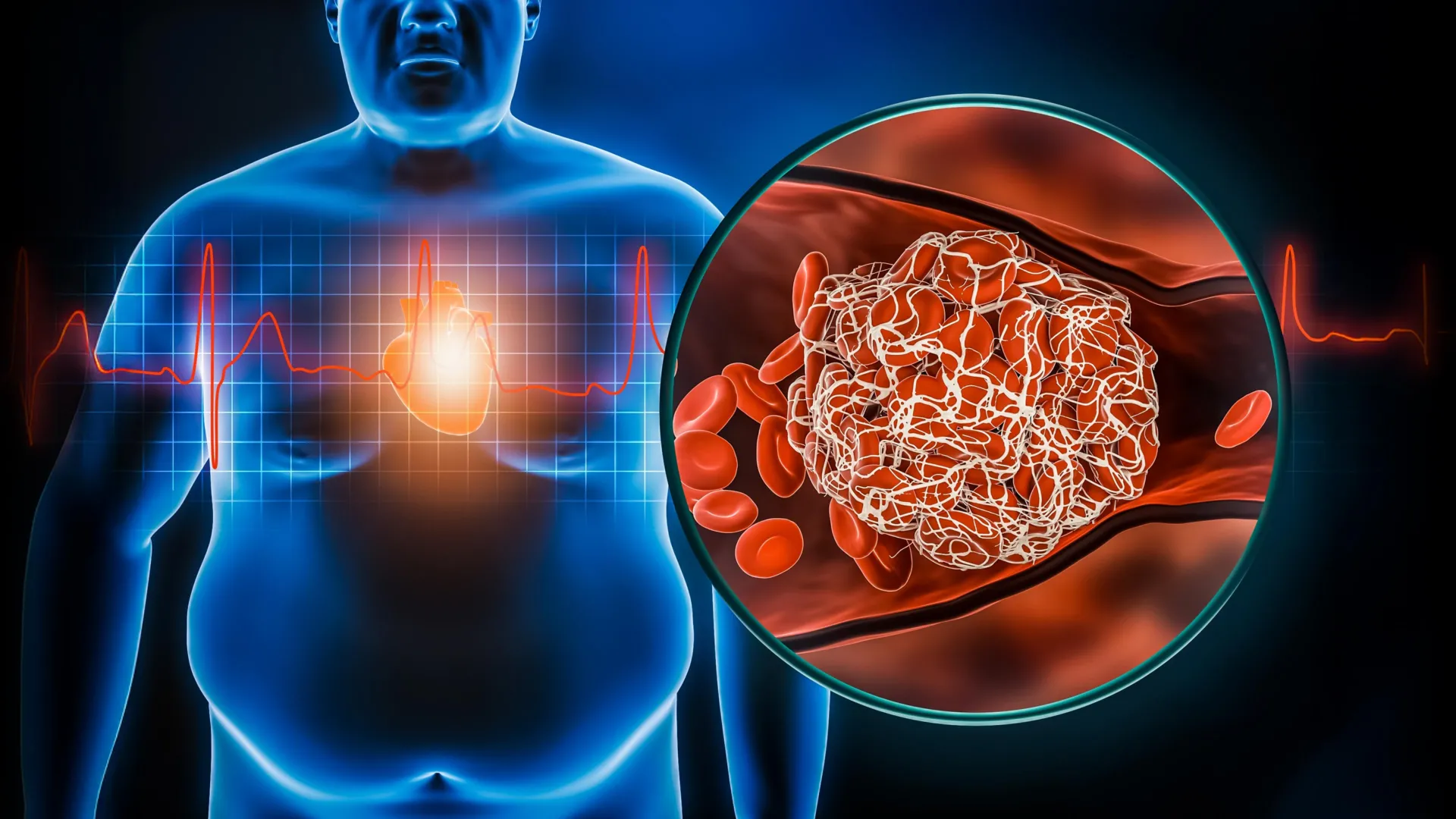
For decades, medical guidelines have treated obesity as a uniform challenge—a matter of calories, BMI, and general cardiovascular risk. However, new evidence suggests that the underlying pathology of the disease diverges sharply based on biological sex, meaning that the health risks of obesity in men vs women are often hidden in plain sight, manifesting through different biomarkers and organ stresses.
Findings presented at the European Congress on Obesity (ECO) in Istanbul, Turkey, reveal that while both sexes face increased dangers from excess weight, the “how” and “where” of those risks differ. Research led by Dr. Zeynep Pekel of Dokuz Eylul University suggests that men are more prone to metabolic and liver-related complications, while women exhibit a more pronounced inflammatory response and higher cholesterol levels.
As a physician, I have seen how a “one-size-fits-all” approach to weight management can overlook these nuances. When a clinician looks only at a scale, they may miss the specific physiological pressures mounting inside a patient’s body. These insights move the conversation away from simple weight loss and toward targeted, sex-based therapies that address the specific biological vulnerabilities of the individual.
The Male Profile: Visceral Fat and Liver Stress
The study, which analyzed data from 248 men and 886 women treated at the Dokuz Eylul University Obesity Clinic, found a distinct pattern in how men store adipose tissue. Men were significantly more likely to accumulate visceral fat—the dangerous fat that wraps around internal organs rather than sitting just beneath the skin.
This abdominal distribution is not merely an aesthetic concern. It’s a metabolic engine that drives systemic disease. The researchers observed that men in the study had a much larger average waist circumference (120 cm compared to 108 cm for women) and higher systolic blood pressure (128 mmHg vs 122 mmHg), both of which are primary indicators of cardiovascular strain.
Beyond the waistline, the biological markers in men pointed toward higher stress on the liver and kidneys. The team recorded significantly higher levels of creatinine and liver enzymes, specifically alanine aminotransferase (ALT) and gamma-glutamyl transferase (GGT). These elevations often serve as early warning signs of liver damage or the progression of non-alcoholic fatty liver disease, a common complication of obesity that can lead to cirrhosis if left unchecked.
The Female Profile: Inflammation and Lipid Imbalance
While men faced higher risks of organ-specific metabolic stress, women with obesity presented a different set of “hidden” risks. The data showed that women typically had higher total cholesterol (215 mg/dL vs 203 mg/dL in men) and higher levels of low-density lipoprotein (LDL), often referred to as “bad” cholesterol.
More striking, however, was the inflammatory profile. Women showed elevated levels of C-reactive protein, erythrocyte sedimentation rate, and platelet counts. These are markers of systemic inflammation, a state where the immune system remains chronically activated. This persistent inflammation is a known catalyst for the development of type 2 diabetes and atherosclerosis, the hardening of the arteries that leads to heart attacks and strokes.
The difference in risk is partly explained by where the fat is stored. Women tend to store more subcutaneous fat—fat located beneath the skin—which, while contributing to overall weight, does not always trigger the same immediate metabolic crisis as visceral fat. However, the corresponding increase in inflammatory markers suggests that the female body may respond to obesity with a more aggressive immune reaction.
| Marker | Men (Average) | Women (Average) | Primary Risk Association |
|---|---|---|---|
| Waist Circumference | 120 cm | 108 cm | Cardiovascular/Diabetes |
| Systolic Blood Pressure | 128 mmHg | 122 mmHg | Hypertension/Heart Strain |
| Total Cholesterol | 203 mg/dL | 215 mg/dL | Atherosclerosis |
| LDL (“Bad”) Cholesterol | 123 mg/dL | 130 mg/dL | Arterial Plaque |
| BMI | 37.5 kg/m² | 36 kg/m² | General Obesity Risk |
The Biological Drivers: Hormones and Genetics
These divergent paths are not accidental; they are rooted in deep biological differences. Dr. Pekel attributes these findings to the interplay of hormones, immune system activity, and genetic factors. Estrogen, for instance, plays a critical role in determining where fat is deposited and how the body regulates its inflammatory response.
the researchers noted that women generally possess a more active immune response, a trait partially linked to the X chromosome. This heightened reactivity may explain why women in the study exhibited higher levels of inflammation-related markers despite having lower waist circumferences than their male counterparts.
“Our findings reveal intriguing differences in the way men and women respond to obesity,” said Dr. Pekel. “They reveal just how essential gender-specific research is. Not only are sex differences a powerful player in the pathology and course of obesity, but our results indicate that such differences could be a stepping stone toward finding targeted, sex-based therapies to help in the management of people living with obesity.”
A Global Crisis of Metabolic Syndrome
The urgency of this research is underscored by the scale of the global epidemic. According to a systematic review published in Nature Communications, approximately 1.54 billion adults worldwide were living with metabolic syndrome in 2023. This condition—a cluster of risks including abdominal obesity, high blood pressure, and elevated glucose—affects roughly 1 in 3 women and 1 in 4 men.

When a patient is diagnosed with metabolic syndrome, the goal is typically to reduce the overall risk of cardiovascular disease. However, if the drivers of that risk are different for men and women, the treatment should be as well. For a man, the priority might be aggressive management of liver enzymes and visceral fat reduction; for a woman, the focus might shift toward mitigating systemic inflammation and managing LDL cholesterol.
Constraints and Future Directions
While these findings provide a compelling roadmap, the researchers cautioned that the study has limitations. Because the research was cross-sectional, it provides a snapshot in time rather than a long-term cause-and-effect analysis. The participants were primarily of Turkish ethnicity, meaning the results may not be perfectly generalizable to all global populations.
The next phase of this research will involve validating these patterns in larger, more diverse patient groups. The goal is to move beyond observation and determine exactly how these sex-based biomarkers correlate with long-term clinical outcomes, such as the rate of heart failure or the onset of kidney disease.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
The medical community is now looking toward larger-scale validation studies to refine these findings, with the ultimate aim of integrating sex-specific markers into standard obesity clinical guidelines. We will continue to monitor updates from the European Congress on Obesity as more peer-reviewed data becomes available.
Do you think healthcare providers should use different screening tools for men and women with obesity? Share your thoughts in the comments or share this article with your network.