For decades, the biggest hurdle in deep-tissue imaging and neuromodulation has been a simple matter of physics: the human body is remarkably opaque. While we can use ultrasound to see a fetus in the womb or MRI to map a brain, using light to trigger biological responses deep within living tissue has traditionally required a “brute force” approach—specifically, drilling holes in the skull or inserting invasive fiber-optic cables directly into the organ of interest.
A recent breakthrough detailed in Physics World suggests a more elegant solution. Researchers have developed ultrasound-activated nanoparticles that act as internal lamps, converting sound waves into visible light. By bypassing the need for physical probes, this technology could transform how we treat neurological disorders and monitor internal cellular activity in real time.
As a former software engineer, I tend to view these challenges as a “last mile” delivery problem. We have the tools to create light and the tools to send sound deep into the body, but we lacked a reliable transducer to bridge the two. This new approach essentially installs a wireless receiver inside the tissue, allowing clinicians to “switch on” light exactly where and when it is needed using non-invasive ultrasound pulses.
The Physics of Sonoluminescence
The core of this technology lies in a phenomenon known as sonoluminescence. When ultrasound waves pass through a liquid, they create tiny bubbles through a process called acoustic cavitation. As these bubbles rapidly expand and then violently collapse, they generate intense localized heat and pressure. In a vacuum, this is just a physical curiosity; however, when specific nanoparticles are present, this energy can be harnessed to emit photons.

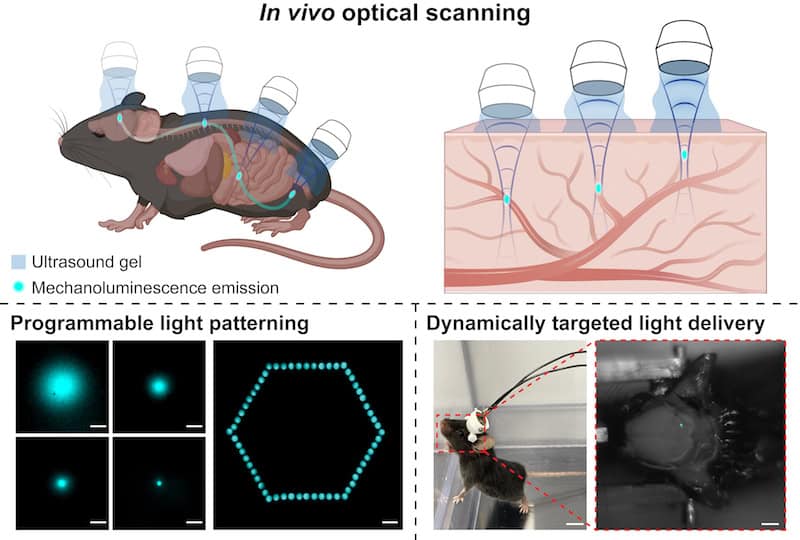
The nanoparticles are engineered to be “mechanoluminescent,” meaning they emit light when subjected to mechanical stress. When the ultrasound-induced bubbles collapse around these particles, the resulting shockwave triggers a flash of light. Because ultrasound waves travel through biological tissue with far less scattering than light waves, the “trigger” can reach depths that would be impossible for a laser or LED to penetrate.
This process effectively turns the body’s own fluid environment into a medium for light generation. Rather than trying to push a photon from the outside in, the researchers are creating the photon on the inside, precisely at the site of the nanoparticle.
Unlocking Deep-Tissue Optogenetics
The most immediate and provocative application of this research is in the field of optogenetics. This is a biological technique that involves genetically modifying specific neurons to express light-sensitive ion channels. Once modified, these neurons can be turned “on” or “off” using a pulse of light, allowing scientists to control brain activity with unprecedented precision.
Until now, optogenetics has been largely confined to laboratory settings or invasive surgeries because the light source had to be physically implanted. The introduction of ultrasound-activated nanoparticles removes this barrier. By injecting these particles into a target area—such as the deep nuclei of the brain or the heart—and applying external ultrasound, researchers can trigger the light-sensitive neurons without a single incision.
The implications for treating chronic conditions are significant. Potential applications include:
- Parkinson’s Disease: Precisely stimulating the subthalamic nucleus to reduce tremors without the need for permanent deep-brain stimulation (DBS) electrodes.
- Chronic Pain Management: Inhibiting pain-signaling neurons in the spinal cord using targeted light pulses.
- Cardiac Regulation: Using light to pace heart cells or treat arrhythmias with higher specificity than electrical stimulation.
Comparing Light Delivery Methods
To understand why this shift is critical, it is helpful to compare the current gold standard of light delivery with this emerging nanoparticle approach.
| Feature | Fiber-Optic Implants | Ultrasound Nanoparticles |
|---|---|---|
| Invasiveness | High (Requires Surgery) | Low (Injectable/Non-invasive) |
| Tissue Damage | Risk of scarring/inflammation | Minimal mechanical stress |
| Depth Reach | Limited by cable length | Deep (Limited by ultrasound) |
| Precision | Fixed location | Adjustable via ultrasound focus |
Constraints and the Path to Clinical Use
Despite the promise, the transition from a physics experiment to a medical treatment is fraught with challenges. The first is biocompatibility. Any nanoparticle introduced into the bloodstream or brain must be non-toxic and, ideally, biodegradable. The body’s immune system is designed to clear foreign particles, meaning researchers must find a way to keep the nanoparticles in place long enough to be useful without triggering an inflammatory response.
There is also the question of “light budget.” The amount of light produced by a single collapsing bubble is minuscule. To achieve the threshold required to trigger an optogenetic response, a high density of nanoparticles or a high frequency of ultrasound pulses is required. However, increasing the intensity of ultrasound can lead to overheating or unintended tissue damage (thermal effects), creating a narrow window of safety and efficacy that engineers must navigate.
the delivery mechanism remains a hurdle. Getting nanoparticles across the blood-brain barrier—the body’s most restrictive security fence—requires sophisticated chemical coatings or temporary disruptions to the barrier, adding another layer of complexity to the procedure.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. The technologies discussed are currently in research stages and are not yet approved for general clinical use.
The next critical milestone for this technology will be the results of expanded in vivo longitudinal studies, which will determine if these nanoparticles can remain effective over months rather than days. Researchers are currently refining the chemical composition of the particles to increase their light yield while decreasing the required ultrasound intensity. Official updates on these trials are expected as the research moves toward peer-reviewed clinical pilot phases.
Do you think non-invasive light therapy will eventually replace electrical implants for neurological disorders? Share your thoughts in the comments below.