The Irish government has secured multi-billion-euro agreements to ensure the steady supply of essential medicines over the next three years, a move intended to stabilize the healthcare system and protect patient access to life-saving drugs. Yet, as these massive financial commitments are finalized, a critical gap has emerged: the agreements contain virtually no reference to the procurement or strategic rollout of vaccines.
This omission has sparked a sharp critique from policymakers and health advocates, who argue that the State is prioritizing the treatment of disease over the prevention of it. By focusing almost exclusively on curative pharmaceuticals, the government may be overlooking the most cost-effective tool in the public health arsenal—vaccination—leaving a significant portion of the population vulnerable to preventable illnesses that eventually place an even greater burden on the HSE.
For clinicians, this disconnect is more than a budgetary oversight; it is a missed opportunity to shift the paradigm of Irish healthcare from “sick care” to true preventative medicine. When billions are allocated to manage chronic conditions, the failure to invest in the vaccines that could prevent those conditions—or their debilitating complications—creates a systemic inefficiency that patients will ultimately feel.
The Cost of Omission in Preventative Care
The recent agreements are designed to provide long-term price stability and supply security for a wide array of medications. While What we have is a victory for patients relying on daily prescriptions for chronic illness, the Labour Party and other critics have pointed out that the silence regarding vaccines is deafening. The argument is simple: it is far more sustainable to prevent a disease than to treat its long-term sequelae.
Vaccines are not merely tools for pandemic response; they are the bedrock of geriatric and pediatric health. When vaccines are excluded from high-level procurement strategies, the rollout of new protections often becomes fragmented, relying on sporadic funding or leaving patients to pay out-of-pocket. This creates a tiered system of health where preventative care is a luxury rather than a standard of public health.
The tension here lies in the “curative bias” of modern healthcare spending. It is often politically easier to fund a drug that treats a visible, existing crisis than to fund a vaccine that prevents a crisis from ever happening. However, from a public health perspective, the latter is almost always the more prudent investment.
The Shingles Example: Beyond the Rash
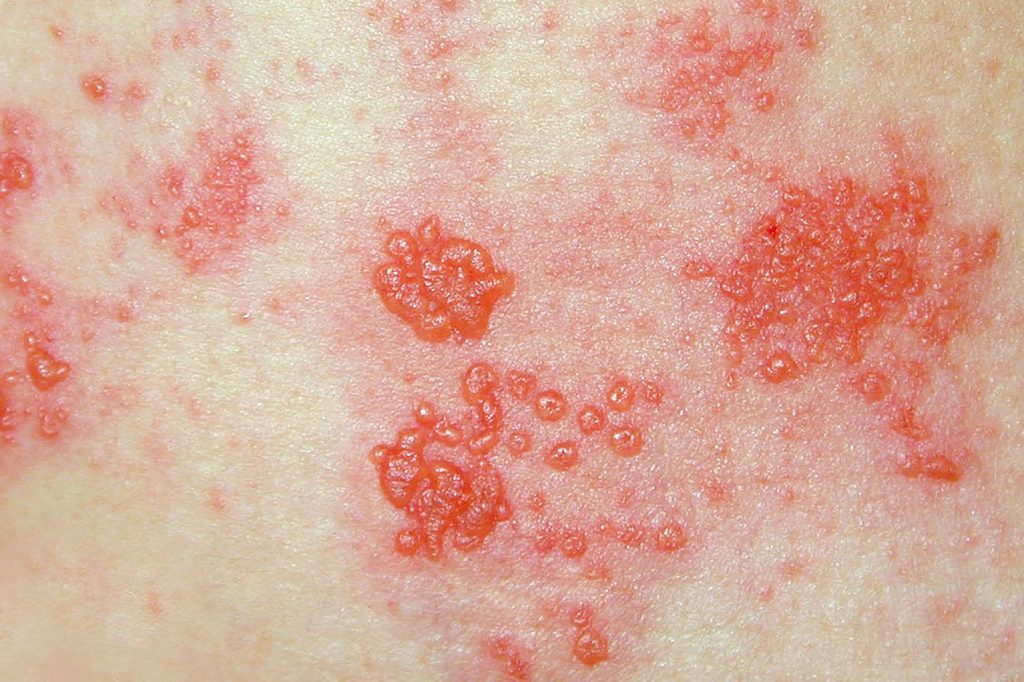
The case of the shingles vaccine (Herpes Zoster) serves as a potent example of what is at stake. Shingles is not merely a painful skin rash; for many, especially the elderly, it leads to postherpetic neuralgia (PHN)—a chronic, stabbing nerve pain that can last for years and severely diminish quality of life.

Recent evidence highlighted in The Irish Times underscores the growing clinical benefit of shingles vaccination in reducing these severe outcomes. But the value proposition for the vaccine is expanding. New research from the United States, as reported by MedPage Today, suggests a potential link between shingles vaccination and a reduced risk of developing dementia. While more research is needed to establish a definitive causal link, the possibility that a vaccine could offer neuroprotective benefits adds a massive layer of value to its administration in an aging population.
If the State is spending billions to manage the fallout of dementia and chronic pain in the elderly, the failure to integrate shingles vaccination into a national strategic agreement is a clinical contradiction. Preventing PHN and potentially lowering dementia risk would directly reduce the long-term demand for the very drugs the government is currently spending billions to secure.
Comparing the Curative and Preventative Models
To understand why this policy gap matters, one must look at the trajectory of a patient’s journey through the healthcare system. A curative-heavy approach waits for the pathology to manifest, while a preventative approach interrupts the disease process entirely.
| Feature | Curative Drug Focus | Preventative Vaccine Focus |
|---|---|---|
| Primary Goal | Management of existing disease | Prevention of disease onset |
| System Impact | High long-term maintenance cost | High upfront cost, long-term savings |
| Patient Experience | Treatment of symptoms/complications | Avoidance of illness and disability |
| Health Outcome | Stabilization or remission | Primary prevention of morbidity |
The Burden on the Aging Population
The stakes are particularly high for Ireland’s aging demographic. As the population grows older, the prevalence of comorbidities increases. A patient who suffers from shingles is more likely to experience a decline in functional independence, which in turn increases their reliance on the HSE for home care and pharmaceutical support.
By neglecting to include vaccines in these multi-billion-euro deals, the State risks a “failure of demand” strategy—where the system is so focused on treating the current queue of sick patients that it fails to stop new patients from entering that queue. This is not just a financial miscalculation; it is a clinical one. As a physician, I see the daily struggle of patients managing multiple prescriptions for conditions that could have been mitigated by a single dose of a vaccine years prior.
the lack of a clear vaccine strategy in these agreements leaves the public in a state of uncertainty. When the State does not signal a long-term commitment to vaccine procurement, uptake remains lower than optimal, and the “herd immunity” required to protect the most vulnerable is never fully realized.
Disclaimer: This article is provided for informational purposes only and does not constitute medical advice. Patients should consult with their healthcare provider regarding vaccinations and medication.
The next critical checkpoint for this issue will be the upcoming parliamentary reviews of the health budget and the formal implementation phase of the drug agreements, where opposition members are expected to press for a dedicated vaccine supplement to the existing contracts. Whether the government will pivot toward a more holistic, preventative model remains to be seen.
Do you believe the state should prioritize prevention over treatment in its healthcare spending? Share your thoughts in the comments or share this article to join the conversation.