For many, the arrival of spring is heralded by blooming cherry blossoms and warmer breezes. But for millions of others, the season brings a more irritating companion: the relentless, burning itch of allergic conjunctivitis. This condition, often dismissed as a minor seasonal nuisance, is actually a complex immune response that can significantly impair quality of life if left unmanaged.
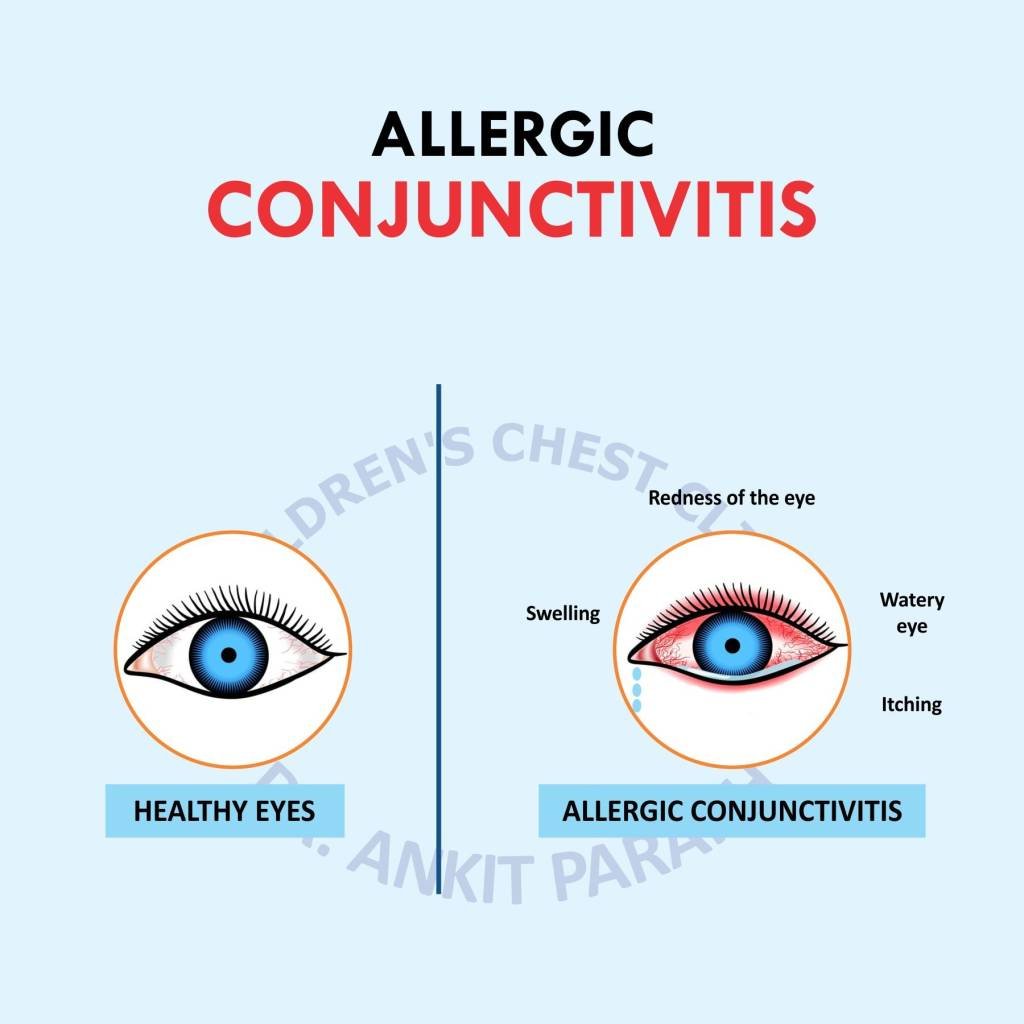
Allergic conjunctivitis occurs when the immune cells in the conjunctiva—the thin, transparent membrane lining the eyelid and covering the white part of the eye—overreact to external antigens. These antigens, commonly pollen from trees and grasses, trigger the release of histamine and other inflammatory mediators. This chemical cascade causes blood vessels to dilate and fluid to leak into the tissues, resulting in the characteristic redness, swelling and intense itching associated with seasonal allergies.
The most instinctive reaction to this irritation is to rub the eyes. However, medical professionals warn that Here’s the worst possible response. Rubbing the eyes not only introduces more allergens into the ocular environment but as well triggers the mechanical rupture of mast cells, which releases even more histamine. This creates a feedback loop that intensifies the inflammation and can, in severe cases, lead to corneal thinning or a condition known as keratoconus, where the cornea bulges into a cone shape, permanently altering vision.
Distinguishing Allergies from Infections
A critical challenge for patients is distinguishing between allergic conjunctivitis and infectious forms of the disease, such as viral or bacterial conjunctivitis (commonly known as “pink eye”). While all three cause redness and irritation, the nature of the ocular discharge is a primary diagnostic clue.
In cases of bacterial conjunctivitis, the eye typically produces a thick, yellow, or greenish discharge that can cause the eyelids to stick together upon waking. In contrast, allergic conjunctivitis is characterized by a watery, transparent, and often “stringy” or sticky secretion. The presence of intense itching is almost always a hallmark of an allergic reaction, whereas viral infections are more likely to produce a gritty sensation or a feeling of foreign bodies in the eye.
| Feature | Allergic | Viral | Bacterial |
|---|---|---|---|
| Primary Symptom | Intense Itching | Watery/Gritty | Burning/Irritation |
| Discharge | Clear, Stringy | Watery/Clear | Thick, Yellow/Green |
| Onset | Rapid/Seasonal | Gradual/Contagious | Gradual/Contagious |
| Eye Involvement | Usually Both Eyes | Often starts in one | Often starts in one |
The Danger of the “Itch-Scratch Cycle”
The danger of rubbing eyes extends beyond the immediate release of histamine. The delicate surface of the eye is susceptible to micro-abrasions. When a person rubs their eyes during an allergic flare, they are effectively scrubbing the corneal epithelium with particles of pollen or dust, which can lead to secondary infections or corneal ulcers.
the chronic inflammation associated with untreated allergic conjunctivitis can lead to a thickening of the conjunctiva. According to the American Academy of Ophthalmology, managing the inflammatory response early is key to preventing long-term ocular surface damage. By breaking the itch-scratch cycle, patients can avoid the escalation of symptoms from mild irritation to severe chemosis, where the conjunctiva becomes so swollen it looks like a blister on the eye.
Practical Strategies for Symptom Relief
For those suffering from spring allergies, the goal is to reduce the allergen load and stabilize the mast cells. While over-the-counter solutions are available, a systematic approach to ocular hygiene is most effective.
- Cold Compresses: Applying a clean, cold cloth or a chilled gel mask to closed eyelids helps constrict blood vessels and soothe the itch without the require for rubbing.
- Artificial Tears: Preservative-free artificial tears can help flush out pollen and pollutants from the surface of the eye, providing a mechanical rinse that reduces the concentration of antigens.
- Environmental Control: Keeping windows closed during peak pollen hours (usually early morning) and wearing wraparound sunglasses outdoors can physically block allergens from reaching the eyes.
- Pharmacological Intervention: Antihistamine eye drops or mast cell stabilizers can prevent the release of histamine. These should be used under the guidance of a healthcare provider to ensure the correct formulation for the patient’s specific allergy profile.
For more comprehensive guidance on managing seasonal allergies, the Mayo Clinic provides detailed protocols on identifying triggers and utilizing prophylactic treatments before the spring season peaks.
Long-term Management and Prevention
While acute treatment focuses on symptom relief, long-term management involves identifying the specific triggers through allergy testing. Once a patient knows whether they are reacting to birch, cedar, or grass pollen, they can better time their medication and avoid high-risk environments. In some cases, immunotherapy (allergy shots) may be recommended to desensitize the immune system over time, reducing the overall severity of the spring response.
Maintaining a strict hygiene routine—such as washing hands and face immediately after coming indoors and showering before bed to remove pollen from the hair—can significantly reduce the nocturnal exposure that often leads to waking up with swollen, itchy eyes.
Disclaimer: This article is for informational purposes only and does not constitute professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
As we move deeper into the spring season, pollen counts are expected to fluctuate based on regional weather patterns and temperature spikes. Patients are encouraged to monitor local pollen forecasts and consult an ophthalmologist or allergist to establish a preventative care plan before the peak pollination period arrives in late spring.
Do you have a specific routine that helps you manage seasonal eye allergies? Share your experiences in the comments below or share this guide with someone struggling with the spring itch.

