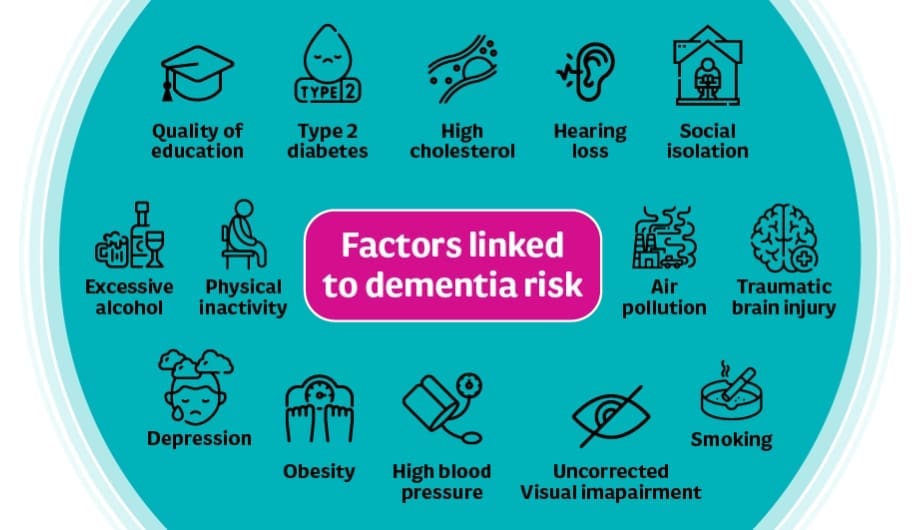
For decades, the medical community has known that smoking damages the lungs and the heart. But latest research is revealing a more complex and unsettling connection: a biological “bridge” between the lungs and the brain that may explain why smoking and dementia risk are so closely linked.
The discovery centers on lung exosomes—tiny, messenger-like vesicles released by cells—that can travel through the bloodstream and cross the blood-brain barrier. According to recent findings, smoking triggers the release of these exosomes, which then enter the brain and disrupt the delicate balance of iron, a process that can trigger neurodegeneration long before a patient shows the first sign of memory loss.
As a physician, I have often seen how systemic inflammation from smoking affects various organs, but the concept of a “lung-brain axis” provides a specific mechanical explanation for cognitive decline. This pathway suggests that the damage caused by tobacco isn’t just a result of reduced oxygen or vascular disease, but a direct biochemical interference with how the brain manages essential minerals.
The mechanism of the lung-brain axis
To understand how a habit in the lungs affects the mind, one must first understand exosomes. These are small extracellular vesicles that carry proteins, lipids, and RNA between cells. They act as a cellular communication system, allowing one organ to “signal” another.
In smokers, the lungs produce a specific profile of these exosomes. Once these vesicles reach the brain, they interfere with iron homeostasis—the process by which the brain regulates the absorption and storage of iron. While iron is critical for neuronal health and myelin production, too much of it in the wrong place is toxic.
When iron balance is disrupted, it can lead to the production of reactive oxygen species, causing oxidative stress. This stress damages neurons and promotes the accumulation of proteins associated with dementia, such as amyloid-beta and tau. This progression creates a fertile environment for neurodegenerative diseases to grab root, effectively priming the brain for decline.
A ‘triple threat’ appearing decades early
One of the most concerning aspects of this research is the timeline. The biochemical shifts in the brain—specifically the iron imbalance and the influx of lung-derived exosomes—can commence decades before clinical symptoms of dementia manifest. This suggests that the “damage” is not an acute event but a unhurried, cumulative erosion of cognitive reserve.
Scientists are now identifying what some describe as a “triple threat” of risk factors that converge to accelerate this process. While the specific combination can vary, it generally involves the synergy of chronic smoking, age-related metabolic decline, and pre-existing vascular vulnerabilities. When these three factors overlap, the brain’s ability to clear toxins and regulate minerals is severely compromised.
This early window of dysfunction presents a critical opportunity for intervention. If iron imbalance can be detected via biomarkers before cognitive impairment begins, it may be possible to implement protective strategies far earlier than is currently standard in geriatric care.
Comparing the impact of smoking on brain health
| Mechanism | Primary Action | Timing of Effect | Primary Result |
|---|---|---|---|
| Vascular Damage | Reduced blood flow/stroke | Acute or chronic | Ischemic tissue death |
| Exosomal Transport | Disrupts iron homeostasis | Decades-long progression | Neurodegenerative protein buildup |
| Systemic Inflammation | Increases blood-brain permeability | Continuous | General neuroinflammation |
What this means for prevention and diagnosis
The identification of lung exosomes as a driver of dementia risk shifts the conversation from general “wellness” to specific biological targets. For those currently smoking, the data reinforces that cessation is not just about preventing lung cancer or heart disease, but about protecting the structural integrity of the brain.
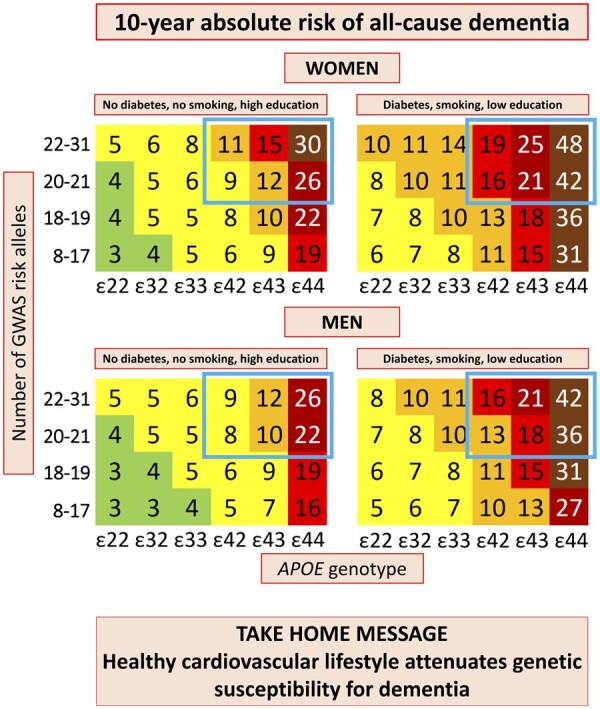
From a diagnostic perspective, this research opens the door to using exosomes as “liquid biopsies.” If clinicians can identify specific lung-derived exosomes in the blood that are known to disrupt brain iron, they may be able to screen high-risk individuals for dementia risk years before a cognitive test would present a deficit.
However, iron imbalance is a contributing factor, not the sole cause of dementia. The National Institute on Aging notes that dementia is typically the result of a complex interplay of genetics, environment, and lifestyle. The lung-exosome pathway is a significant piece of the puzzle, but it works in tandem with other risks.
The path forward in neuroprotection
The next phase of research will likely focus on whether the brain’s iron balance can be restored or if the transport of these harmful exosomes can be blocked. Researchers are investigating whether specific inhibitors can prevent lung exosomes from crossing the blood-brain barrier or if antioxidant therapies can mitigate the oxidative stress caused by iron accumulation.
For the general public, the most immediate application of this science is the reinforcement of smoking cessation. The brain’s plasticity means that reducing the influx of harmful signals can slow the progression of damage, even in middle age.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
Further studies are expected to refine the specific biomarkers used to track lung-brain communication, with upcoming clinical trials focusing on the efficacy of iron-regulating compounds in high-risk smokers. We will continue to monitor these developments as they move toward clinical application.
Do you have questions about how lifestyle factors impact long-term brain health? Share this article and join the conversation in the comments below.