For millions of people, the most agonizing part of chronic pain is not the physical sensation itself, but the silence that follows a clean MRI. It is a specific, isolating kind of frustration: waking up with a level of pain that renders a workday impossible, only to be told by a specialist that “everything looks normal.” When the imaging is clear and the blood work is unremarkable, the patient is often left in a diagnostic vacuum, floating between specialists who cannot find a structural cause for their suffering.
This phenomenon—pain without a clear organic diagnosis—is not a failure of the patient’s reporting, nor is it necessarily a failure of the technology. Rather, it often represents a gap in how modern medicine categorizes pain. For decades, the medical community operated on a binary: pain was either nociceptive (caused by tissue damage, like a broken bone) or neuropathic (caused by nerve damage, like sciatica). If neither was present, the pain was frequently dismissed as psychosomatic—a polite medical term suggesting the pain exists only in the patient’s mind.
However, emerging research in neuroscience is redefining this space. We now understand that the nervous system can develop its own pathology, independent of a visible injury. This is known as nociplastic pain, a term adopted by the International Association for the Study of Pain (IASP). In these cases, the “hardware” of the body is intact, but the “software” processing the pain signals has become glitchy, amplifying normal sensations into intense distress.
The Volume Knob: Understanding Central Sensitization
To understand pain without a diagnosis, one must look at the concept of central sensitization. In a healthy system, pain acts as a vital alarm system. If you touch a hot stove, the nerves send a signal to the brain, which triggers a withdrawal reflex. In a sensitized system, however, the alarm system becomes hyper-reactive. The threshold for what the brain perceives as “painful” drops significantly.
Medical professionals often describe this as a “volume knob” that has been turned up too high and stuck there. For a person with central sensitization, a light touch on the skin or a mild change in temperature can be interpreted by the brain as a severe threat. Because this process happens at the level of the central nervous system—the spinal cord and the brain—it does not show up on a traditional X-ray or CT scan. There is no inflammation to see, no tumor to excise and no fracture to set.
This invisibility creates a precarious dynamic in the doctor-patient relationship. When a physician cannot find a “why,” they may inadvertently signal to the patient that the pain isn’t real. This can lead to a cycle of medical gaslighting, where the patient begins to doubt their own physical experience, increasing stress and anxiety, which in turn further sensitizes the nervous system, exacerbating the pain.
The Spectrum of Undiagnosed Pain
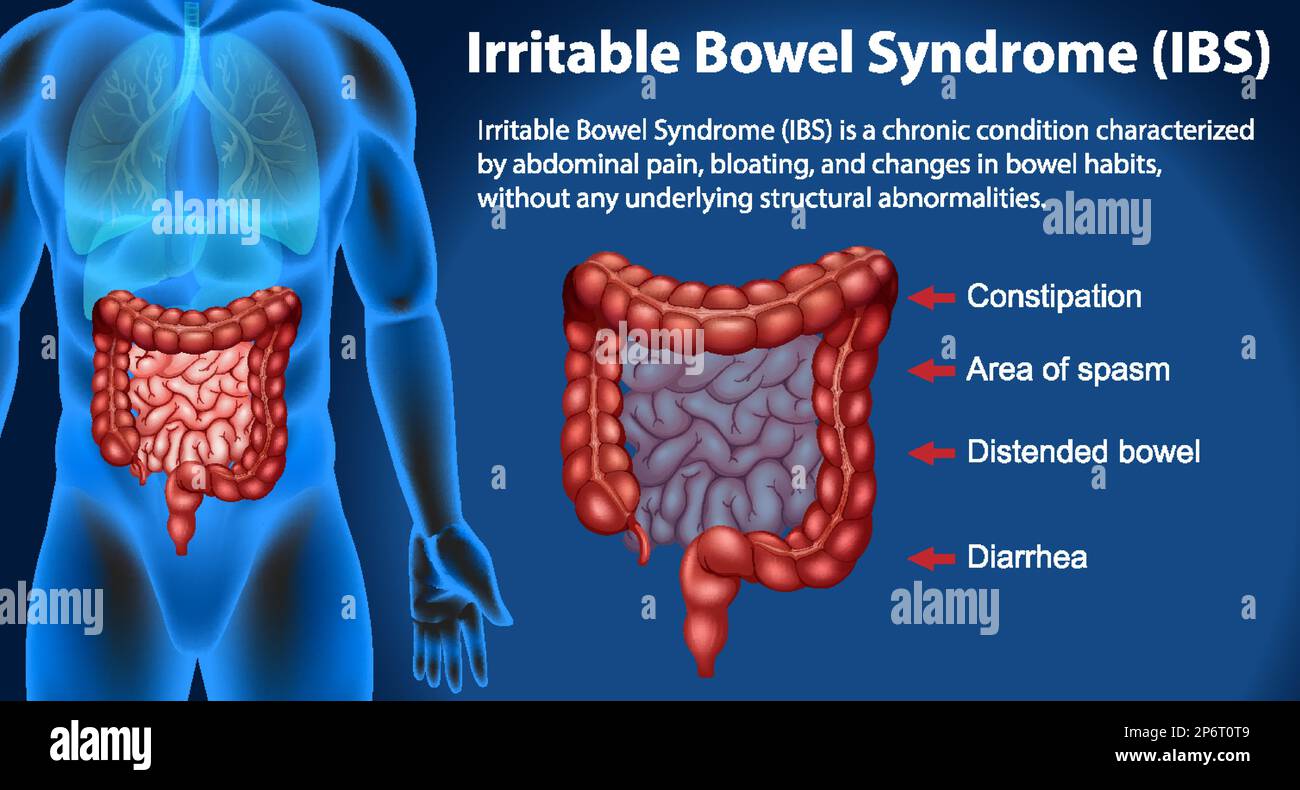
While “pain without diagnosis” is a broad category, it often manifests in specific clinical patterns. Fibromyalgia is perhaps the most well-known example, characterized by widespread musculoskeletal pain, fatigue, and sleep disturbances. Other conditions, such as Irritable Bowel Syndrome (IBS) or certain types of chronic pelvic pain, often follow the same nociplastic pattern where the organ itself is healthy, but the sensory processing is dysfunctional.
The impact on the stakeholder—the patient—is profound. Beyond the physical toll, there is a significant socioeconomic burden. Many individuals find themselves unable to maintain full-time employment, yet they struggle to secure disability benefits because they lack a “verifiable” diagnosis based on imaging. The psychological weight of being “unseen” by the medical establishment often leads to secondary diagnoses of depression and generalized anxiety disorder.
| Pain Type | Primary Cause | Diagnostic Evidence | Example |
|---|---|---|---|
| Nociceptive | Actual or threatened tissue damage | Visible on MRI/X-ray/Physical exam | Acute ankle sprain |
| Neuropathic | Lesion or disease of the somatosensory system | Nerve conduction studies/EMG | Diabetic neuropathy |
| Nociplastic | Altered nociception (sensitization) | Clinical history/Exclusion of others | Fibromyalgia |
Moving Beyond the Search for a ‘Spot’
The shift in treating undiagnosed chronic pain requires moving away from the “search for the spot”—the idea that if we just find the one damaged disc or the one inflamed nerve, People can fix the problem. When pain is nociplastic, the goal of treatment shifts from repair to retraining.
Multimodal therapy is currently the gold standard for managing these conditions. This approach acknowledges that because the pain is a complex interaction of biological, psychological, and social factors, a single pill or surgery is rarely the answer. Effective management typically includes:
- Patient Education: Understanding that “hurt does not always equal harm.” Knowing that the pain is real but not indicative of ongoing tissue damage can lower the brain’s threat response.
- Graded Motor Imagery: Slowly reintroducing movement through a series of steps—from imagining the movement to performing it—to desensitize the nervous system.
- Cognitive Behavioral Therapy (CBT): Not to “cure” the pain, but to manage the emotional distress and catastrophic thinking that can amplify the sensory experience.
- Neuromodulators: Certain medications that target neurotransmitters in the brain and spinal cord to help “turn down the volume” of the pain signals.
The Path Forward in Pain Medicine
The future of diagnosing “invisible” pain lies in the development of biomarkers. Researchers are currently exploring functional MRI (fMRI) and advanced blood protein analysis to identify the chemical signatures of central sensitization. The goal is to move from a diagnosis of exclusion—where we say a patient has nociplastic pain because we found nothing else—to a diagnosis of inclusion, where we can objectively prove the nervous system is in a sensitized state.
Until those tools are widely available, the most powerful tool remains the clinical validation of the patient’s experience. Acknowledging that pain is real, even in the absence of a visible lesion, is often the first step in reducing the patient’s stress response and beginning the process of neurological retraining.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
Medical researchers are currently refining the IASP’s guidelines on nociplastic pain, with updated clinical frameworks expected to be integrated into primary care training over the next two years. This shift aims to reduce the time patients spend in the “undiagnosed” phase of their illness.
Do you or a loved one have experience with chronic pain that defied a traditional diagnosis? We invite you to share your story in the comments or share this article to help others find a vocabulary for their experience.

