The sudden onset of a runny nose, a persistent cough, and a general feeling of malaise can be disorienting, especially when these symptoms overlap across several different conditions. For many, the primary challenge is determining whether they are dealing with a seasonal flare-up or a contagious illness. Understanding the difference between allergies and a cold is essential not only for personal recovery but for preventing the spread of viral infections in the community.
While the outward signs may appear identical, the underlying biological mechanisms are entirely different. A cold is caused by a virus—most commonly rhinoviruses—that attacks the upper respiratory tract. Allergies, conversely, are an overreaction of the immune system to harmless environmental triggers, such as pollen, dust mites, or pet dander. As a physician, I often remind patients that while both cause inflammation in the nasal passages, one is an invasion and the other is a hypersensitivity.
Distinguishing between the two requires looking beyond the primary symptoms to the “supporting evidence” of the body’s response. The timing, the presence of a fever, and the nature of the nasal discharge provide critical clues. When these indicators are analyzed together, the path to the correct treatment becomes clear, preventing the misuse of medications that may be ineffective or even counterproductive depending on the diagnosis.
Decoding the Symptoms: Viral vs. Allergic
The most reliable way to tell the two apart is to look for symptoms that do not cross over. For instance, a fever is a hallmark of a viral infection as the body ramps up its internal temperature to kill the pathogen. Allergies never cause a fever. Similarly, while a cold may cause a mild ache in the muscles, a high-grade fever or significant body aches almost always point toward a virus or a more severe respiratory infection.
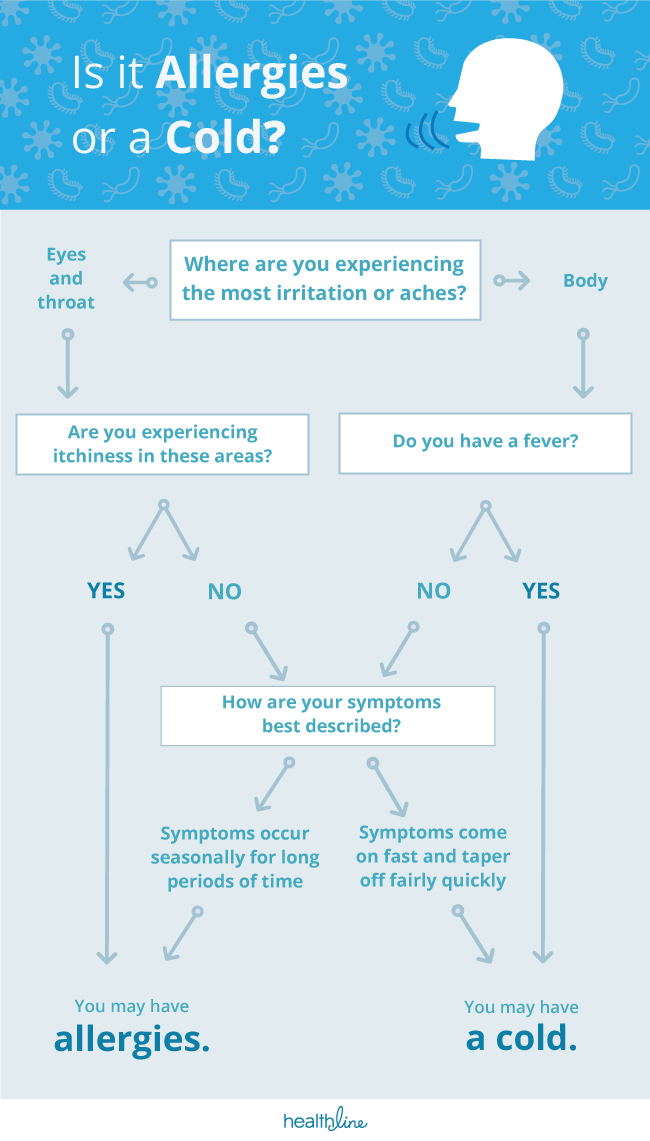
The nature of the itch is another defining characteristic. Allergic reactions typically trigger the release of histamine, which causes intense itching in the eyes, nose, and throat. While a cold can make the throat sense “scratchy” or sore due to inflammation and post-nasal drip, it rarely produces the classic, irritating itch associated with allergic rhinitis.
The duration of the illness too serves as a diagnostic tool. A common cold typically runs its course in seven to ten days. Allergies, but, persist as long as the trigger is present. If your symptoms last for weeks or only appear when you are outdoors during peak pollen season, the likelihood of an allergic response is significantly higher.
| Symptom | Common Cold (Viral) | Seasonal Allergies |
|---|---|---|
| Fever | Common (especially in children) | Never |
| Itchy Eyes/Nose | Rare | Very Common |
| Mucus Color | Often yellow or green | Usually clear and watery |
| Onset | Gradual over a few days | Rapid/Immediate upon exposure |
| Duration | 7 to 10 days | Weeks or months |
The Role of Mucus and Inflammation
Many people believe that the color of their mucus is a definitive diagnostic tool. While it is true that thick, yellow, or green mucus is more common with viral infections—as the immune system sends white blood cells to fight the virus—it is not a foolproof rule. Some allergy sufferers can develop secondary sinus infections that change the color of their discharge.
However, the consistency is usually a giveaway. Allergic discharge is typically thin, clear, and watery. This is a direct result of the body attempting to flush the allergen out of the nasal cavity. In contrast, viral mucus tends to be thicker and more viscous, which can lead to a feeling of congestion and pressure in the sinuses.
The “cough” also differs in quality. A cold cough is often productive, meaning it brings up phlegm from the chest or throat. An allergy-induced cough is typically a dry, hacking reflex caused by post-nasal drip irritating the larynx. This “trickle” of mucus down the back of the throat is a common cause of nocturnal coughing for those with environmental sensitivities.
When to Seek Medical Intervention
Knowing the difference is not just about choosing between an antihistamine and a decongestant; it is about recognizing when a condition has evolved into something more serious. For those with allergies, untreated inflammation can lead to secondary issues. For example, chronic nasal congestion can trigger the development of sinusitis or exacerbate underlying asthma.
According to the Centers for Disease Control and Prevention (CDC), monitoring for “red flag” symptoms is crucial. If a simple cold progresses to a high fever that will not break, shortness of breath, or chest pain, it may have evolved into pneumonia or another lower respiratory tract infection requiring prescription antibiotics or antivirals.
For those struggling to identify their triggers, a board-certified allergist can perform skin-prick tests or blood tests (IgE tests) to identify the exact proteins causing the reaction. This allows for a targeted approach, such as immunotherapy, rather than a lifelong reliance on over-the-counter symptom suppressants.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
As we move into the next peak pollen season, public health officials continue to monitor air quality and pollen counts to provide early warnings for sensitive populations. Checking local aeroallergen reports remains the most effective way to anticipate and mitigate the impact of seasonal triggers before they begin.
Do you have a specific method for telling your allergies apart from a cold? Share your experiences in the comments below or share this guide with someone who might be struggling with their symptoms.

