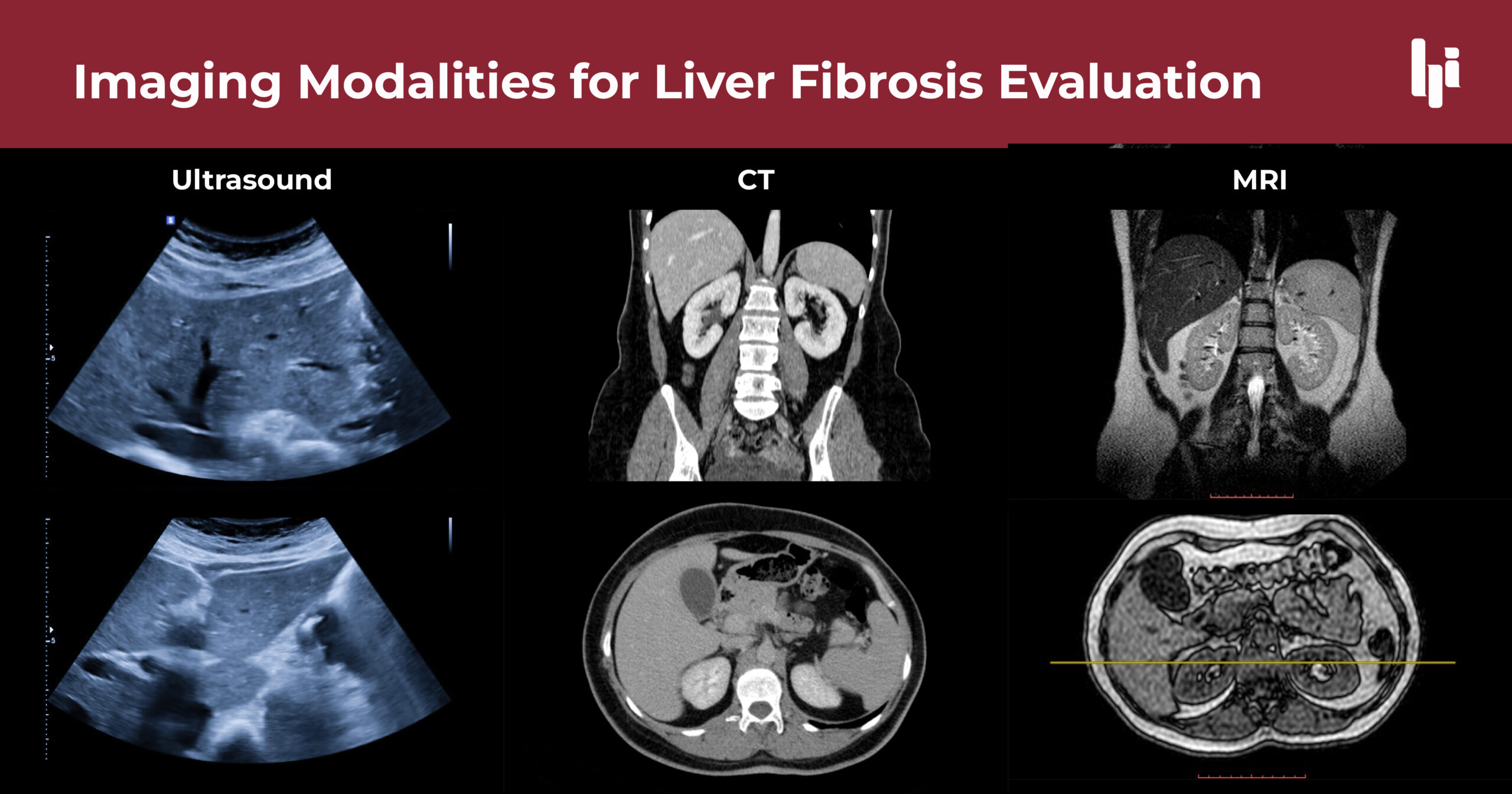
A significant portion of the European population is living with undiagnosed liver fibrosis, a condition where the liver develops scar tissue that can eventually lead to permanent organ failure. According to the findings of the LiverScreen project, a comprehensive multinational cohort study, this silent progression of liver disease is more prevalent in the general population than previously recognized, often remaining undetected until the damage is advanced.
The study identifies a critical gap in current healthcare screening, revealing that many individuals with significant liver scarring have no prior diagnosis. This lack of awareness is particularly concerning because liver fibrosis is often asymptomatic in its early and middle stages. By the time a patient presents with clinical symptoms, the window for the most effective interventions may have already closed.
As a physician, I have seen how metabolic dysfunction and lifestyle factors create a “perfect storm” for liver injury. The LiverScreen data underscores that the prevalence of liver fibrosis in the general population is primarily driven by two intersecting crises: the rise of metabolic dysfunction-associated steatotic liver disease (MASLD) and the long-term effects of alcohol consumption.
The implications of these findings are clear: shifting the diagnostic focus from symptomatic patients to at-risk populations could prevent thousands of cases of cirrhosis and liver cancer. Early detection allows for personalized medical and lifestyle interventions that can not only halt the progression of fibrosis but, in many cases, allow the liver to regenerate and heal.
The Drivers of Silent Liver Damage
The LiverScreen project highlights that the surge in liver fibrosis is not random but closely tied to systemic health trends across Europe. The primary drivers identified are metabolic factors—including obesity, type 2 diabetes, and hypertension—and alcohol use. When the liver is repeatedly injured by these factors, it attempts to repair itself, creating scar tissue (fibrosis) in the process.
Metabolic-associated liver disease has become a global epidemic, mirroring the rise in metabolic syndrome. When excess fat accumulates in the liver, it can trigger inflammatory responses that accelerate scarring. This process is often invisible on standard blood tests, meaning a patient might have “normal” liver enzyme levels although their liver architecture is actively being compromised.
Alcohol consumption remains a potent catalyst. The study emphasizes that the interaction between alcohol and metabolic dysfunction often compounds the risk, accelerating the transition from simple fatty liver to advanced fibrosis. This synergy makes the general population more vulnerable than previously estimated, as many individuals fall into both high-risk categories without realizing the cumulative impact on their hepatic health.
Understanding the Stages of Liver Injury
To understand why the LiverScreen project is so pivotal, It’s necessary to distinguish between the different stages of liver damage. Fibrosis is a spectrum, and the goal of early screening is to catch the disease before it reaches the point of no return.
| Stage | Description | Reversibility |
|---|---|---|
| Steatosis | Accumulation of fat in liver cells. | Highly Reversible |
| Fibrosis (Early/Mod) | Development of scar tissue; liver function remains stable. | Potentially Reversible |
| Cirrhosis | Extensive scarring; liver architecture is distorted. | Difficult/Irreversible |
| Liver Failure | Loss of essential liver functions; high risk of malignancy. | Requires Transplant |
The Challenge of Early Detection
The “silent” nature of liver fibrosis is the primary hurdle to public health. Traditional screening methods often rely on liver function tests (LFTs), but these can be misleading. A person can have advanced fibrosis without elevated enzymes, leading to a false sense of security for both the patient and the clinician.
The LiverScreen project advocates for a more proactive approach to screening. By utilizing non-invasive tools—such as transient elastography (FibroScan) or validated biomarkers—healthcare providers can identify scarring before it evolves into cirrhosis. These tools allow clinicians to “see” the stiffness of the liver without the need for an invasive biopsy, which has historically been the gold standard but is fraught with risks and patient reluctance.
The study suggests that integrating these screenings into routine care for patients with metabolic risk factors—such as those with a high BMI or diagnosed diabetes—could fundamentally change the trajectory of liver disease management in Europe. Instead of treating end-stage failure, the medical community can move toward a model of preventative maintenance.
Pathways to Personalized Intervention
Once fibrosis is detected early, the focus shifts to personalized intervention. The LiverScreen project emphasizes that the treatment for a patient with alcohol-driven fibrosis differs significantly from one driven by metabolic dysfunction, though the goals remain the same: stop the injury and reduce the scar tissue.
For those with metabolic-driven disease, interventions focus on aggressive weight management, glycemic control, and dietary changes. For those affected by alcohol, cessation is the primary requirement for stabilization. When these interventions are implemented early, the liver’s remarkable capacity for regeneration can be leveraged to reverse early-stage fibrosis.
The broader public health goal is to create a screening pipeline that identifies “at-risk” individuals through primary care, moves them to specialized non-invasive testing, and then places them on a tailored management plan. This systemic approach would reduce the burden on tertiary care centers and decrease the number of patients requiring emergency liver transplants.
For more detailed information on liver health and screening guidelines, the European Association for the Study of the Liver (EASL) provides comprehensive clinical practice guidelines for healthcare professionals and patients.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
The next phase of research stemming from the LiverScreen project will focus on refining the specific biomarkers that can most accurately predict the rate of fibrosis progression in diverse populations. These updates are expected to inform updated screening protocols across European health ministries in the coming years.
Do you believe liver health should be part of a standard annual check-up? Share your thoughts in the comments below or share this article with someone who may be at risk.