, emeritus professor of tropical disease microbiology at the Liverpool School of Tropical Medicine, the difficulty of final eradication lies in the “last mile.” While millions of people are no longer at risk, the remaining pockets of infection are often in conflict-prone or remote regions where health workers struggle to maintain consistent surveillance.
Why Eradicating Guinea Worm is Not Like Smallpox
To understand why we haven’t yet seen a second eradication, it is helpful to compare the biological and logistical hurdles of guinea worm against those of smallpox. Smallpox was a virus with no animal reservoir; once it was gone from humans, it was gone from the world. Guinea worm, however, has presented a surprising biological twist.
In recent years, researchers discovered that the parasite could infect animals, particularly dogs in Chad. This “animal reservoir” complicates the mission significantly. If the parasite can survive and circulate in canine populations, the risk of spillover back into humans remains a constant threat, even if every single human case is treated and contained.
| Feature | Smallpox (Eradicated) | Guinea Worm (In Progress) |
|---|---|---|
| Preventative Tool | Effective Vaccine | Water Filtration/Education |
| Animal Reservoir | None | Present (e.g., Dogs) |
| Transmission | Respiratory/Contact | Water-borne (Copepods) |
| Detection | Visible Rash | Delayed (1-year incubation) |
The Role of the Carter Center and Global Strategy
The decline of the disease is largely attributed to the work of the Carter Center, founded by former U.S. President Jimmy Carter. Their strategy has not relied on high-tech medicine, but on grassroots public health: distributing cloth filters to strain out water fleas, digging deeper boreholes for clean water, and providing cash incentives for people to report their infections.
This approach targets the environmental root of the problem. By educating communities on how the parasite spreads, the program has successfully shifted the behavior of millions. However, as the number of cases drops into the single digits, the cost and effort required to find and contain one single case increase exponentially.
The strategy now involves intensive “case containment,” where health workers ensure that an infected person does not enter any water source until the worm has completely emerged. This requires a level of trust and cooperation between local populations and international health agencies that can be fragile in unstable political climates.
The Stakeholders in the Final Push
- Affected Communities: Primarily in sub-Saharan Africa, where the burden of disease remains.
- The Carter Center: Leading the operational coordination and funding of the eradication effort.
- WHO and National Ministries of Health: Providing the official certification and regulatory framework for eradication.
- Research Institutions: Like the Liverpool School of Tropical Medicine, which study the parasite’s evolution and animal reservoirs.
The Path Forward: Can We Reach Zero?
The question of whether we can eradicate a second human disease depends on our ability to address the animal-human interface. If the parasite continues to circulate in dogs and other wildlife, the goal may shift from “eradication” (complete extinction of the parasite) to “elimination” (reducing human cases to zero or near-zero).
Despite these hurdles, the momentum is undeniable. The drop from millions of cases in the 1980s to just 10 in the last year is a testament to the power of focused public health interventions. The biological challenge of animal reservoirs is a new variable, but it is one that scientists are actively working to manage through veterinary surveillance and targeted interventions.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Please consult a healthcare provider for medical concerns or diagnosis.
The global health community continues to monitor case reports closely, with the next major milestone being the continued suppression of human cases throughout 2024 and 2025 to determine if the animal-to-human transmission can be effectively blocked. Official updates on case counts are typically released annually by the Carter Center and the World Health Organization.
Do you believe the focus should remain on total eradication or shift toward containment? Share your thoughts in the comments below.