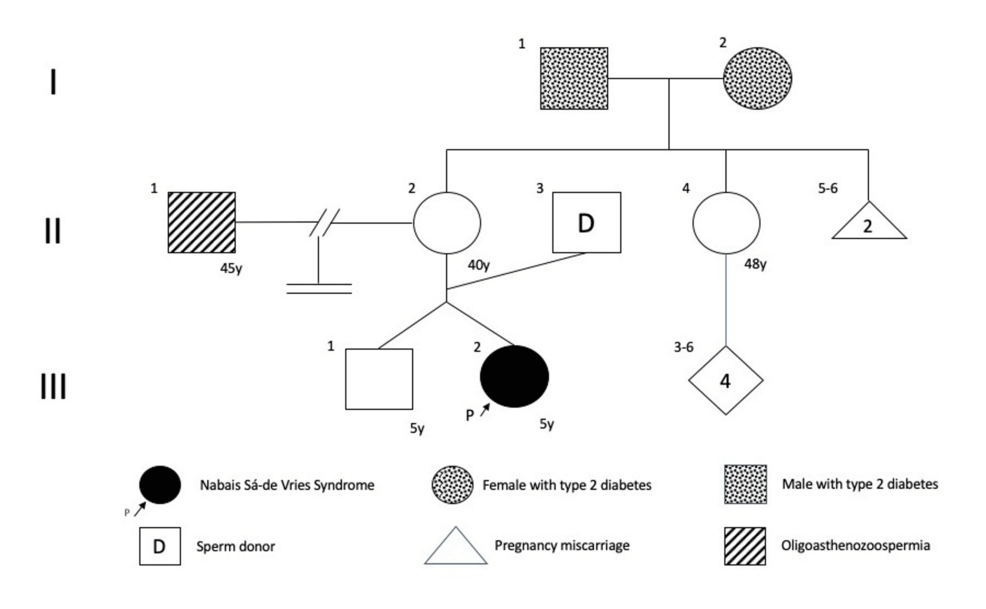
For a young girl in Mexico, the path to a medical diagnosis was as complex as the symptoms she presented. Facing a combination of developmental delays, intellectual disabilities, and cardiac irregularities, her case highlights the diagnostic challenges associated with ultra-rare genetic conditions that often slip through the cracks of standard pediatric screenings.
Medical professionals have identified her condition as Nabais Sá-de Vries Syndrome Type 1, an exceptionally rare multisystem disorder. Because the syndrome manifests across different organ systems—affecting the brain, the heart, and physical development—it requires a multidisciplinary approach to identify and manage. The confirmation of this diagnosis in the patient was made possible through targeted genetic testing, which revealed a pathogenic variant in the SNC5A gene.
As a physician and medical writer, I have seen how “diagnostic odysseys” can strain families. In cases like this, the transition from a set of unexplained symptoms to a named syndrome is more than a clinical victory; We see a roadmap for life-saving preventative care, particularly regarding the heart.
The Clinical Triad of Nabais Sá-de Vries Syndrome
Nabais Sá-de Vries Syndrome (NSdV) is characterized by a distinct “triad” of clinical findings. When these three elements appear together, they provide a strong signal to clinicians that they are dealing with this specific genetic mutation rather than a more common developmental disorder.
The first element is developmental and cognitive impairment. The patient in this case exhibited significant intellectual disability and delays in reaching early childhood milestones. These cognitive challenges are a hallmark of the syndrome and typically require long-term educational and therapeutic support.
The second element involves dysmorphism, or distinctive facial features. While these features can vary, they often include a broad nasal bridge and other subtle craniofacial characteristics that, while not immediately obvious to a layperson, are recognized by clinical geneticists as markers of the syndrome.
The third and most critical element is the presence of cardiac conduction system abnormalities. The heart’s electrical system, which regulates the beat, is often compromised in individuals with NSdV Type 1. This can manifest as various forms of heart block or conditions similar to Brugada syndrome, which can predispose an individual to dangerous arrhythmias.
The Genetic Blueprint: The Role of SNC5A
The underlying cause of Nabais Sá-de Vries Syndrome Type 1 is a mutation in the SNC5A gene. This gene provides instructions for making the alpha subunit of the cardiac sodium channel, a protein essential for the initiation and propagation of electrical impulses in the heart muscle.
When the SNC5A gene is mutated, the sodium channels may not function correctly, leading to “electrical instability” in the heart. While mutations in this gene are also linked to other conditions—such as Brugada syndrome or Long QT syndrome—the specific mutation associated with NSdV Type 1 results in a broader systemic effect, impacting not only the heart but also neurological development.
The distinction between Type 1 and other variants of the syndrome is primarily genetic. By utilizing whole-exome sequencing or targeted gene panels, physicians can pinpoint the exact location of the mutation, allowing them to differentiate NSdV from other overlapping syndromes that present with similar intellectual disabilities and cardiac issues.
| System Affected | Common Manifestations | Clinical Significance |
|---|---|---|
| Cardiac | Conduction blocks, arrhythmias | Risk of sudden cardiac arrest |
| Neurological | Intellectual disability, developmental delay | Requires specialized education/therapy |
| Physical | Distinctive facial features (dysmorphism) | Aids in early clinical suspicion |
| Genetic | SNC5A gene mutation | Confirms Type 1 diagnosis |
Why Early Detection is Life-Saving
The identification of Nabais Sá-de Vries Syndrome Type 1 is not merely an academic exercise in labeling; it is a critical step in preventing sudden cardiac death. Because the SNC5A mutation can lead to unpredictable heart rhythms, patients require rigorous cardiac monitoring.
For the girl in this report, the diagnosis allows her medical team to implement a proactive surveillance plan. This typically includes regular electrocardiograms (ECGs) and potentially the implantation of a pacemaker or an implantable cardioverter-defibrillator (ICD) if high-grade heart block or dangerous arrhythmias are detected. Without this genetic confirmation, a clinician might treat the developmental delays while remaining unaware of the hidden, life-threatening cardiac risk.
a genetic diagnosis provides essential information for the family. Understanding that the condition is genetic allows parents to seek screening for other family members who may carry the same mutation, even if they are currently asymptomatic. This “cascade screening” can identify at-risk relatives before a cardiac event occurs.
Navigating the Rare Disease Landscape
Rare diseases like NSdV Type 1 often go underdiagnosed because they do not fit into a single medical specialty. A cardiologist may spot the heart issue, and a neurologist may see the intellectual disability, but without a unifying diagnosis, the patient receives fragmented care. This case underscores the importance of the “medical geneticist” as the coordinator who connects these disparate symptoms into a single, actionable diagnosis.
For those seeking more information on rare genetic conditions, the National Organization for Rare Disorders (NORD) provides resources for patients and clinicians to identify emerging syndromes and connect with specialized care centers.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
The next step for patients with confirmed NSdV Type 1 is the establishment of a lifetime cardiac surveillance protocol to monitor for the progression of conduction defects. As genetic sequencing becomes more accessible in regions like Mexico, the hope is that more children with this syndrome will be identified early, moving them from a state of uncertainty to a managed, safer clinical path.
Do you have experience with rare disease diagnostics or genetic screening? Share your thoughts or questions in the comments below.