For many families, the moment a surgeon announces a successful operation on a child with congenital heart disease feels like the finish line. The tension of the operating room evaporates, replaced by the relief of a stable heartbeat and a recovering patient. However, as a physician and medical writer, I have seen that this milestone is often not the end of the journey, but rather the beginning of a lifelong commitment to cardiovascular health.
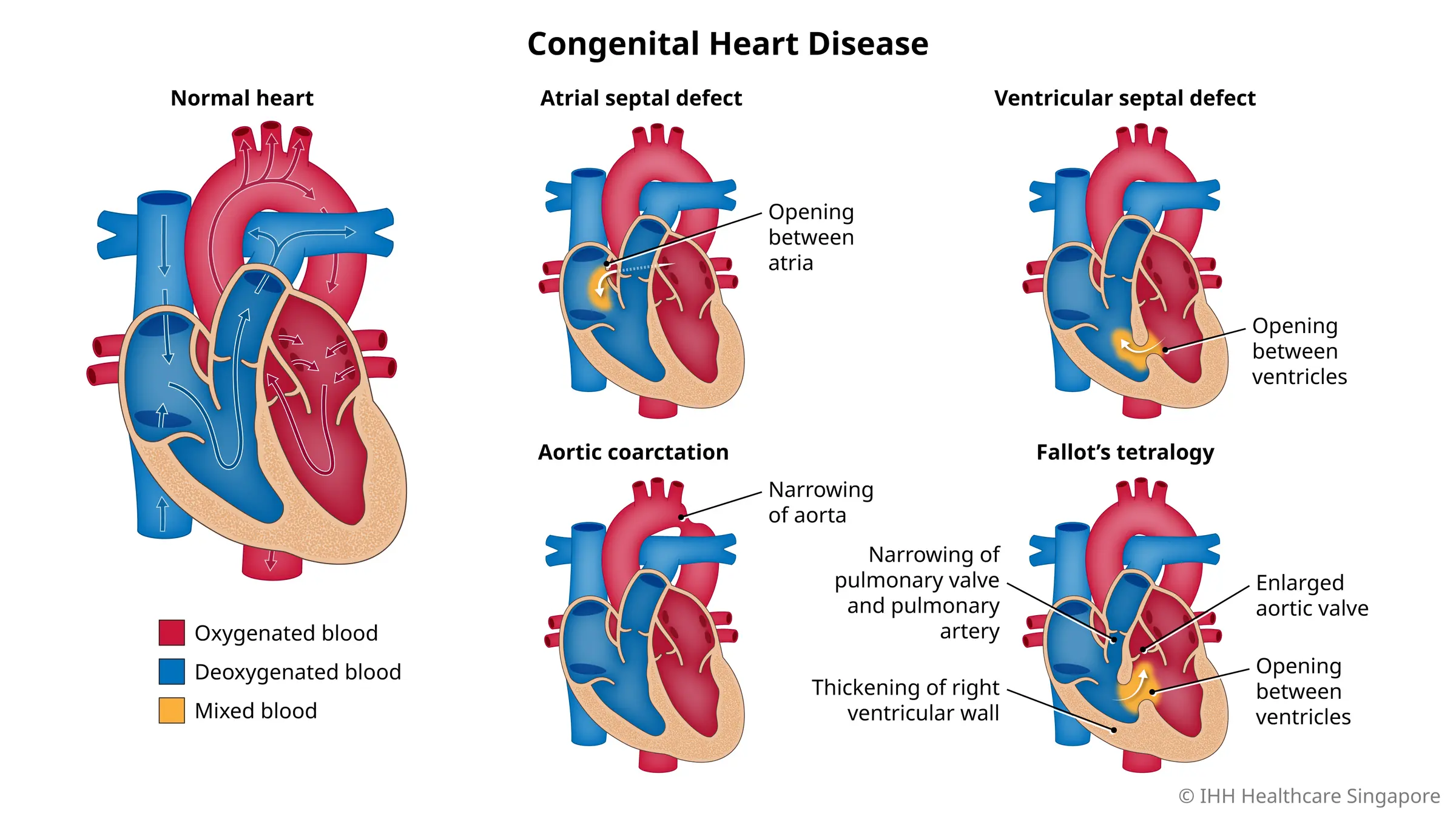
Congenital heart disease (CHD)—structural problems with the heart present at birth—requires a paradigm shift in how patients and caregivers view recovery. While modern surgical techniques have dramatically increased survival rates, the heart is a dynamic organ. A repair performed in infancy must function through the rapid growth of childhood, the hormonal shifts of adolescence, and the physiological demands of adulthood.
The necessity for lifelong management of congenital heart disease stems from the fact that surgical “fixes” are often palliative or corrective for a specific moment in time, but they do not “cure” the underlying predisposition of the heart to develop further complications. From valve leakages to rhythm disturbances, the long-term trajectory of a CHD patient requires a specialized transition from pediatric to adult care.
The Complexity of Long-Term Cardiovascular Maintenance
The primary challenge in managing CHD after the initial surgery is the evolution of the heart’s anatomy. A patch used to close a hole or a conduit used to route blood may not grow at the same rate as the child’s body. Over time, these synthetic materials can degrade or become too small, leading to a decrease in efficiency and the potential need for repeat interventions.
Beyond the structural integrity of the repair, patients face a heightened risk of arrhythmias. Scar tissue from previous surgeries can interfere with the heart’s electrical signaling, potentially leading to tachycardia or other irregular heartbeats that may only manifest years or even decades after the primary operation. This makes regular monitoring via echocardiograms and EKGs essential, even when the patient feels entirely asymptomatic.
the hemodynamic changes caused by CHD can place chronic stress on the pulmonary arteries and the right ventricle. If left unmonitored, this can lead to pulmonary hypertension, a condition where high blood pressure in the lungs forces the heart to function harder, eventually leading to heart failure if not managed with precise pharmacological and lifestyle interventions.
Key Monitoring Milestones and Risk Factors
To understand the scope of long-term care, it is helpful to gaze at the specific areas of concern that clinicians monitor throughout a patient’s life. The focus shifts from immediate survival to the preservation of heart function and the prevention of secondary complications.
| Phase of Life | Primary Clinical Focus | Common Risks |
|---|---|---|
| Childhood | Growth & Development | Stenosis of repaired areas, growth failure |
| Adolescence | Physical Activity Limits | Exercise-induced arrhythmias, valve dysfunction |
| Early Adulthood | Transition to Adult Care | Psychological impact, medication adherence |
| Mature Adulthood | Chronic Organ Stress | Heart failure, pulmonary hypertension |
The Critical Window: Transitioning to Adult Congenital Heart Disease (ACHD)
One of the most vulnerable periods for a patient is the transition from a pediatric cardiologist to an Adult Congenital Heart Disease (ACHD) specialist. This transition is not merely a change of doctors; it is a shift in the philosophy of care. Pediatric care focuses on growth and correction, while adult care focuses on stability and the management of chronic conditions.
Many patients fall through the cracks during this window, often stopping their follow-up appointments once they reach their late teens because they feel “cured.” This gap in care is dangerous. According to the American Heart Association, the prevalence of adults living with CHD is increasing rapidly due to the success of pediatric surgeries, creating an urgent need for specialized adult care centers that understand the nuances of congenital anatomy.
A successful transition involves “transition clinics” where patients are taught to articulate their own medical history—knowing exactly which surgery they had, which vessels were diverted, and which medications they are taking. This self-advocacy is a critical survival skill for the adult CHD patient.
Holistic Health and Preventative Strategies
Because the heart is already compromised or has undergone significant trauma, patients with CHD have a lower “reserve” than the general population. This means that traditional risk factors for heart disease—such as hypertension, high cholesterol, and diabetes—are far more dangerous for a CHD survivor than for someone with a healthy heart.
- Blood Pressure Management: Even mild hypertension can put undue strain on a surgically repaired ventricle, accelerating the onset of heart failure.
- Infective Endocarditis Prevention: Some CHD patients remain at higher risk for heart infections. Understanding when to use prophylactic antibiotics before dental procedures is a vital part of lifelong care.
- Psychosocial Support: Living with a chronic heart condition from birth can lead to anxiety and depression. Mental health support is an integral part of the clinical pathway to ensure patients remain compliant with their medical regimens.
The goal of this comprehensive approach is to ensure that the patient does not just survive, but thrives. This includes navigating the complexities of insurance, employment disclosures, and the planning of future pregnancies, as pregnancy can place significant stress on a congenital heart.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
As medical technology advances, the focus is shifting toward “precision monitoring,” using wearable tech and advanced imaging to detect failures in surgical repairs before they become symptomatic. The next major checkpoint for the community will be the integration of AI-driven predictive modeling to determine the exact timing for re-intervention surgeries, reducing the risks associated with emergency procedures.
We invite you to share your experiences or questions regarding long-term heart health in the comments below to help build a supportive community for CHD survivors and their families.

