For most, Mother’s Day is a celebration of kinship, resilience, and the quiet strength of the women who anchor their families. But for a growing number of American families, the holiday is marked by a profound and preventable void. In the United States, the act of bringing new life into the world has become an increasingly dangerous gamble, particularly for women of color and those living in underserved regions.
The paradox is stark: the U.S. Possesses some of the most advanced medical technology and highly trained specialists in the world, yet it consistently reports the highest maternal mortality rate among developed nations. While the “Ivory Tower” of academic medicine produces groundbreaking research on fetal development and surgical interventions, the actual outcomes for mothers on the ground reveal a systemic failure that transcends the walls of the clinic.
This crisis is not merely a medical failure but a sociological one. The data suggests that maternal death is less about the lack of clinical tools and more about the lack of equitable access to those tools. From “maternity deserts” in rural Appalachia to the implicit biases encountered in urban hospitals, the American healthcare system is failing to protect the very people It’s designed to serve.
The Statistical Divide: A Crisis of Equity
The most damning aspect of the U.S. Maternal health crisis is its uneven distribution. Maternal mortality is not an equal-opportunity tragedy; it is sharply divided along racial and socioeconomic lines. According to data from the Centers for Disease Control and Prevention (CDC), Black women are significantly more likely to die from pregnancy-related complications than white women, regardless of their income level or educational attainment.
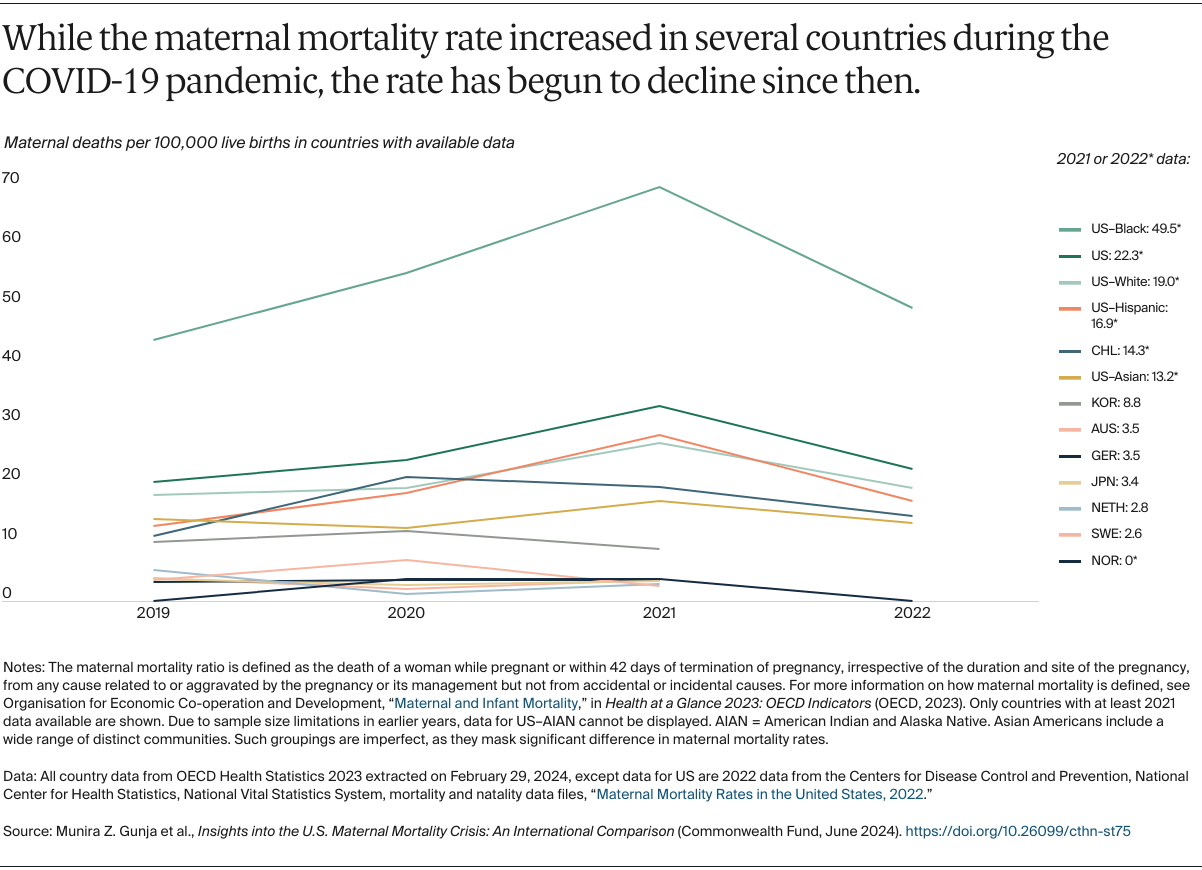
This disparity indicates that the issue is not simply a matter of poverty or lack of insurance, but rather a systemic failure in the quality of care provided to Black mothers. Implicit bias—where healthcare providers may subconsciously dismiss the pain or concerns of minority patients—often leads to delayed diagnoses of life-threatening conditions like preeclampsia or postpartum hemorrhage.
| Demographic Group | Relative Risk Level | Primary Contributing Factors |
|---|---|---|
| Non-Hispanic White | Baseline | Chronic conditions, advanced maternal age |
| Non-Hispanic Black | High (2-3x Baseline) | Systemic bias, chronic stress, access gaps |
| Hispanic/Latina | Moderate to High | Language barriers, insurance instability |
| Rural Populations | Elevated | Hospital closures, “maternity deserts” |
Post-Pandemic Trends and the ‘Obstetric’ Nuance
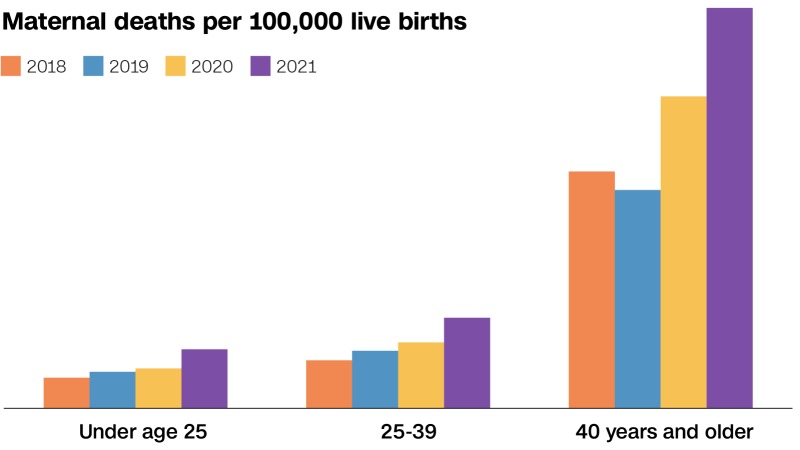
The COVID-19 pandemic acted as a catalyst, exposing the fragility of the maternal health infrastructure and causing a spike in deaths. However, recent analysis suggests a nuanced shift in the data. Reports indicate that “obstetric-only” maternal deaths—those caused directly by the complications of pregnancy and childbirth—began to fall after the peak of the pandemic.
Yet, this slight decline in acute obstetric deaths does not signal a total victory. The broader category of maternal mortality includes deaths that occur up to a year after childbirth. Many of these are linked to indirect causes—pre-existing conditions like hypertension or diabetes that are exacerbated by the stress of pregnancy—as well as mental health crises and substance use disorders.
The distinction is critical: while the medical community has improved its immediate response to birth-related emergencies, the long-term support system for the “fourth trimester” remains dangerously thin. The transition from being a patient in a delivery ward to a mother at home is where many women fall through the cracks of a fragmented healthcare system.
Moving From ‘Mom’ to ‘Mother’
There is a vital conceptual difference between caring for “Mom” during the clinical window of pregnancy and caring for a “Mother” as a whole person. Much of the U.S. Healthcare model is designed around the fetus, with the mother serving as the vessel. Once the baby is delivered, the clinical intensity drops precipitously, often leaving the mother with minimal follow-up care.
Advocates argue that the U.S. Must shift toward a holistic model of maternal health that includes:
- Extended Postpartum Care: Moving beyond the standard six-week checkup to provide comprehensive mental and physical health screenings for a full year.
- Community-Based Support: Integrating doulas and midwives into the primary care team to provide emotional support and advocacy, particularly for marginalized women.
- Addressing Social Determinants: Recognizing that housing instability, food insecurity, and chronic stress are as impactful to maternal survival as clinical interventions.
- Standardized Safety Bundles: Implementing rigorous, evidence-based protocols across all hospitals to treat hemorrhage and hypertension uniformly, regardless of the patient’s background.
The Knowns and the Unknowns
What is known is that the majority of maternal deaths in the U.S. Are preventable. The CDC has consistently highlighted that a significant percentage of fatalities could have been avoided with timely intervention and adherence to standard care protocols. We also know that countries with universal prenatal and postpartum care report drastically lower mortality rates.
What remains unknown, or under-reported, is the full extent of the mental health toll. While physical deaths are tracked, the “near-misses”—women who survive severe complications but are left with lifelong trauma or disability—are rarely quantified. The exact impact of recent legislative changes regarding reproductive healthcare access on maternal mortality rates is still being analyzed by public health researchers.
“We do a lot for the baby, and we do a lot for the immediate act of birth, but we do far too little for the woman who remains after the nursery is filled. To save mothers, we have to see them as patients in their own right, not just as conduits for the next generation.”
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
The next critical benchmark for U.S. Maternal health will be the release of the updated CDC maternal mortality data and the progress of states in extending Medicaid coverage for postpartum care from 60 days to a full year. These policy shifts will determine whether the U.S. Can finally close the gap between its medical capabilities and its actual outcomes.
We want to hear from you. How has your community addressed maternal health, or where do you see the biggest gaps in care? Share your thoughts in the comments below.

