Dietary choices are often discussed in terms of long-term outcomes—decades of habit leading to chronic illness. However, latest research suggests that the biological impact of what we eat can manifest far more rapidly. A study from Brigham and Women’s Hospital (General de Massachusetts Brigham) has revealed that a dieta alta en grasas debilita la defensa intestinal in a matter of days, compromising one of the body’s most critical barriers against external pathogens.
The findings, published in the journal Immunity, indicate that brief periods of high fat intake can trigger a selective and rapid decline in specific immune cells. This depletion renders the intestinal mucosa more permeable, essentially “opening the door” for harmful substances to enter the bloodstream and trigger systemic inflammation.
The Role of ILC3s: The Gut’s First Line of Defense
The human intestine is not merely a digestive organ; it is a powerhouse of the immune system. Approximately 70% of the body’s defense cells are concentrated in the gut, tasked with distinguishing between harmless nutrients and dangerous pathogens.

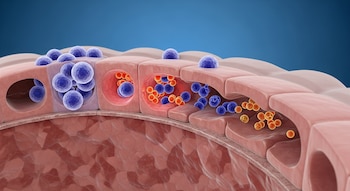
The researchers focused their investigation on Group 3 innate lymphoid cells, known as ILC3s. These cells act as biological “guardians,” maintaining the integrity of the intestinal wall and secreting vital molecules that prevent microorganisms from leaking into the body’s internal environment.
The study found that when exposed to a high-fat diet, the population of ILC3s dropped significantly and rapidly. According to researcher Selma Boulenouar, this reduction was both quick and selective. While other immune cells, such as Th17 cells, remained stable, the ILC3s showed a particular sensitivity to the excess of fats, disappearing far sooner than the team had expected.

From Permeability to Systemic Inflammation
The loss of ILC3s creates a ripple effect in the gut’s chemistry. Specifically, it leads to a reduction in the production of IL-22, a signaling molecule essential for maintaining the mucosal lining of the intestine. Without sufficient IL-22, the intestinal barrier loses its efficacy, becoming more permeable.
In medical terms, What we have is often referred to as a “leaky” barrier. When the wall is compromised, substances that should be excreted instead leak into the surrounding tissues, activating inflammatory processes. While high-fat diets have long been linked to obesity and colorectal cancer, this research highlights a critical timeline: the damage begins almost immediately, long before clinical symptoms of chronic disease appear.
The Metabolic Link and the Role of Microbiota
To uncover the “how” behind this rapid decline, scientists utilized animal models and human intestinal tissue samples. By employing advanced genetic analysis and cellular metabolism studies, the team looked closely at the mitochondria—the energy-producing structures within cells.
They discovered that the gut microbiota, the vast community of microorganisms living in the intestine, plays a pivotal role. Certain inflammatory signals produced by the microbiota interfere with the way ILC3s process fats. When these cells cannot effectively metabolize the excess lipids, their function is impaired, eventually leading to their disappearance.
The Path to Recovery: Is the Damage Permanent?
Perhaps the most encouraging finding of the study is that this immune depletion is not necessarily permanent. The researchers observed that when the subject returned to a balanced diet, the affected cells began to recover, and the protective function of the intestinal barrier was restored.
This suggests a window of opportunity for intervention. By adjusting dietary habits before long-term chronic inflammation sets in, individuals may be able to “reset” their intestinal defenses.

Disclaimer: This article is for informational purposes only and does not constitute medical advice. Please consult a healthcare provider for personalized dietary and health recommendations.
The research team at Brigham and Women’s Hospital has emphasized that while these results are promising, the next critical step involves moving from animal models and tissue samples to broader clinical trials. These future studies will be essential to confirm how these mechanisms operate across diverse human populations and to determine if targeted metabolic therapies can help restore the intestinal barrier in patients with existing digestive disorders.
We aim for to hear from you. Do you believe dietary changes can be felt in days, or do you view health as a long-term accumulation? Share your thoughts in the comments and share this article with your network.

