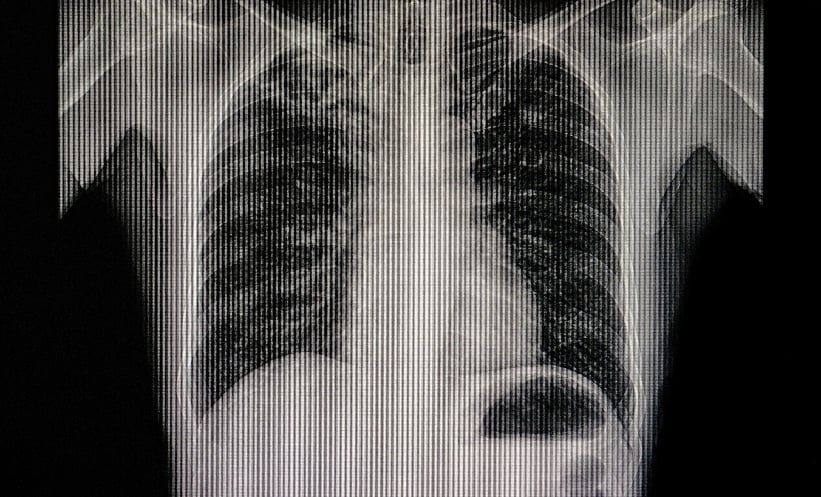
For millions of people living in the world’s most underserved regions, a treatable cough can quickly become a death sentence. Tuberculosis (TB) remains one of the deadliest infectious killers globally, with the World Health Organization reporting that roughly 10.6 million people fell ill with the disease in 2022 alone, resulting in 1.3 million deaths.
The tragedy is not a lack of cure, but a lack of detection. In many low- and middle-income countries (LMICs), the path to diagnosis is blocked by a severe shortage of radiologists and a stark lack of basic medical imaging. This “imaging gap” means that countless cases go undetected until the disease is advanced, fueling community transmission and increasing mortality.
However, a shift toward AI-assisted chest X-rays for TB detection is beginning to bridge this divide. By integrating artificial intelligence with portable imaging, health systems are now able to screen high-risk populations in remote areas, identifying abnormalities with a speed and precision that was previously impossible without a specialist on-site.
As a physician, I have seen how diagnostic delays erode patient trust and worsen clinical outcomes. The promise of AI here is not to replace the doctor, but to act as a sophisticated triage tool—flagging the most urgent cases for confirmatory testing and ensuring that those who are “invisible” to the healthcare system are finally seen.
Closing the Global Imaging Divide
The inequity in diagnostic access is staggering. This proves estimated that approximately 3.21 billion people in LMICs lack access to basic imaging services, meaning nearly two-thirds of the global population is effectively blind to the internal manifestations of disease. Even as high-income nations rely on a dense network of CT and MRI scanners, many regions in the Global South struggle to maintain a single functioning X-ray machine for an entire district.
Chest X-rays have long been the backbone of respiratory screening because they are relatively low-cost and versatile. They can detect not only TB but also pneumonia and lung cancer. The bottleneck, however, has always been the human element: there are simply not enough trained radiologists to read the volume of films generated during mass screening campaigns.
AI changes this equation by automating the initial interpretation. Recent implementation data suggests that AI-assisted interpretation can increase the sensitivity for detecting thoracic abnormalities by up to 26%, while simultaneously reducing the time required to read a scan by nearly a third. This efficiency allows health workers to move through high-risk populations more quickly, prioritizing patients for the gold-standard microbiologically confirmed tests.
The Power of Active Case Finding
One of the most significant hurdles in TB control is the “asymptomatic” patient. A substantial number of people with microbiologically confirmed TB do not present with the classic symptoms—such as a persistent cough or night sweats—until the disease is well-advanced. These individuals continue to spread the bacteria in their communities, unaware they are ill.
AI-enabled workflows facilitate “active case finding,” where screening is brought to the people rather than waiting for patients to visit a clinic. The deployment of ultra-portable X-ray systems is central to this strategy. These devices, which can operate without fixed hospital infrastructure, allow medical teams to reach remote villages and urban slums.
| Feature | Traditional Screening | AI-Assisted Screening |
|---|---|---|
| Detection Method | Symptom-based triage | AI-flagged imaging abnormalities |
| Speed of Result | Days to weeks (radiologist review) | Near-instantaneous triage |
| Reach | Fixed clinic/hospital settings | Portable, community-based outreach |
| Sensitivity | Dependent on clinician experience | Up to 26% increase in abnormality detection |
Beyond TB, these AI tools are proving to be multi-purpose. Automated analysis can identify other critical conditions, such as cardiomegaly (an enlarged heart) and various pulmonary diseases. This represents particularly vital as LMICs face a “double burden” of disease—the simultaneous rise of non-communicable diseases like heart failure alongside persistent infectious threats.
Navigating the Risks of Automation
Despite the clinical potential, the integration of AI into public health is not without risk. Much of the current evidence comes from implementation studies often funded or conducted by the organizations developing the software. This creates a pressing require for independent validation and more robust regulatory frameworks to ensure these tools work across diverse ethnicities and populations.

There are also significant technical and ethical concerns that must be addressed:
- Algorithm Bias: AI trained on datasets from one region may not perform with the same accuracy in another, potentially leading to false negatives in specific populations.
- Over-Reliance: In settings with minimal clinical oversight, there is a danger that practitioners may trust the AI implicitly, overlooking subtle clinical signs that a human eye would catch.
- Infrastructure Fragility: AI requires stable electricity and, often, internet connectivity for cloud-based processing—luxuries that are not guaranteed in the most remote areas.
To be effective, AI must complement clinical expertise, not replace it. The goal is a “human-in-the-loop” system where AI handles the bulk of the triage, and human clinicians focus their limited time on the most complex and high-risk cases.
The Path Toward Integration
For AI-assisted imaging to move from a series of successful pilots to a global standard of care, it must be woven into national digital health strategies. This requires more than just software. it requires investment in the “last mile” of healthcare—clear referral pathways that ensure a patient flagged by an AI scan actually receives the necessary treatment.
If implemented with caution and equity, these tools could fundamentally alter the trajectory of the TB epidemic, moving the world closer to the WHO’s End TB Strategy targets by finding the millions of missing cases that currently evade detection.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
The next critical step for the global health community will be the publication of larger, independent longitudinal studies verifying the long-term impact of AI triage on patient mortality rates in LMICs. These findings will likely dictate the next wave of WHO guidelines for respiratory screening.
Do you suppose AI should be the primary triage tool in underserved regions, or does the risk of bias outweigh the benefit of speed? Let us know in the comments.