Understanding the specific manifestations of cerebral palsy in children is critical for developing targeted rehabilitation strategies, particularly in rapidly evolving healthcare hubs. A detailed retrospective study conducted at tertiary referral hospitals in Dubai, United Arab Emirates, has provided a comprehensive look at the clinical patterns of cerebral palsy in pediatric patients from 2018 to 2020, offering a blueprint for how the region manages this complex neurological condition.
Cerebral palsy (CP) remains one of the most common motor disabilities in childhood, characterized by permanent disorders of movement and posture. Because the condition often involves a constellation of comorbidities—ranging from cognitive impairments to sensory deficits—the data from Dubai’s specialized centers highlights the necessity of a multidisciplinary approach to care.
The study focused on children referred to high-level care facilities, where the complexity of cases typically requires advanced diagnostic tools and specialized therapy. By analyzing the patient population over a three-year window, researchers were able to categorize the dominant types of CP and identify the most frequent associated health challenges, providing a clearer picture of the pediatric burden in the UAE.
As a physician and medical writer, I recognize that the value of such regional data lies in its ability to bridge the gap between global clinical guidelines and local patient needs. When clinicians understand the prevailing clinical patterns of cerebral palsy in pediatric patients, they can better allocate resources for physical therapy, speech pathology, and orthopedic interventions.
Dominant Clinical Classifications and Motor Patterns
The study categorized patients based on the primary type of movement disorder. In pediatric neurology, these are generally divided into spastic, dyskinetic, and ataxic patterns. Spastic cerebral palsy, characterized by hypertonia and stiff muscles, typically represents the most common form encountered in clinical settings, often affecting the legs (diplegia) or one side of the body (hemiplegia).
The Dubai data underscores a prevalence of spasticity, which often necessitates early intervention with stretching, bracing, and in some cases, pharmacological management to prevent permanent joint contractures. The distribution of these patterns helps hospitals determine whether to prioritize gait-training equipment or upper-limb dexterity tools in their procurement cycles.
Beyond the motor type, the study evaluated the functional severity of the condition. Here’s often measured using standardized scales such as the Gross Motor Function Classification System (GMFCS), which ranks children from Level I (walking without limitations) to Level V (transported in a manual wheelchair). The findings from the tertiary centers indicate a significant concentration of patients requiring moderate to high levels of support, reflecting the nature of referral hospitals as destinations for the most severe cases.
Common Comorbidities and Associated Challenges
Cerebral palsy rarely exists in isolation. The retrospective analysis identified a high frequency of “co-occurring conditions” that complicate the clinical picture and require integrated care pathways. These comorbidities often dictate the quality of life for the child and the level of stress placed on the caregiver.
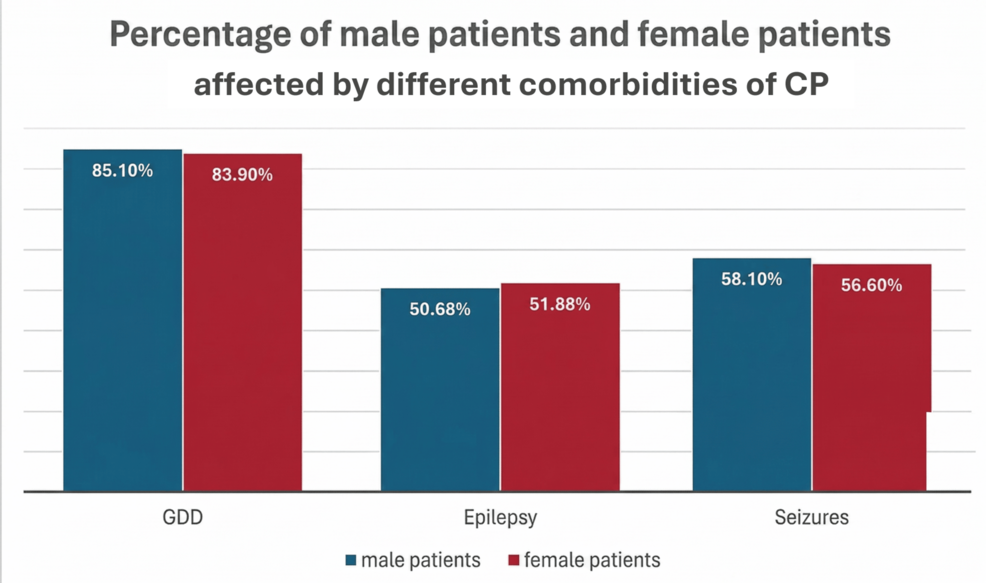
Among the most frequent associations identified in the Dubai cohort were epilepsy and intellectual disabilities. The presence of seizures often requires a delicate balance of medication to control neurological activity without inducing excessive sedation, which could otherwise hinder the child’s progress in physical therapy.
Other significant patterns emerged in the form of sensory and nutritional deficits:
- Visual and Hearing Impairments: A notable percentage of patients exhibited cortical visual impairment or hearing loss, necessitating the involvement of ophthalmologists and audiologists.
- Feeding and Swallowing Difficulties: Dysphagia, or difficulty swallowing, was a recurring theme, often leading to nutritional deficiencies or the need for enteral feeding tubes.
- Orthopedic Complications: As children grow, the mismatch between muscle tension and bone growth often leads to hip dislocations or scoliosis.
Summary of Clinical Findings (2018-2020)
| Category | Commonly Observed Pattern | Clinical Impact |
|---|---|---|
| Motor Type | Spasticity | Increased muscle stiffness. gait abnormalities |
| Functional Level | GMFCS III-V | Requirement for assistive mobility devices |
| Neurological | Epilepsy | Requirement for long-term anticonvulsant therapy |
| Sensory | Visual/Hearing Loss | Challenges in communication and environmental navigation |
The Role of Tertiary Care in the UAE Healthcare Ecosystem
The reliance on tertiary referral hospitals in Dubai suggests a centralized model of care where specialized expertise is concentrated. For families, In other words that while they have access to world-class diagnostics and surgical options, the logistical burden of frequent travel to a central hub can be significant.

The study’s timeframe (2018-2020) captures a critical era of healthcare expansion in the UAE. The integration of World Health Organization guidelines on cerebral palsy into local practice has emphasized the move toward “family-centered care,” where the goals of therapy are aligned with the daily needs of the family rather than just clinical markers.
One of the most critical takeaways from the Dubai study is the importance of early detection. When clinical patterns are identified early, the window for neuroplasticity—the brain’s ability to reorganize itself—is widest. This makes the transition from primary care screening to tertiary specialist intervention a pivotal moment in a child’s development.
Implications for Future Public Health Policy
The data gathered from these referral hospitals serves as a foundation for future public health initiatives in the Emirates. By identifying the most common clinical patterns, health authorities can develop more precise screening protocols for newborns and infants, potentially catching signs of motor delay before they become permanent disabilities.
the high prevalence of comorbidities suggests a need for “one-stop” clinics. Instead of a family visiting a neurologist, a cardiologist, and a physical therapist in three different locations, the trend is moving toward integrated pediatric centers where all specialists collaborate under one roof.
For those seeking more information on managing pediatric neurological conditions, the Cerebral Palsy Network provides evidence-based resources for clinicians and caregivers globally.
Disclaimer: This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
The next step for the region involves the transition from retrospective observation to prospective longitudinal studies. Researchers are expected to track these cohorts to determine how different intervention strategies—such as robotic-assisted gait training or selective dorsal rhizotomy—impact long-term outcomes for children in the UAE.
We invite readers to share their experiences with pediatric care in the comments below or share this article with healthcare professionals in your network.