For millions of people living with treatment-resistant depression, the traditional path of antidepressants and psychotherapy does not always provide the necessary relief. In these cases, medical science has turned toward the brain’s electrical architecture. Repetitive Transcranial Magnetic Stimulation (rTMS), a non-invasive procedure that uses magnetic fields to stimulate nerve cells, has emerged as a clinically proven intervention for those who have not responded to medication.
While rTMS is widely recognized as an effective treatment for depression, the primary barrier for many patients has been the grueling nature of the protocol. Standard clinical guidelines typically require a rigorous schedule of daily sessions over several weeks—often spanning nearly two months—to achieve a stable therapeutic response. This time-intensive commitment can be a significant hurdle for patients already struggling with the debilitating fatigue and cognitive fog associated with severe depressive episodes.
As a physician, I have seen how the “treatment burden” can lead to attrition. When a patient is told they must visit a clinic every single day for six to eight weeks, the logistical and emotional toll can be as daunting as the illness itself. The current scientific push is therefore focused on “accelerated” protocols, aiming to condense the delivery of these magnetic pulses to achieve the same clinical efficacy in a fraction of the time.
The Mechanics of Magnetic Stimulation
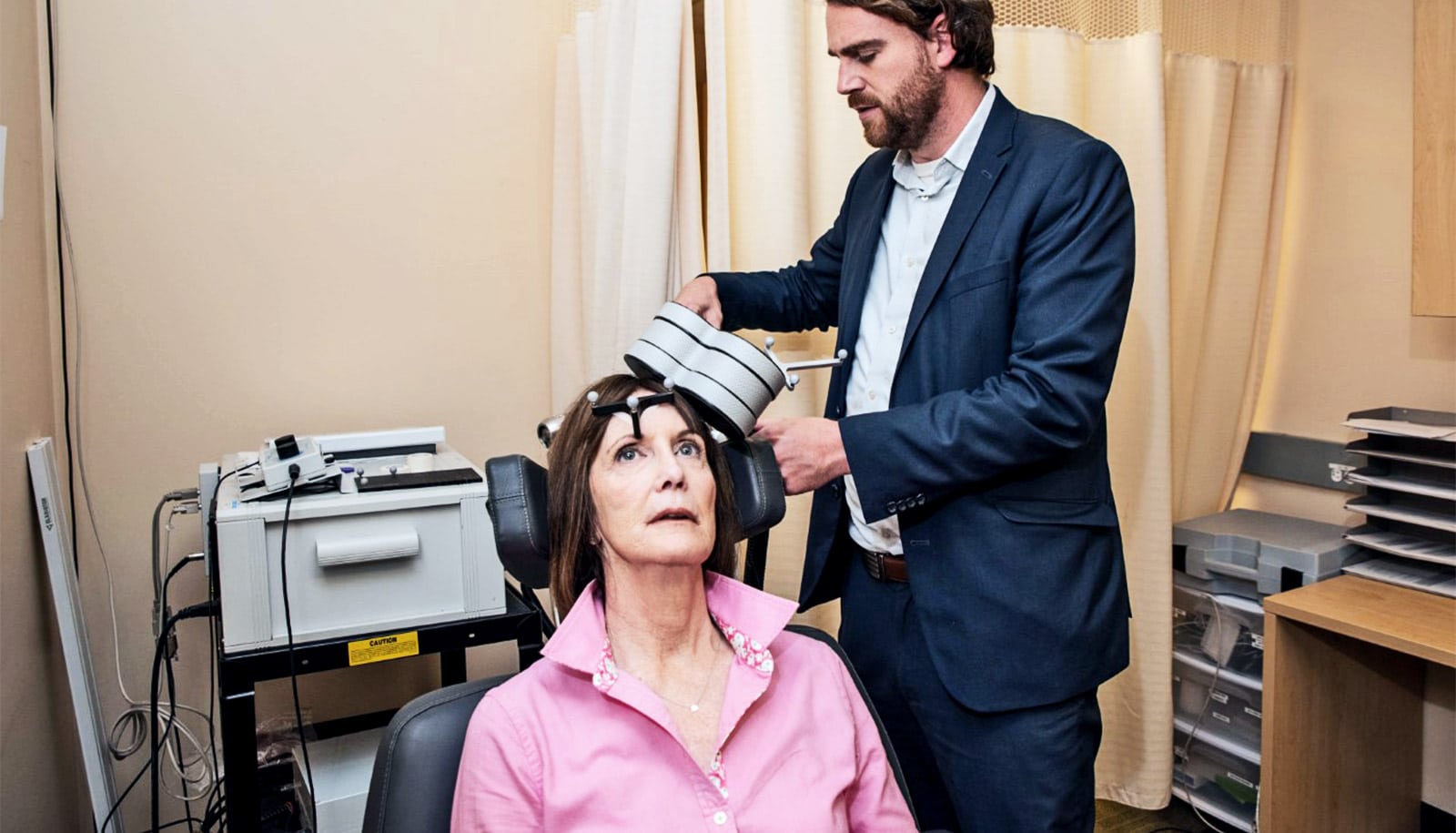
Unlike Electroconvulsive Therapy (ECT), which involves the induction of a seizure under general anesthesia, rTMS does not require sedation and does not cause loss of consciousness. The process involves placing an electromagnetic coil against the scalp. This coil generates brief, powerful magnetic pulses that pass through the skull to stimulate specific regions of the brain, most commonly the left dorsolateral prefrontal cortex (DLPFC), an area heavily involved in mood regulation.
The goal is to “reawaken” underactive neural circuits. By inducing electrical currents in these targeted neurons, rTMS helps restore the brain’s plasticity and improves the communication between different brain regions. According to the Mayo Clinic, the procedure is typically reserved for adults who have not seen improvement from at least one antidepressant medication.
Standard vs. Accelerated Protocols
The traditional approach to rTMS is a “marathon” of stimulation. A typical course involves 20 to 30 sessions, usually delivered once per day, five days a week. This timeline is designed to allow the brain to integrate the stimulation over time, but it creates a significant gap between the start of treatment and the point of clinical remission.
Emerging research into “theta-burst stimulation” (TBS) and accelerated regimens is attempting to change this. By delivering multiple sessions per day—sometimes up to ten—researchers are investigating whether the brain can reach the same threshold of recovery in just a few days rather than two months. This shift would transform rTMS from a long-term commitment into an intensive, short-term “burst” of therapy.
| Feature | Standard rTMS | Accelerated rTMS (Experimental) |
|---|---|---|
| Duration | 4 to 8 weeks | Few days to 2 weeks |
| Frequency | 1 session per day | Multiple sessions per day |
| Patient Burden | High (Daily travel) | Moderate (Intensive short-term) |
| Clinical Goal | Sustained remission | Rapid symptom reduction |
Who Benefits Most from Magnetic Stimulation?
rTMS is not a universal cure, but it serves as a critical lifeline for a specific subset of the population. Patients with “treatment-resistant depression”—defined as those who have failed to respond to two or more different classes of antidepressants—are the primary candidates. For these individuals, the chemical imbalance is often compounded by a lack of connectivity in the prefrontal cortex, which magnetic pulses can directly address.
The efficacy of the treatment is often measured by the “response rate” (a 50% reduction in symptoms) and the “remission rate” (the virtual absence of symptoms). Data from the National Institute of Mental Health suggests that a significant percentage of patients who fail medication still find relief through neuromodulation.
Potential Side Effects and Safety
Because the procedure is non-invasive, the side-effect profile is generally mild. The most common reports include:

- Scalp Discomfort: A tapping or tingling sensation during the pulse delivery.
- Headaches: Mild tension-type headaches following a session.
- Seizure Risk: While extremely rare, there is a marginal risk of induced seizures, which is why rigorous screening for epilepsy is mandatory.
The Future of Neuromodulation
The transition toward more efficient, shorter treatment windows is part of a larger trend in psychiatry: precision medicine. By using functional MRI (fMRI) scans, clinicians can now more accurately target the exact coordinates of a patient’s brain that require stimulation, potentially reducing the number of sessions needed and increasing the success rate.
the integration of “closed-loop” systems—devices that can sense brain activity and deliver stimulation only when needed—could eventually move these treatments from the clinic into more accessible settings. The objective is to move away from the “one size fits all” two-month protocol toward a tailored experience based on the patient’s unique neural signature.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
As clinical trials for accelerated rTMS protocols continue to publish their results, the next major checkpoint will be the updated guidelines from global psychiatric associations regarding the “dose-response” relationship of magnetic stimulation. These updates will determine if the shorter, more intense schedules can officially replace the traditional two-month model in standard clinical practice.
Do you have experience with rTMS or other neuromodulation therapies? We invite you to share your perspective or ask questions in the comments below.