As temperatures climb across New England, health officials are warning that the window for tick-borne illness is opening. While a relatively cool spring may have delayed the initial surge, the risk remains high as more people head outdoors for the season. The danger is often invisible; spring ticks are typically in their nymph stage, making them significantly smaller and harder to detect than the adult ticks seen in late summer.
The primary concern for residents in regions like Massachusetts is the blacklegged tick, commonly known as the deer tick. This species is a prolific vector for several pathogens, most notably the bacteria that cause Lyme disease, as well as babesiosis and anaplasmosis. According to health experts, these three infections are relatively common, together accounting for roughly 10,000 cases annually in Massachusetts alone.
While nature provides essential mental and physical health benefits, the intersection of human activity and tick habitats creates a persistent public health challenge. Understanding the specific health risks of tick bites is the first step in mitigating the impact of these seasonal pests, as symptoms can range from mild, unnoticed rashes to severe, flu-like illnesses.
The risk is not confined to deep woods. While ticks thrive in leaf litter, tall grass, and bushes—particularly in areas frequented by deer and mice—they are increasingly prevalent in residential backyards, public parks, and hiking trails. Public health officials emphasize that even beach areas can be dangerous, noting that unless one is standing on a concrete surface in a city center, ticks should remain a primary consideration during outdoor excursions.
The Spectrum of Tick-Borne Pathogens
While Lyme disease remains the most frequent diagnosis, a diversifying range of threats is emerging. The blacklegged tick can also transmit Borrelia miyamotoi and the Powassan virus. The latter is particularly concerning to medical professionals because, unlike most tick-borne infections, it can cause serious neurological damage and is rarer in its response to standard treatments.
the expansion of the lone star tick—driven in part by climate change—has introduced a different kind of risk: alpha-gal syndrome. This is a tick-triggered allergy to red meat and other animal products. The condition is notoriously difficult to diagnose because the allergic reaction typically occurs two to 10 hours after eating, rather than immediately. Symptoms can range from gastrointestinal distress to severe anaphylaxis, sometimes requiring the utilize of an EpiPen.
| Pathogen/Condition | Associated Tick | Primary Impact |
|---|---|---|
| Lyme Disease | Blacklegged (Deer) Tick | Joint pain, rash, flu-like symptoms |
| Powassan Virus | Blacklegged (Deer) Tick | Potential neurological damage |
| Alpha-gal Syndrome | Lone Star Tick | Allergy to red meat/animal products |
| Babesiosis/Anaplasmosis | Blacklegged (Deer) Tick | Severe flu-like illness |
In response to the rise of alpha-gal syndrome, Massachusetts has recently begun tracking the allergy more rigorously, requiring physicians to report cases to the Department of Public Health to better understand the geographic spread, particularly on Cape Cod and the Islands.
Proven Prevention and Field Response
The most effective way to manage the health risks of tick bites is to prevent the attachment entirely. Dr. Jacob Lemieux, an infectious disease physician at Mass General Brigham, suggests a combination of chemical barriers and physical protection. This includes using EPA-approved repellents containing DEET on the skin and treating clothing with permethrin, a compound that can kill ticks on contact.
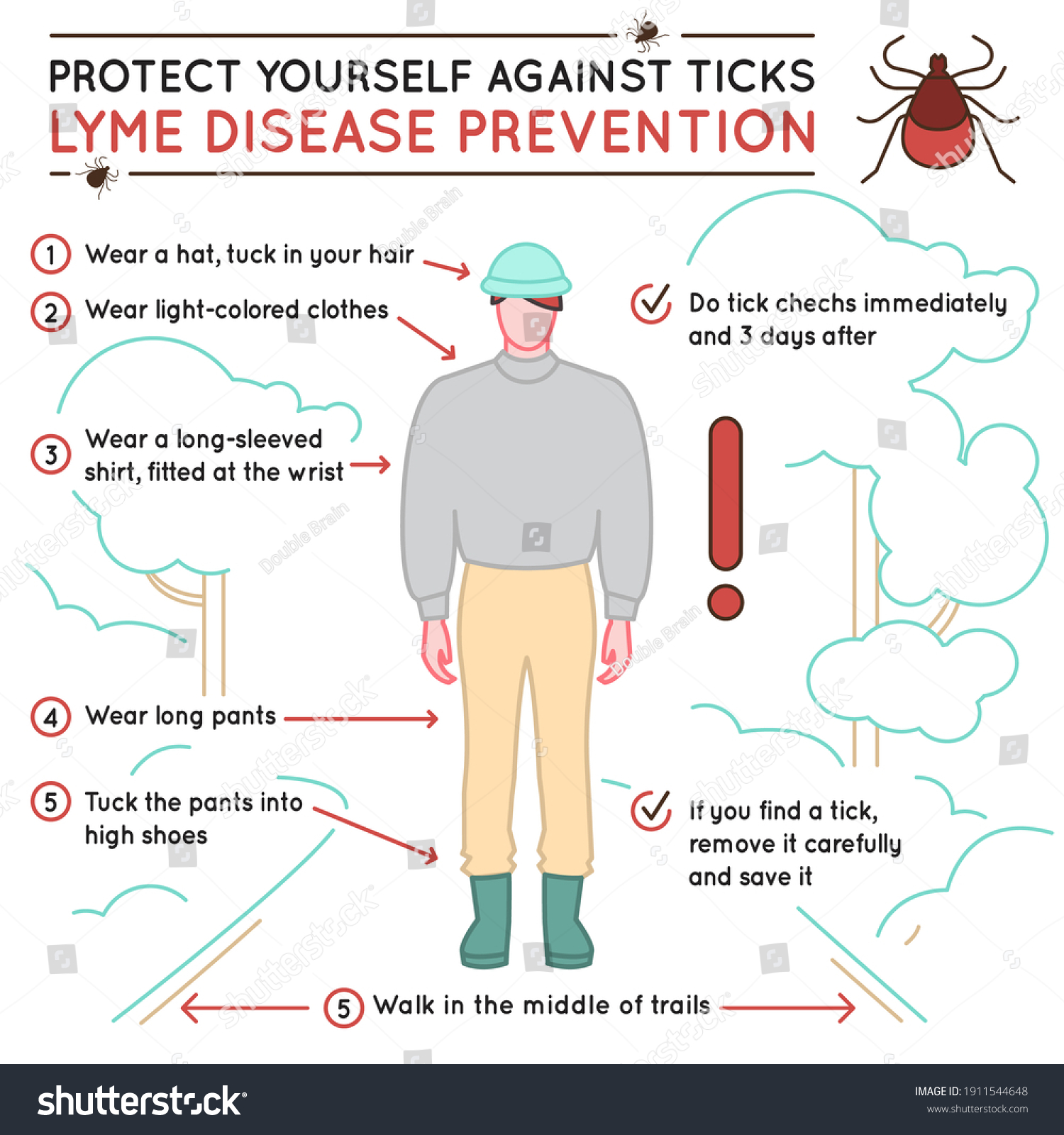
Physical barriers, such as wearing long sleeves and tucking pants into socks, further reduce the available surface area for ticks to attach. Once indoors, the process of “de-ticking” is critical. Experts recommend a prompt shower and a full-body check. A crucial, often overlooked detail is the use of a dryer: while a washing machine may not kill ticks, tossing clothes in the dryer on high heat for 10 minutes is effective at eliminating hitchhikers.
If a tick is discovered attached to the skin, speed and technique are paramount. The recommended method is to use fine-tipped tweezers to grasp the tick as close to the skin as possible and pull steadily upward. It’s vital not to twist or crush the tick, as this can increase the risk of pathogens being pushed into the bloodstream. Following removal, the area should be cleaned and monitored for several weeks for signs of fever, fatigue, or the characteristic “bullseye” rash.
The Future of Tick Prevention
While awareness and prevention are the current gold standards, medical research is moving toward pharmaceutical interventions. Clinical trials are currently exploring new tools, including a monoclonal antibody developed by the UMass Chan School for seasonal prevention of Lyme disease. A vaccine developed by Pfizer and Valneva showed a reduction in cases by approximately 73 percent during a Phase 3 trial.
Despite these advancements, the immediate focus remains on coexistence and vigilance. The seasonal peak for tick-borne diseases typically occurs between June and August, though the threat begins as early as April. For those experiencing unusual symptoms after a bite—or unexpected reactions after eating red meat—contacting a healthcare provider immediately is the recommended course of action.
Disclaimer: This article is provided for informational purposes only and does not constitute professional medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
Public health departments will continue to monitor tick populations and report infection rates throughout the summer. The next major data update on alpha-gal syndrome tracking is expected as the Department of Public Health compiles reports from clinicians through the complete of the year.
We invite readers to share their experiences with tick prevention or ask questions in the comments below to help our community stay safe this season.

