A routine screening procedure designed to prevent cancer can occasionally lead to an unexpected and acute surgical emergency. While colonoscopies are generally safe, a rare but critical complication has emerged in clinical literature: the development of appendicitis following the procedure. This phenomenon, often termed “post-colonoscopy appendicitis,” presents a diagnostic challenge because the symptoms can mimic the general discomfort associated with the procedure’s recovery.
The mechanism behind this complication often involves the mechanical stress placed on the cecum and the appendix during the navigation of the colonoscope. When the scope reaches the end of the large intestine, the pressure exerted or the introduction of air and carbon dioxide for insufflation can potentially trigger an obstruction or inflammation of the appendiceal orifice. For patients, identifying the difference between normal post-operative bloating and a surgical emergency is vital for a timely recovery.
As a physician and medical writer, I have seen how “incidental” findings in medicine can often be the most dangerous. In these specific cases, the appendicitis is not a coincidence but a direct, albeit rare, consequence of the clinical intervention. Understanding the timeline of symptom onset and the specific red flags can prevent the progression from a simple inflammation to a life-threatening appendiceal rupture.
The Mechanics of Post-Procedure Inflammation
During a standard colonoscopy, the gastroenterologist must navigate the scope through the entire length of the colon to reach the cecum—the pouch-like beginning of the large intestine where the appendix is attached. To maintain visibility, the physician pumps air or gas into the colon. This process, known as insufflation, expands the bowel walls.

In rare instances, this pressure can cause the appendix to become compressed or can push fecal matter into the appendiceal lumen, leading to an obstruction. Once the appendix is blocked, bacteria multiply rapidly, causing the organ to swell and become infected. Because the patient has recently undergone a procedure that involves gas and mild cramping, the early signs of appendicitis following colonoscopy may be dismissed as “normal” recovery symptoms.
Clinical data suggests that the risk is further compounded if the patient has pre-existing conditions, such as a narrow appendiceal opening or previous abdominal surgeries that have created adhesions. These adhesions can tether the appendix in a way that makes it more susceptible to mechanical trauma during the scope’s maneuvers.
Recognizing the Red Flags
The primary challenge for both patients and clinicians is the “diagnostic mask.” A patient who has just had a colonoscopy is expected to experience some gas, bloating, and mild abdominal discomfort. However, the progression of appendicitis follows a distinct, albeit sometimes subtle, pattern.
Typical post-colonoscopy recovery involves generalized bloating that improves as gas is expelled. In contrast, appendicitis typically manifests as a shift in pain. What begins as a vague feeling of discomfort around the navel often migrates to the lower right quadrant of the abdomen. This “migratory pain” is a classic hallmark of the condition and should be treated as a medical emergency.
Patients and caregivers should be vigilant for the following symptoms following a procedure:
- Localized Pain: Sharp, stabbing pain specifically in the lower right abdomen that worsens with movement or coughing.
- Systemic Response: The development of a low-grade fever or chills, which are not typical of a standard colonoscopy recovery.
- Gastrointestinal Distress: Nausea and vomiting that persist or worsen several hours after the sedation has worn off.
- Rebound Tenderness: Intense pain that occurs when pressure is released from the abdominal wall.
Clinical Diagnosis and Management
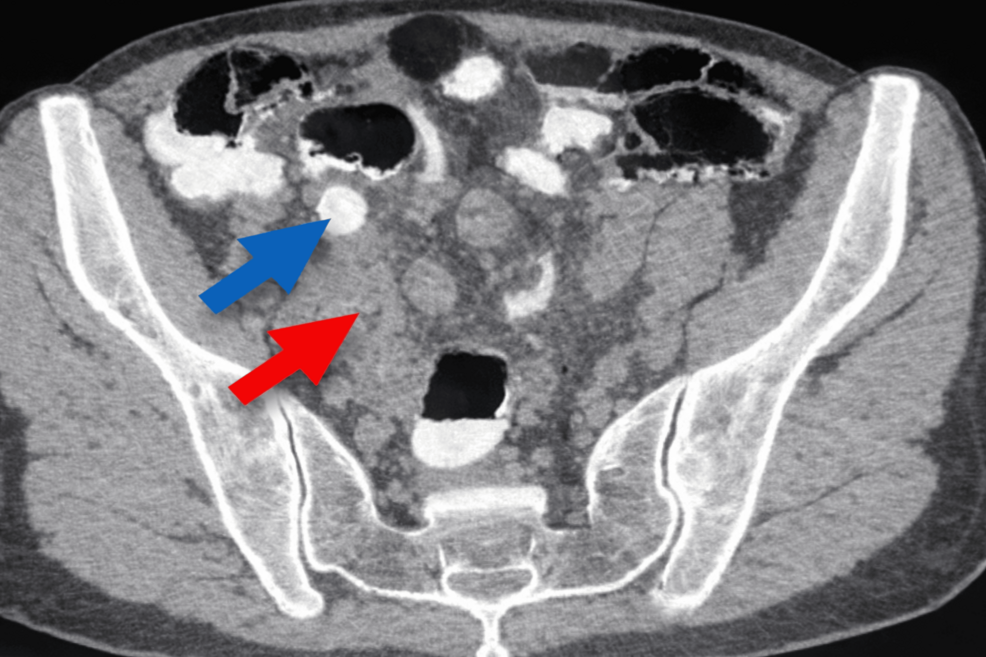
When a patient presents with these symptoms, clinicians must act quickly to avoid perforation. The gold standard for diagnosis remains imaging, specifically Computed Tomography (CT) scans or ultrasound. A CT scan is particularly effective at visualizing the diameter of the appendix and the presence of periappendiceal fat stranding, which indicates active inflammation.
The management of this condition is similar to primary appendicitis, typically involving an appendectomy. Depending on the severity and whether the appendix has already ruptured, surgeons may opt for a laparoscopic approach—which is less invasive and allows for faster recovery—or an open surgery if complications are extensive.
| Symptom | Standard Recovery | Appendicitis Warning |
|---|---|---|
| Pain Location | Generalized/Diffuse bloating | Localized Lower Right Quadrant |
| Pain Progression | Improves as gas is passed | Increases in intensity over hours |
| Temperature | Normal (Afebrile) | Low-grade fever or higher |
| Nausea | Mild, related to sedation | Persistent or worsening vomiting |
The Broader Impact on Patient Safety
This rare complication underscores the importance of the “post-procedure window.” While the risk is low, the impact of a missed diagnosis is high. Medical professionals are encouraged to maintain a high index of suspicion when patients return to the clinic or emergency room with right-sided pain shortly after a bowel scope.
For the general public, the takeaway is not to fear the colonoscopy—which remains the gold standard for colorectal cancer screening—but to be an active participant in their post-operative monitoring. Reporting “atypical” pain immediately can be the difference between a simple laparoscopic procedure and a complex treatment for peritonitis.
Medical guidelines from organizations like the American Society for Gastrointestinal Endoscopy (ASGE) emphasize the require for careful patient education regarding the signs of perforation and inflammation following endoscopic interventions.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
The medical community continues to monitor these rare events to refine the techniques used during cecal intubation. The next step in improving patient outcomes involves the integration of more rigorous post-discharge symptom checklists to aid patients identify early warning signs of complications.
Do you have questions about colonoscopy recovery or have you experienced unexpected symptoms after a procedure? Share your thoughts and experiences in the comments below.