For most of the 20th century, the medical community viewed cancer as a disease of the twilight years—a consequence of the accumulated cellular damage that comes with aging. But in the clinics and oncology wards of the 21st century, that narrative is shifting. Doctors are increasingly treating patients in their 20s, 30s, and 40s for malignancies that were once rare in people under 50.
This trend, now categorized as “early-onset cancer,” is not a statistical fluke. Data indicates a steady rise in several cancer types among younger adults since the 1990s, with colorectal, breast, kidney, and uterine cancers showing the most significant upticks. While the increase is global, it is particularly pronounced in industrialized nations, prompting a search for the environmental and biological triggers driving this demographic shift.
As a physician and medical writer, I have watched this trend move from a series of anecdotal concerns in medical journals to a public health priority. The challenge lies in the fact that there is no single “smoking gun.” Instead, researchers believe we are seeing the cumulative effect of a modern environment—one defined by ultra-processed diets, sedentary behavior, and a chemical landscape that the human body was not evolved to handle.
The Metabolic Driver: Diet and the Obesity Epidemic
One of the most consistent links in early-onset cancer research is the rise of metabolic dysfunction. The World Health Organization reports that global obesity rates have more than doubled since 1990, a trend that mirrors the rise in early-onset malignancies. This is not merely about weight, but about the systemic inflammation and hormonal disruptions that accompany obesity.

Central to this is the proliferation of ultra-processed foods (UPFs). Diets heavy in refined sugars, emulsifiers, and processed meats are linked to a disruption of the gut microbiome—the trillions of bacteria that regulate our immune system and protect the lining of our intestines. When the microbiome is compromised, chronic inflammation can set in, creating a fertile environment for DNA mutations and tumor growth.
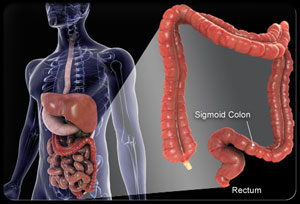
Sedentary lifestyles exacerbate this risk. A lack of physical activity affects how the body processes insulin and regulates estrogen, both of which are critical factors in the development of breast and uterine cancers. In the case of colorectal cancer, researchers are particularly interested in how a low-fiber, high-sugar diet alters the gut environment, potentially accelerating the growth of precancerous polyps in adults decades younger than previously expected.
Environmental Toxins and the Microplastic Question
While lifestyle factors provide a clear lead, scientists are now looking closer at the “invisible” exposures of modern life. There is growing concern regarding microplastics—tiny polymer particles now detected in human blood, lung tissue, and placentas. Because microplastics can act as endocrine disruptors and trigger oxidative stress, researchers are investigating whether they contribute to cellular damage and DNA mutations.
Beyond plastics, the focus has shifted to “forever chemicals,” known as PFAS (per- and polyfluoroalkyl substances). These industrial chemicals, found in everything from non-stick cookware to firefighting foams, do not break down in the environment or the human body. Their ability to mimic hormones and suppress immune responses makes them a prime suspect in the rise of early-onset kidney and uterine cancers.
However, the evidence here is more fragmented than the data on obesity. While the biological plausibility is high, proving a direct causal link between a specific chemical exposure and a cancer diagnosis in a 35-year-old is complex, as most people are exposed to a “cocktail” of different toxins over several decades.
The Screening Paradox: Detection vs. Incidence
It is important to distinguish between a rise in incidence (more people getting cancer) and a rise in detection (finding cancer that was already there). Part of the increase in early-onset diagnoses is a success story of modern medicine: we are simply getting better at finding it.
Increased public awareness and the adoption of more sensitive imaging technologies mean that cancers are being caught earlier. Medical guidelines have shifted to reflect the changing risk profile of younger adults. For example, the recommended age to begin colorectal cancer screening in the U.S. Was lowered from 50 to 45 to combat the rise in early-onset cases.
| Cancer Type | Previous Typical Screening Age | Current/Updated Guidance | Primary Driver of Change |
|---|---|---|---|
| Colorectal | 50 | 45 | Rising early-onset incidence |
| Breast | 50 | 40–45 (varies by org) | Increased detection/risk profiles |
| Cervical | 21 (Pap) | 25 (HPV testing) | Improved molecular testing |
The Clinical Reality: Why Early-Onset Cancer is Different
Despite the rise in diagnoses, there is a silver lining: overall cancer death rates for many types have declined due to breakthroughs in immunotherapy and targeted treatments. However, early-onset cancers often present a unique clinical challenge. Because younger patients are not typically viewed as “high risk,” both patients and providers may dismiss early warning signs as minor issues.
This often leads to a dangerous delay in diagnosis. Early-onset colorectal and breast cancers are frequently discovered at more advanced stages than those in older adults. When a 30-year-old experiences rectal bleeding or unusual fatigue, it is often attributed to hemorrhoids or stress rather than malignancy, allowing the cancer to progress unchecked.
Medical professionals urge young adults to be vigilant. Symptoms that should never be ignored include:
- Unexplained, persistent weight loss.
- Changes in bowel habits or rectal bleeding.
- Unusual lumps in the breast, armpit, or groin.
- Chronic, unexplained fatigue that does not improve with rest.
- Persistent abdominal pain or bloating.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
The next major milestone in understanding this trend will be the release of updated longitudinal data from the National Cancer Institute (NCI) and the World Health Organization, which are currently tracking the long-term impact of dietary shifts and environmental toxins on the “millennial” and “Gen Z” cohorts. These findings will likely dictate whether further shifts in screening ages are necessary for the general population.
Do you have questions about early screening or the impact of lifestyle on long-term health? Share your thoughts in the comments or share this article with someone who needs to see it.