For decades, a silent epidemic has persisted in the world’s most food-insecure regions, often hidden behind the labels of more common metabolic disorders. In 2025, the International Diabetes Federation (IDF) officially recognized type 5 diabetes, a distinct form of the disease rooted in severe nutrient deficiency rather than autoimmune failure or lifestyle-induced insulin resistance.
This formal designation marks the end of a seventy-year scientific debate and provides a critical clinical framework for a condition that is estimated to affect up to 25 million people worldwide. The IDF is now urging other global health authorities, including the World Health Organization (WHO), to adopt this classification to ensure patients receive the specific care their unique metabolic profiles require.
As a physician, I have seen how the “one size fits all” approach to chronic disease can fail vulnerable populations. The danger here is not just a lack of treatment, but the application of the wrong treatment. Because type 5 diabetes does not follow the typical pathways of type 1 or type 2, standard therapies can be ineffective or, in some cases, life-threatening.
The recognition of this disease is more than a semantic victory; it is a prerequisite for funding, standardized diagnostic criteria, and the development of therapies tailored to those living in extreme poverty.
A Seventy-Year Struggle for Recognition
The history of type 5 diabetes is a study in medical erasure. First described in Jamaica in 1955, the condition—previously known as malnutrition-related diabetes mellitus (MRDM)—was largely ignored by the global medical community for decades. Although the WHO acknowledged the diagnosis in the 1980s, the classification remained contentious, leading the organization to withdraw it in 1999 due to a perceived lack of evidence.

The controversy stemmed from a lack of consensus on how to differentiate MRDM from other forms of diabetes. However, recent research has finally provided the metabolic evidence needed to separate it from its counterparts. A pivotal 2022 study led by Meredith Hawkins, an endocrinologist at the Albert Einstein College of Medicine’s Global Diabetes Institute, established a unique metabolic profile for the disease.
Through a trial in south India, Hawkins and her team demonstrated that patients with this form of diabetes are insulin-deficient, similar to those with type 1 diabetes, but not to the same extreme. Crucially, unlike those with type 2 diabetes, these patients remain sensitive to insulin, meaning their bodies can still use the hormone effectively—they simply do not produce enough of it.
Understanding the Pathogenesis: Why Type 5 is Different
To understand why a separate classification is necessary, one must look at the different ways the body fails to regulate blood glucose. Most people are familiar with the “big two,” but the medical landscape is more complex.
| Type | Primary Cause | Insulin Status |
|---|---|---|
| Type 1 | Autoimmune destruction of pancreas | Severe deficiency |
| Type 2 | Insulin resistance (lifestyle/genetics) | Variable / Resistance |
| Type 3c | Physical damage to the pancreas | Deficiency due to trauma |
| Gestational | Pregnancy-induced hormonal shifts | Temporary resistance |
| Type 5 | Chronic nutrient deficiency | Developmental deficiency |
Type 5 diabetes is theorized to result from compromised pancreatic development. According to Rahul Garg, a physician at F.H. Medical College and Hospital in India, this happens during extended periods of nutritional insufficiency, which disrupts the pancreas’s lifelong ability to secrete insulin and balance blood sugar levels.
This distinction is vital because it changes the risk profile for the patient. In type 2 diabetes, the primary goal is often to overcome insulin resistance. In type 5, the patient is already sensitive to insulin; administering standard high-dose insulin treatments can cause blood sugar to plummet dangerously.
The Human Cost of Misdiagnosis
The impact of type 5 diabetes is most acutely felt in Asia and Africa, though it is a growing concern in Latin America and the Caribbean due to escalating political and economic instability. Because the disease is so often misdiagnosed as type 1 or type 2, patients are frequently put on inappropriate medication regimens.
Meredith Hawkins has warned that the lack of an official name hindered efforts to find effective therapies for a disease that she describes as more common than tuberculosis and nearly as common as HIV/AIDS. The danger of inappropriate insulin treatment is particularly high in settings where food insecurity is rampant and affordable glucose monitoring is unavailable.
“Inappropriate insulin treatment could induce hypoglycemia [low blood sugar levels], which can be a particular risk in settings with food insecurity and where glucose monitoring might not be affordable,” Hawkins and her colleagues explained in a recent review.
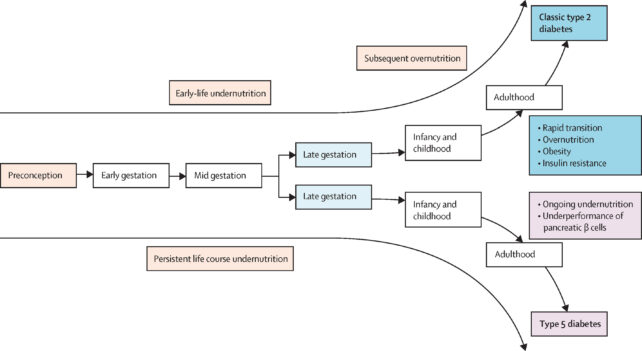
For these patients, the clinical “fine line” is narrow. They may require only minimal supplementary insulin or alternative methods to stimulate their own insulin secretion to avoid the lethal spikes and crashes associated with improper dosing.
Next Steps for Global Health
The IDF’s recognition of type 5 diabetes is the first step in a broader effort to standardize care. In 2025, the IDF established a dedicated type 5 diabetes working group, chaired by Dr. Hawkins. This group is tasked with three primary objectives: developing formal diagnostic criteria and therapeutic guidelines, establishing a global research registry to track the disease’s prevalence, and creating specialized training for healthcare professionals in low-resource settings.
While some researchers argue that “diagnostic uncertainty” still exists due to the variety of malnutrition-related cases, the consensus among advocates is that the risk of inaction is far greater than the risk of imperfect classification. Without a formal name, the disease remains invisible to policymakers and funding bodies.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Please consult a healthcare professional for diagnosis and treatment of any medical condition.
The next major milestone for the community will be the publication of the IDF’s formal therapeutic guidelines, which will provide clinicians with the first standardized roadmap for treating type 5 diabetes safely. We invite you to share this story and join the conversation on how we can better address neglected diseases in underserved regions.