California is preparing for a significant shift in its healthcare landscape as it moves to implement California Medicaid work requirements for millions of residents. The transition, mandated by the 2025 reconciliation law, requires states to condition eligibility for adults in the Affordable Care Act (ACA) Medicaid expansion group on meeting specific work or educational criteria starting January 1, 2027.
The mandate arrives at a precarious moment for the state’s finances. Governor Gavin Newsom projects a $3 billion structural deficit for fiscal year 2027, a gap that is expected to widen to $22 billion by fiscal year 2028. This fiscal strain is compounded by slowing revenue growth and a reduction in federal funding, leaving the state to balance the administrative costs of a massive policy overhaul against a shrinking budget.
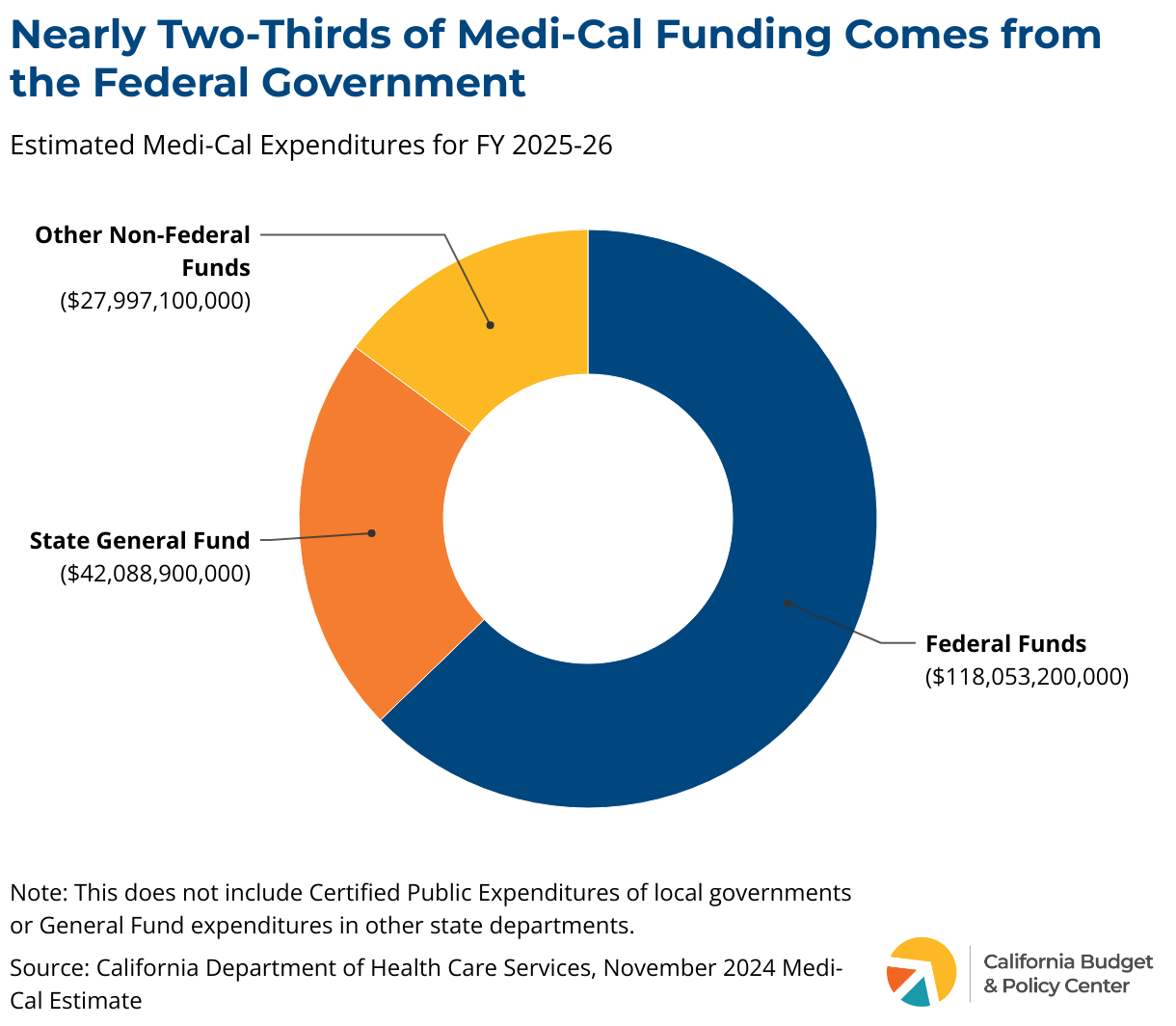
Medi-Cal, the state’s Medicaid program, is a cornerstone of California’s public health infrastructure, providing coverage to 14.8 million enrollees as of June 2025. The program’s scale is immense; under the Governor’s proposed budget, Medicaid accounts for approximately 40% of the total state budget and 20% of General Fund spending in FY 2027, totaling $49 billion.
A Tenuous Fiscal Climate and Immediate Cuts
To manage rising costs and revenue volatility, California has already begun implementing spending cuts. In fiscal year 2026, the state took several steps to slow the growth of Medicaid expenditures, which were driven by higher service utilization per enrollee and recent benefit expansions. These measures included the partial restoration of asset tests for seniors and people with disabilities, the termination of coverage for GLP-1 obesity treatments, and the end of supplemental payments for dental services.
The state has also tightened restrictions on its state-funded health program for immigrant adults. These changes include pausing certain benefits and enrollment, implementing cost-sharing, and reducing payments to health centers for services provided to undocumented immigrants. To mitigate some of the federal funding losses, California allocated funds to replace ACA Marketplace subsidies after the expiration of enhanced premium tax credits at the end of 2025 and received $233 million through the federal Rural Health Transformation Program.
The 2025 reconciliation law is expected to be a primary driver of future deficits. The governor’s budget estimates that this law alone will result in $1.4 billion in General Fund costs for FY 2027, with $1.1 billion of that stemming specifically from Medicaid. In some regions, the financial pressure has reached the local level; voters in one California county approved a tax increase in December 2025 specifically to backfill Medicaid funding gaps caused by the federal changes.
Who Is Affected by the Modern Requirements?
The scope of the work requirements is vast, potentially affecting approximately five million expansion enrollees. However, state data suggests that a majority of this population may already meet the criteria. Analysis indicates that roughly 63% of Medicaid adults without dependent children in California already work 80 or more hours per month or are attending school.
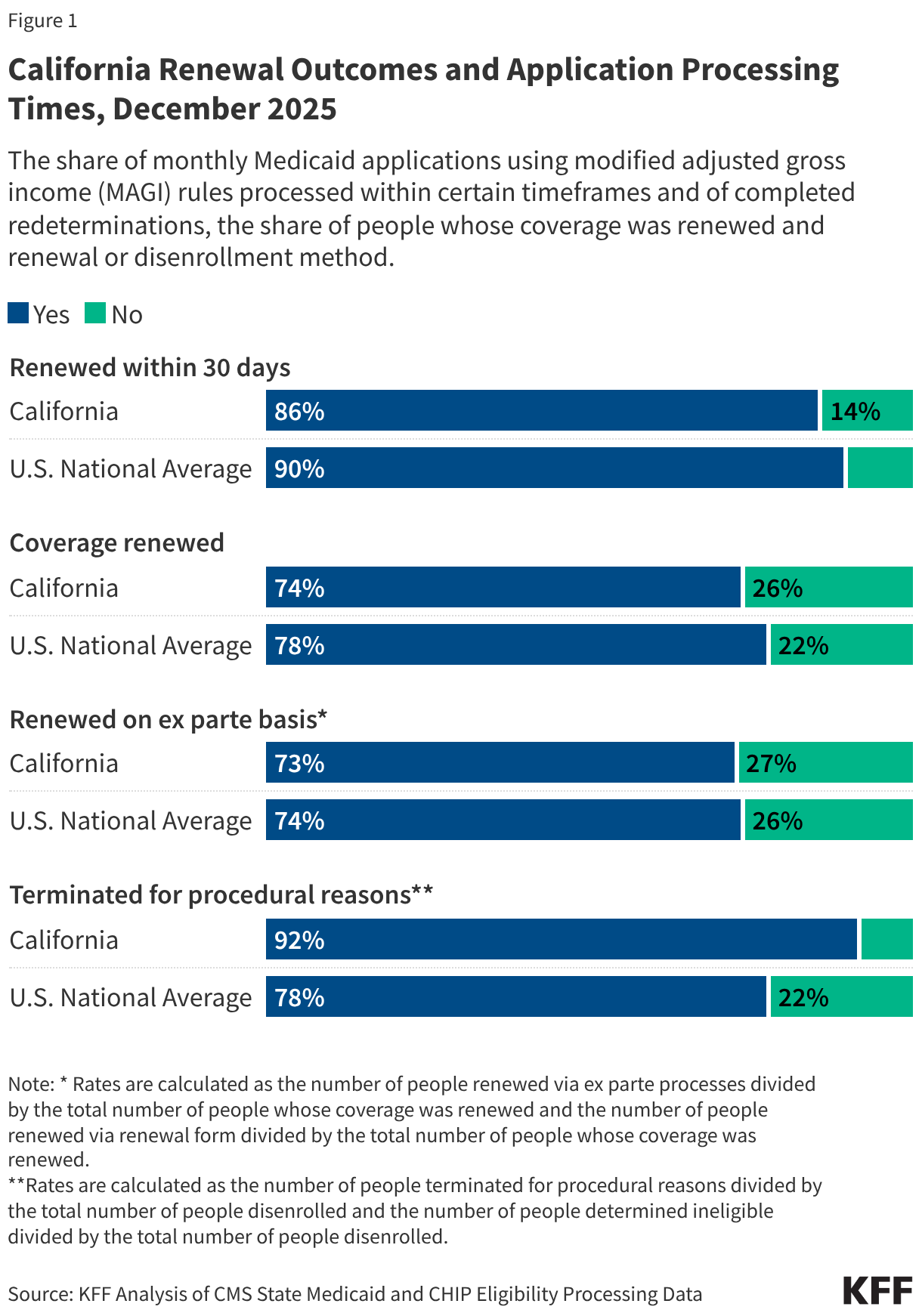
Despite this, the administrative hurdle remains significant. California estimates that the introduction of these requirements could lead to the disenrollment of up to 1.4 million individuals over the implementation period. This risk is heightened by the state’s history of “procedural disenrollments”—people losing coverage not because they are ineligible, but because of paperwork errors or missed deadlines. As of December 2025, 92% of those disenrolled in California were terminated for procedural reasons, a rate significantly higher than the national average of 78%.
The Roadmap for Implementation and Outreach
The state is currently developing the technical and communicative infrastructure needed to execute these changes. Initial guidance from the Department of Health Care Services (DHCS) outlines the use of data matching and look-back periods to verify compliance. To prevent immediate losses of coverage, the state plans to verify work requirements at the next renewal for individuals transitioning into the ACA expansion group, rather than requiring immediate proof.
To support this transition, the Governor’s budget includes $4 million for navigators to assist residents with eligibility and retention. The state’s outreach strategy includes several key components:
- Multilingual Communication: Materials will be translated into 19 languages to reach California’s diverse population.
- Trusted Messengers: The state will partner with local community groups and clinics to spread awareness.
- Digital Outreach: Use of text messages, social media, and flyers to notify members at least three months before the first compliance period.
- Automation: An effort to use existing data sources to minimize the manual paperwork required from enrollees.
The state’s ability to automate this process is critical. Early estimates suggest that roughly 1.8 million individuals could be determined exempt or compliant through automated data matching based on August 2025 data. However, the state acknowledges that the “ex parte” renewal rate—where the state verifies eligibility without requiring a form from the user—has dropped since the end of the COVID-era continuous enrollment guarantees, which may increase the manual administrative burden.
What Remains Uncertain
While the framework is taking shape, several critical definitions remain pending. California is currently awaiting federal guidance to clarify the standards for “medically frail” exemptions, the acceptable forms of verification, and the specific criteria for what constitutes a qualifying work activity. Until these definitions are finalized, the state cannot fully determine how many residents will qualify for exemptions.
Disclaimer: This article is provided for informational purposes only and does not constitute legal or financial advice regarding Medicaid eligibility or state budget law.
The next critical phase will involve the refinement of the state’s data-matching systems and the rollout of the comprehensive outreach campaign as the January 2027 deadline approaches. State officials have indicated they will continue to monitor key metrics, including the number of procedural disenrollments, to assess the impact of these requirements in real-time.
We invite readers to share their perspectives on these policy changes in the comments below or share this story with others affected by these updates.