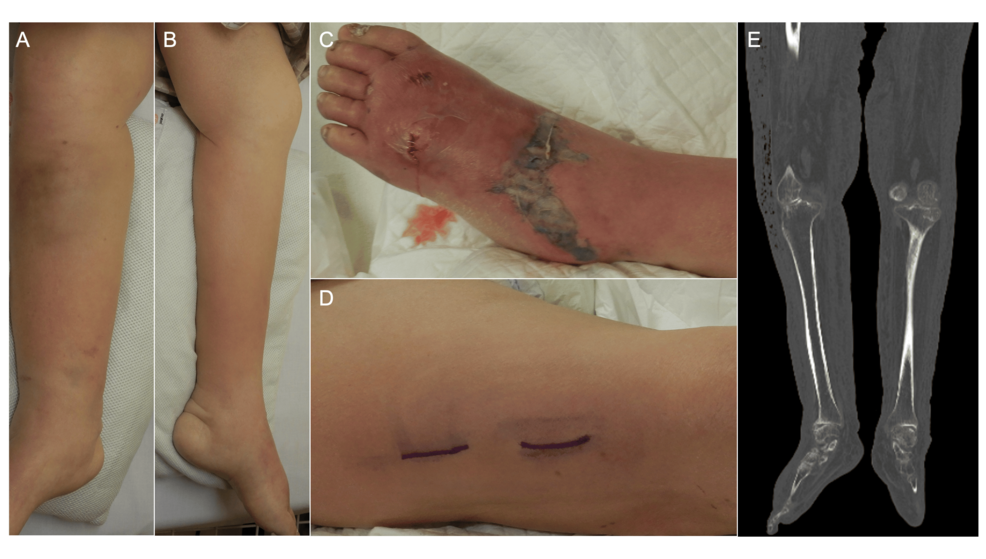
A rare and aggressive skin infection has highlighted the precarious balance of health for organ transplant recipients, specifically those managing the long-term effects of immunosuppression. A recent clinical case detailed a patient who developed bilateral lower extremity necrotizing fasciitis, a “flesh-eating” infection that rapidly destroys the soft tissue and fascia of the legs, caused by a highly resistant strain of bacteria.
The infection was driven by Extended-Spectrum Beta-Lactamase (ESBL)-producing Escherichia coli. While E. Coli is common in the human gut, the ESBL-producing variety is significantly more dangerous due to the fact that it produces enzymes that neutralize many of the most common antibiotics used in hospitals, including penicillins and cephalosporins. For a patient who has undergone a liver transplant, the risk of such an infection is compounded by the necessary medications used to prevent organ rejection, which simultaneously weaken the body’s ability to fight off opportunistic pathogens.
This specific case of bilateral lower extremity necrotizing fasciitis caused by ESBL-producing E. Coli serves as a critical reminder for clinicians of the need for rapid surgical intervention and targeted antimicrobial therapy when treating immunocompromised patients. The simultaneous involvement of both legs is an uncommon presentation that underscores the systemic vulnerability of the patient.
The progression of necrotizing fasciitis is notoriously swift. In this instance, the infection moved through the deep fascia—the connective tissue surrounding muscles and nerves—effectively cutting off blood supply to the skin and underlying tissues. Because the patient was a liver transplant recipient, the typical inflammatory response that alerts doctors to an infection was muted, potentially masking the severity of the condition during the earliest stages.
The Challenge of Antibiotic Resistance in Transplant Patients
The presence of ESBL-producing bacteria represents a growing challenge in global public health. These enzymes allow the bacteria to survive exposure to a wide array of beta-lactam antibiotics, which are the backbone of many hospital treatment protocols. When these resistant strains enter the bloodstream or deep tissues of a patient with a suppressed immune system, the window for successful treatment narrows significantly.
In the case of the liver transplant recipient, the medical team had to navigate a complex therapeutic path. Standard antibiotics were insufficient; instead, the treatment required “carbapenems,” a class of potent, broad-spectrum antibiotics often reserved as a last line of defense to prevent the further development of resistance. The Centers for Disease Control and Prevention (CDC) emphasizes that managing healthcare-associated infections in transplant patients requires a multidisciplinary approach combining infectious disease expertise with aggressive surgical care.
The patient’s history of a liver transplant meant they were likely on a regimen of corticosteroids or calcineurin inhibitors. While these drugs are life-saving for the organ, they hinder the migration of white blood cells to the site of an infection and dampen the fever response, which can lead to a dangerous delay in diagnosis.
Surgical Intervention and Clinical Management
Necrotizing fasciitis cannot be cured by antibiotics alone. Because the infection causes tissue death (necrosis) and disrupts blood flow, antibiotics cannot reach the center of the infected area. The primary treatment is surgical debridement—the physical removal of all dead and infected tissue until healthy, bleeding tissue is reached.

In this bilateral case, the surgical team had to perform extensive procedures on both lower extremities. The goal of these surgeries is twofold: to stop the spread of the bacteria and to remove the necrotic “fuel” that allows the infection to persist. The process often involves multiple trips to the operating room over several days as surgeons return to ensure no residual infection remains.
The clinical management of this patient followed a rigorous sequence of events:
- Initial Presentation: Identification of skin discoloration and systemic instability.
- Diagnostic Confirmation: Use of imaging and tissue cultures to identify the ESBL-producing E. Coli.
- Emergency Debridement: Immediate surgical removal of necrotic tissue from both legs.
- Targeted Therapy: Administration of carbapenems based on the bacteria’s sensitivity profile.
- Wound Care: Long-term management of the resulting open wounds and potential skin grafting.
Comparative Risks in Immunocompromised Patients
| Factor | Standard Patient | Transplant Recipient |
|---|---|---|
| Immune Response | Strong inflammatory markers | Muted/Delayed response |
| Bacterial Vulnerability | Often susceptible to common antibiotics | Higher risk of resistant (ESBL) strains |
| Progression Speed | Rapid | Accelerated due to lack of defenses |
| Recovery Timeline | Standard wound healing | Prolonged healing due to immunosuppressants |
Broader Implications for Public Health
This case highlights a broader trend in the rise of “superbugs” within hospital environments. The World Health Organization (WHO) has identified antimicrobial resistance as one of the top global public health threats. When common bacteria like E. Coli evolve to resist multiple drugs, routine procedures—including organ transplants—become significantly riskier.
For patients and caregivers, the takeaway is the importance of vigilance. Any sign of skin redness, warmth, or unusual pain in a transplant recipient should be treated as a potential emergency. Early detection is the single most critical factor in preventing the need for extensive amputation or the onset of septic shock.
Medical professionals are encouraged to maintain a high index of suspicion for necrotizing fasciitis in patients with comorbidities like diabetes or those on immunosuppressive therapy, even if the patient does not present with a high fever. The absence of a typical “sick” appearance can be deceptive in the presence of medications that suppress the body’s natural warning signals.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
The medical community continues to monitor the prevalence of ESBL-producing organisms to refine stewardship protocols and develop new antimicrobial agents. Future updates on antibiotic resistance guidelines from the Infectious Diseases Society of America (IDSA) will likely provide further direction on the management of these complex infections.
We invite readers to share their experiences with transplant recovery or questions about antibiotic resistance in the comments below.