For the parents of a three-year-old boy, the symptoms seemed familiar and manageable: a persistent, wheezy cough that flared up periodically, mimicking the classic signs of childhood asthma or recurrent bronchiolitis. Like many families navigating the early years of respiratory health, they followed the standard medical playbook, utilizing nebulizers and oral steroids to open the child’s airways. However, the relief was always temporary, and the “asthma” refused to resolve.
What appeared to be a common respiratory struggle was actually a rare and dangerous masquerade. As detailed in a case report published in Cureus, the child was not suffering from inflammatory airway disease, but from a thoracic neuroblastoma—a malignant tumor arising from primitive nerve cells that had grown large enough to physically compress his lungs and windpipe.
The case serves as a critical reminder for pediatricians and parents alike: when a child fails to respond to standard asthma protocols, the diagnostic lens must widen. In this instance, the transition from a suspected common ailment to a life-threatening oncological diagnosis happened only after clinicians questioned why the “wheezing” was refractory to treatment.
Neuroblastoma is the most common extracranial solid tumor found in childhood, typically originating in the adrenal glands or the sympathetic nervous system. While most cases occur in the abdomen, thoracic presentations are less common and particularly deceptive because they often present as respiratory distress, leading to significant delays in diagnosis.
The Diagnostic Maze: When Asthma Isn’t Asthma
The clinical journey began with a pattern of recurrent respiratory episodes. The child presented with a wheezy chest and coughing, symptoms that are ubiquitous in pediatric primary care. Initial interventions focused on the most likely culprits: viral infections and hyper-responsive airways. The patient was treated with traditional asthma therapies, including bronchodilators and corticosteroids, which provided transient improvement but failed to cure the underlying issue.
The “red flag” in this case was the recurrence. In typical pediatric asthma, triggers are usually identifiable—such as allergens, cold air, or viral illness—and the response to corticosteroids is generally robust. When the child continued to experience respiratory distress despite these interventions, the medical team shifted their focus from inflammation to obstruction.
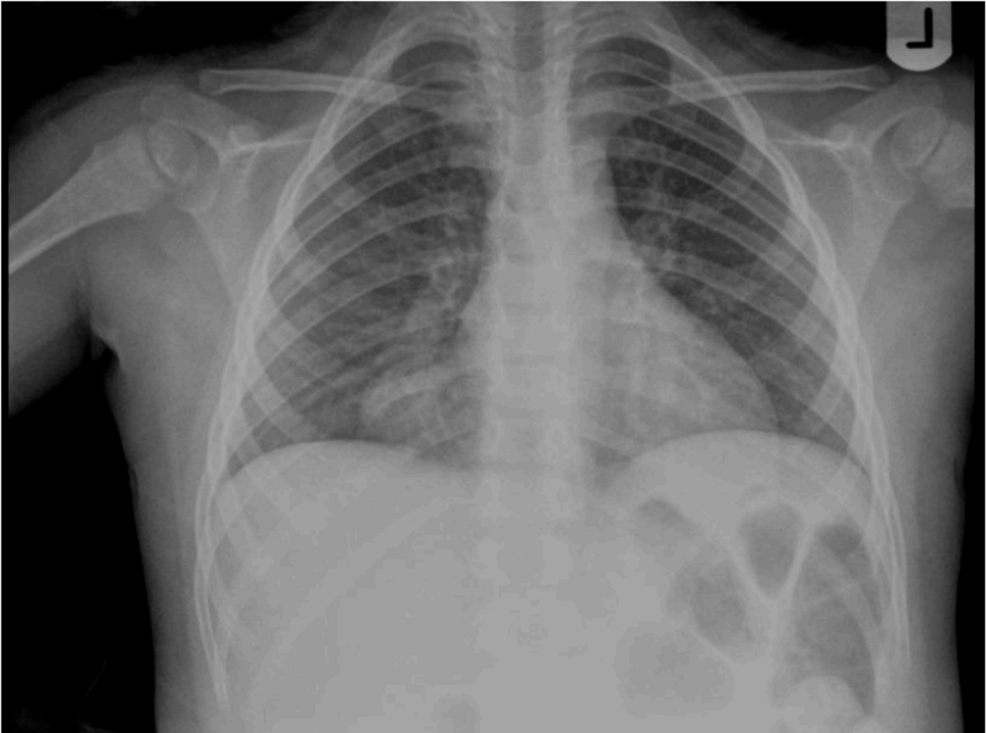
A chest X-ray eventually revealed the truth: a significant mass in the right upper lobe of the chest and the mediastinum. This was followed by a contrast-enhanced CT scan, which provided a clearer picture of the pathology. The imaging identified a large, well-defined mass measuring approximately 6.5 x 5 x 4 cm. This tumor was not just occupying space; it was actively compressing the surrounding lung tissue and shifting the mediastinal structures, creating the “wheezing” sound that had been mistaken for asthma.
Understanding Thoracic Neuroblastoma
To understand why this tumor mimics asthma, one must look at the anatomy of the chest. Neuroblastomas develop from neural crest cells—embryonic cells that migrate during fetal development to form the sympathetic ganglia. When these cells fail to mature and instead proliferate into a tumor in the thoracic cavity, they can press against the trachea or the primary bronchi.
This external pressure narrows the airway, creating a “fixed” obstruction. Unlike asthma, where the narrowing is caused by the swelling of the airway walls and mucus production, the narrowing here was mechanical. This explains why steroids—which reduce swelling—offered little to no long-term relief.
The biopsy and histopathological examination confirmed the diagnosis of neuroblastoma. These tumors are graded based on their cellular maturity and the extent of their spread. In this case, the immediate priority was the relief of the airway obstruction and the removal of the primary tumor mass.
Comparing Respiratory Presentations
Because the symptoms of thoracic neuroblastoma can so closely mirror common pediatric respiratory issues, clinicians look for specific divergent patterns to trigger advanced imaging.
| Feature | Typical Pediatric Asthma/Bronchiolitis | Thoracic Neuroblastoma |
|---|---|---|
| Response to Steroids | Generally high/significant improvement | Minimal or no long-term response |
| Symptom Pattern | Episodic, often triggered by allergens | Persistent or progressively worsening |
| Chest X-Ray | Hyperinflation or patchy infiltrates | Visible mediastinal or pulmonary mass |
| Physical Exam | Diffuse wheezing throughout lungs | Localized wheezing or diminished breath sounds |
Treatment and Path to Recovery
Once the diagnosis was confirmed, the medical team implemented a multidisciplinary approach. The primary goal was the surgical resection of the tumor to alleviate the pressure on the lungs and prevent further growth. Following the surgery, the patient underwent chemotherapy to target any remaining microscopic cancer cells and reduce the risk of recurrence.
The surgical removal of a thoracic mass in a three-year-old is a high-stakes procedure, requiring precise navigation around the heart, great vessels, and the delicate structures of the airway. However, once the mechanical obstruction was removed, the child’s respiratory function improved dramatically, and the “wheezing” that had defined his first three years of life vanished.
The case highlights the importance of the “differential diagnosis”—the process by which doctors list all possible causes of a symptom. In pediatric medicine, the tendency is to treat the most common condition first. While this is statistically sound, the failure of a first-line treatment must be viewed as a diagnostic clue in itself.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
The child remains under close oncological surveillance to monitor for potential relapse, a standard protocol for pediatric neuroblastoma. The next phase of care involves regular imaging and blood tests to ensure the tumor remains in remission, with follow-up appointments scheduled at six-month intervals for the next two years.
Do you have experience navigating complex pediatric diagnoses? Share your thoughts or questions in the comments below.