For millions of people who have survived a deep vein thrombosis (DVT), the initial clot is not the end of the story. Many develop a chronic, debilitating condition known as post-thrombotic syndrome (PTS), characterized by persistent leg swelling, pain and skin changes that can severely limit mobility and quality of life.
A latest randomized clinical trial published in the New England Journal of Medicine suggests that for a specific subset of these patients, endovascular therapy for post-thrombotic syndrome—specifically the surgical opening of obstructed veins—can provide significant relief compared to standard medical management alone.
The study focused on patients with symptomatic chronic venous obstruction, a state where the veins remain blocked or narrowed long after the initial clot has been treated. By using minimally invasive techniques to clear these blockages, researchers found a measurable improvement in both the physical symptoms of the legs and the overall functional capacity of the participants.
This finding is particularly significant because the gold standard for PTS has long been conservative therapy, which primarily involves compression stockings and exercise. While effective for some, these measures often fail to address the underlying mechanical obstruction that drives the disease.
Understanding the Burden of Chronic Venous Obstruction
Post-thrombotic syndrome occurs when a previous blood clot damages the valves in the veins or leaves a permanent obstruction. This prevents blood from flowing efficiently back toward the heart, causing it to pool in the lower extremities. The resulting venous hypertension leads to the hallmark symptoms of PTS: chronic edema, heaviness, and in severe cases, venous ulcers that are tough to heal.
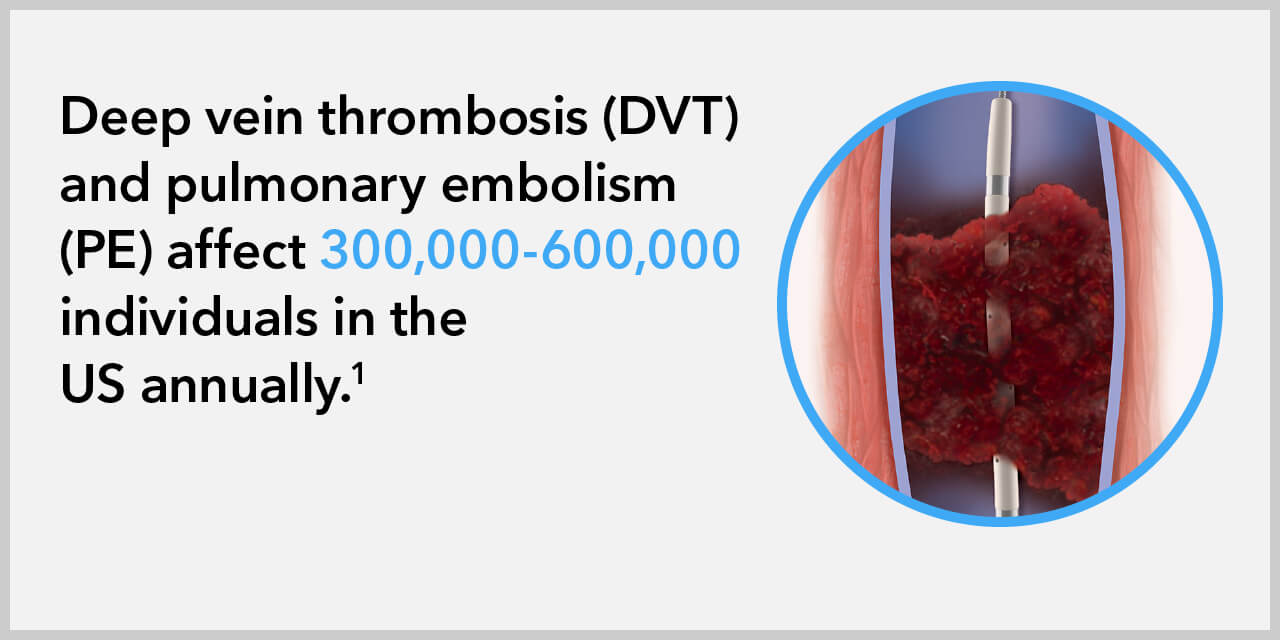
The trial sought to determine if removing these “bottlenecks” via endovascular intervention—such as balloon angioplasty or stenting—could reverse these effects. The participants in the study were those who had failed to respond sufficiently to conservative measures, representing the most challenging patient population to treat.
Medical professionals have long debated the efficacy of these interventions, as the risk of restenosis (the vein closing again) and the potential for complications have historically tempered the enthusiasm for surgical intervention in chronic cases. However, the data from this randomized trial provides a more structured evidence base for the benefits of mechanical intervention.
Trial Design and Key Outcomes
The study employed a rigorous randomized design to compare the outcomes of patients receiving endovascular therapy against those receiving optimal medical management. The primary endpoints focused on the reduction of symptoms and the improvement of the Villalta scale, a validated clinical tool used to grade the severity of post-thrombotic syndrome.
The results indicated that patients who underwent the procedure experienced a more significant decrease in leg swelling and a marked improvement in their ability to perform daily activities. Notably, the endovascular group reported a higher rate of symptom resolution and a decrease in the need for aggressive compression therapy.
| Feature | Medical Management | Endovascular Therapy |
|---|---|---|
| Primary Approach | Compression stockings & activity | Balloon angioplasty/stenting |
| Goal | Symptom mitigation | Mechanical restoration of flow |
| Patient Experience | Consistent daily maintenance | Procedural intervention |
| Key Benefit | Low procedural risk | Higher rate of symptom reversal |
While the procedural group showed superior symptomatic improvement, the researchers also monitored for safety. The trial noted that while the intervention is generally safe, it is not without risks, including potential vessel injury or the recurrence of clots, which requires careful post-operative monitoring and often continued anticoagulation therapy.
Who Benefits Most from Intervention?
Not every patient with a history of DVT is a candidate for endovascular therapy. The trial emphasizes that the benefit is most pronounced in patients with demonstrable venous obstruction. This means that imaging, such as duplex ultrasound or venography, must confirm that there is a physical blockage that can be surgically bypassed or opened.
For those with “valvular insufficiency”—where the vein is open but the valves are simply broken—the benefits of endovascular therapy are less clear. The focus of this trial was specifically on the obstruction component of the syndrome. This distinction is critical for clinicians when deciding whether to refer a patient for a surgical consultation or to double down on compression therapy.
The implications for public health are substantial. Given the prevalence of DVT in aging populations and those with comorbid conditions like obesity or cancer, a larger number of people are living with the long-term consequences of venous thromboembolism. Moving the needle from “managing” a chronic condition to “treating” the underlying cause could reduce the long-term healthcare costs associated with ulcer care and disability.
Clinical Considerations and Next Steps
Despite the positive results, the medical community is looking for more data on the long-term durability of these stents and angioplasties. The “recoil” effect, where the vein narrows again over several years, remains a point of concern for vascular surgeons.
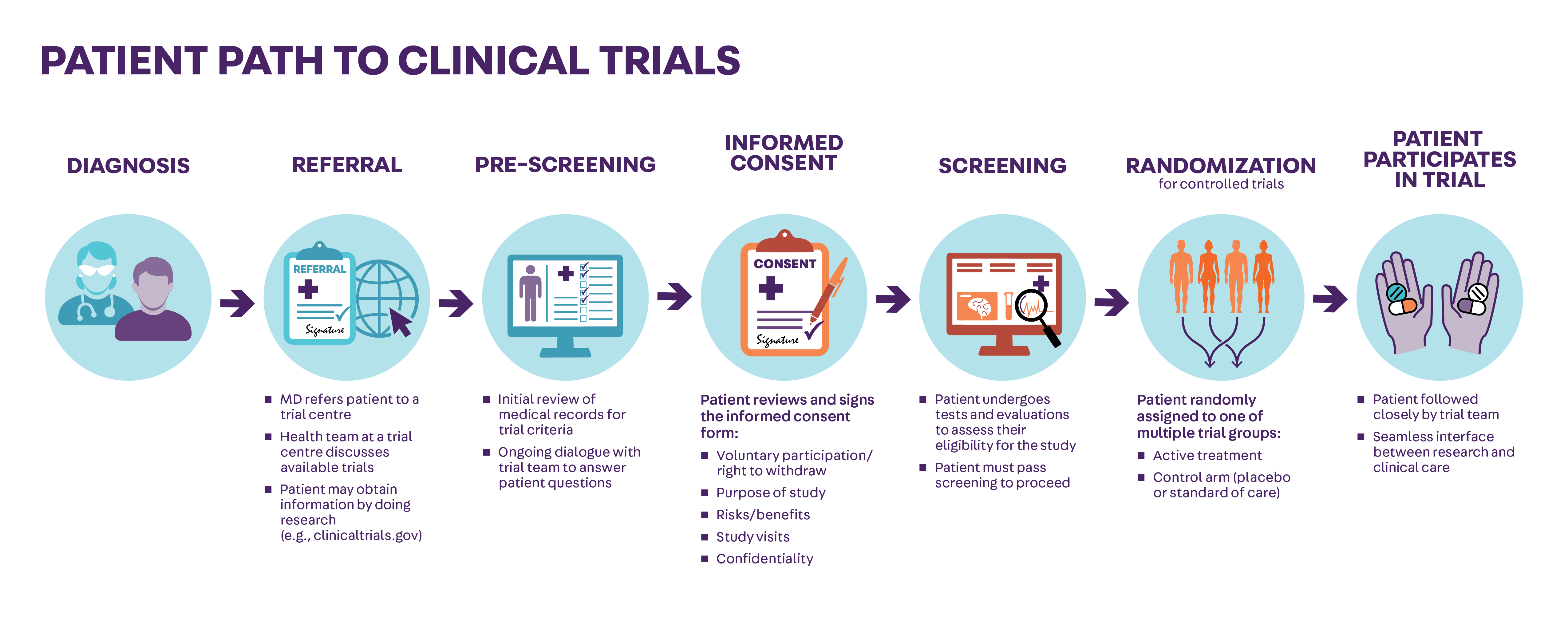
the trial highlights the necessity of a multidisciplinary approach. The most successful outcomes were not just the result of the procedure itself, but the combination of the intervention followed by a strict adherence to post-operative care and lifestyle modifications.
Patients seeking more information on the management of chronic venous insufficiency and post-thrombotic syndrome can find official guidelines and patient resources through the Society for Vascular Surgery or the Centers for Disease Control and Prevention (CDC) regarding DVT prevention and recovery.
Disclaimer: This article is provided for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
The next phase of clinical focus will likely involve long-term follow-up studies to determine the five- and ten-year patency rates of the interventions used in this trial, providing a clearer picture of the permanent efficacy of endovascular therapy for this population.
Do you or a loved one have experience managing post-thrombotic syndrome? We invite you to share your thoughts and experiences in the comments below.

