For anyone who has witnessed a stroke, the atmosphere is defined by a single, crushing variable: time. In the medical community, we often say “time is brain,” a shorthand for the reality that millions of neurons perish every minute a blood clot obstructs flow to the brain. Currently, the race begins in earnest only after a patient reaches the emergency room, where doctors scramble to administer clot-busting drugs or perform surgical interventions to reopen arteries.
But for a vast majority of patients, the clock runs out before they ever see a neurologist. Because the window for effective intervention is so narrow, more than 85 percent of stroke patients are unable to receive timely treatment. The challenge isn’t just logistics; it is biological. The brain is protected by the blood-brain barrier (BBB), a highly selective membrane that keeps toxins and germs out but also blocks the majority of life-saving medications from ever reaching the damaged tissue.
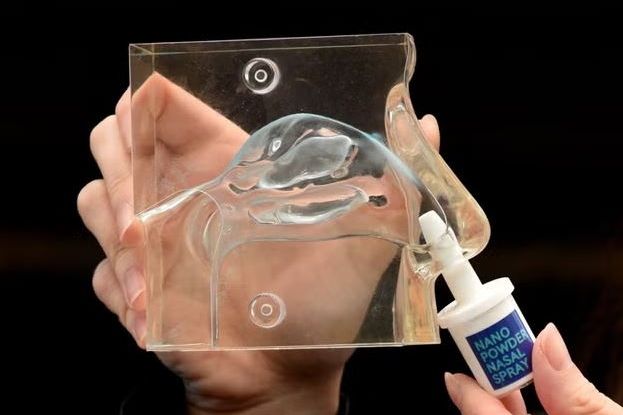
Researchers at the University of Hong Kong are now proposing a way to bypass this biological fortress entirely. By developing a “Nanopowder” nasal spray, scientists have created a delivery system that travels from the nasal cavity directly to the brain, potentially transforming the first 30 minutes of a stroke from a period of inevitable loss into a window of active rescue.
This shift from “in-hospital” to “prehospital” care could fundamentally change the prognosis for stroke survivors, offering a layer of neuroprotection that buys critical time for the more invasive procedures that follow.
The Blood-Brain Barrier: Medicine’s Greatest Hurdle
To understand why a nasal spray is a breakthrough, one must first understand why traditional drugs so often fail. The blood-brain barrier is an evolutionary masterpiece designed to protect the central nervous system (CNS), but for pharmacologists, it is a wall. Aviva Chow Shing-fung of Hong Kong University notes that the failure rate for drug candidates targeting the CNS in clinical trials exceeds 90 percent, largely because these molecules are too large or chemically incompatible to cross the BBB.
When a stroke occurs, the brain enters a state of crisis. While the core of the stroke—the area where blood flow is completely stopped—dies quickly, there is a surrounding area called the penumbra. This is the “at-risk” tissue that is malfunctioning but not yet dead. The goal of any emergency intervention is to save the penumbra.
Currently, the standard of care involves:
- Thrombolysis: Using “clot-buster” drugs like tPA to dissolve the blockage.
- Thrombectomy: A surgical procedure to physically remove the clot via a catheter.
Both are highly effective but require a hospital setting, specialized imaging, and a team of experts. By the time these are deployed, much of the penumbra has often already vanished.
How Nanopowder Bypasses the Barrier
The “Nanopowder” technology avoids the bloodstream entirely. Instead of relying on the circulatory system to carry medicine through the blood-brain barrier, the spray utilizes the nose-to-brain pathway. The nasal cavity is uniquely positioned, with olfactory and trigeminal nerves providing a direct anatomical route to the cerebrospinal fluid and brain tissue.
The spray consists of ultra-small inhalable powders that, upon administration, separate into nanoparticles. These particles are small enough to navigate the mucosal lining of the nose and migrate directly into the brain. This allows brain-protective drugs to reach the target site almost immediately after the first signs of a stroke appear.
The impact of this rapid delivery is stark. Researchers found that administering the nasal spray within 30 minutes of stroke onset could reduce the death of brain tissue by over 80 percent. This doesn’t replace the need for a hospital; rather, it acts as a “bridge” therapy, slowing the cascade of cellular death and protecting neurological and motor functions while the patient is in transit.
Comparing Treatment Paradigms
The transition to prehospital neuroprotection represents a shift in how emergency medicine views the “golden window” of stroke treatment.
| Feature | Standard Hospital Care | Nanopowder Nasal Spray |
|---|---|---|
| Primary Goal | Clot dissolution/removal | Neuroprotection (cell preservation) |
| Location | Hospital/ER | Prehospital (Ambulance/Home) |
| Delivery Route | Intravenous (IV) | Intranasal (Nose-to-Brain) |
| Key Barrier | Blood-Brain Barrier (BBB) | Bypasses the BBB |
| Timing | Post-admission | Within 30 minutes of onset |
The Human Cost of Every Second
The motivation for this research is grounded in the staggering global burden of stroke. With annual healthcare costs exceeding €755 billion worldwide, the economic impact is immense, but the human cost is higher. A stroke doesn’t just affect the patient; it reshapes the lives of families, often leaving survivors with permanent impairments in speech, movement, or cognition.
Shao Zitong of Hong Kong University emphasizes the fragility of this timeline: “After a stroke, every second matters. Even an additional 10 minutes of brain protection might determine whether a patient can walk or speak in the future.”
By shifting the focus to the prehospital stage, the Nanopowder spray aims to ensure that when a patient finally reaches the surgeon’s table, there is more viable brain tissue left to save. This approach transforms the ambulance ride from a period of passive waiting into a period of active treatment.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. In the event of a stroke, call emergency services immediately.
The next phase for this technology involves further clinical validation to determine the optimal drug combinations for the nanopowder delivery system and establishing protocols for emergency responders to administer the spray safely in the field. Official updates on human trial milestones are expected as the researchers refine the delivery mechanisms for broader clinical application.
Do you think prehospital tools like this could change how we handle medical emergencies? Share your thoughts in the comments or share this story with your network.