The delicate balance of the U.S. Public health infrastructure is facing a critical juncture as new data suggests a precarious link between federal funding and the trajectory of the HIV epidemic. A recent analysis indicates that HIV infections could rise 10% if the Centers for Disease Control and Prevention (CDC) ceases its funding for HIV testing provided to local health departments and community organizations.
For decades, the strategy to curb the spread of the virus has relied on a simple but effective clinical loop: early diagnosis followed by immediate initiation of antiretroviral therapy (ART). When a person knows their status and begins treatment, the amount of virus in their blood can drop to undetectable levels—a state known as undetectable = untransmittable (U=U)—effectively stopping the chain of transmission to others.
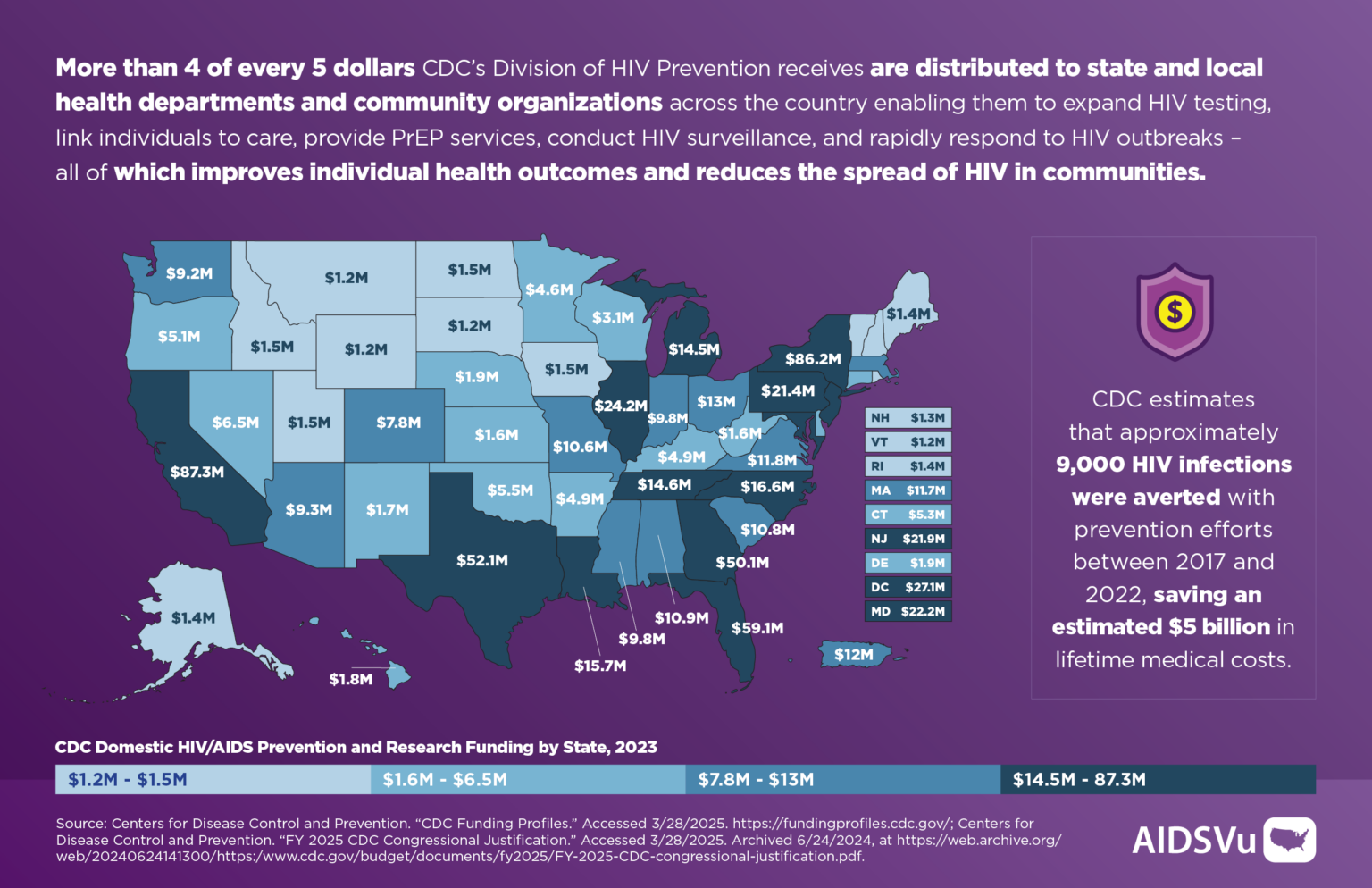
The CDC’s funding serves as the primary engine for this process, financing the tests that identify undiagnosed individuals and the community outreach programs that bring marginalized populations into the healthcare system. Without this financial backbone, the gap between infection and diagnosis is expected to widen, leading to a measurable increase in new transmissions across the country.
As a physician, I have seen how the “testing-to-treatment” pipeline functions on the ground. It is not merely about the cost of a test kit; it is about the infrastructure of trust, and accessibility. When federal funds vanish, the community clinics that serve as the first point of contact for high-risk populations often have no choice but to scale back their services, leaving thousands of people unaware of their status.
The Mathematical Risk of Funding Gaps
The prediction that infections would climb by 10% is not an arbitrary figure but a reflection of how testing prevents secondary infections. When individuals remain undiagnosed, they are more likely to unknowingly transmit the virus to partners. Conversely, timely diagnosis allows for the immediate deployment of PrEP (pre-exposure prophylaxis) for partners and ART for the patient, both of which are cornerstone tools in the modern public health arsenal.
The impact of these funding cuts would not be felt uniformly across the population. Historically, disparities in HIV prevalence and access to care have disproportionately affected Black and Hispanic/Latino communities, as well as LGBTQ+ individuals. A reduction in CDC-funded community testing often hits these “hot spots” first, as these programs are specifically designed to reach people who may not have traditional health insurance or a primary care provider.
The following table outlines the core components of the CDC-funded testing ecosystem and the projected risks associated with their removal:
| Program Component | Primary Function | Risk if Funding Ends |
|---|---|---|
| Local Health Depts | Broad-scale screening & surveillance | Delayed detection of local outbreaks |
| Community Orgs | Hard-to-reach population outreach | Increased undiagnosed rates in marginalized groups |
| Testing Infrastructure | Provision of rapid test kits | Reduced availability of free/low-cost screening |
| Linkage to Care | Connecting positive patients to ART | Higher transmission rates due to treatment gaps |
The Clinical Ripple Effect: From Diagnosis to Transmission
The danger of ending these funds lies in the “silent” period of HIV infection. Many individuals live with the virus for years without presenting obvious symptoms, during which time they can still transmit the virus. The CDC’s role in funding testing is designed to shorten this window of ignorance.

When testing funds are cut, the “cascade of care”—the sequence of steps from diagnosis to viral suppression—breaks at the very first link. If a person is not tested, they cannot be linked to care; if they are not linked to care, they cannot achieve viral suppression; and if they are not suppressed, the risk of new infections continues to grow.
Public health experts emphasize that funding testing is a high-yield investment. The cost of providing a test is negligible compared to the lifelong cost of treating a new HIV infection and the broader societal cost of an expanding epidemic. By preventing a 10% increase in new cases, the federal government avoids millions of dollars in future healthcare expenditures.
Who is Most at Risk?
The vulnerability to these funding cuts is highest among those who rely on “low-barrier” testing. This includes individuals experiencing homelessness, those in rural areas with limited clinic access, and people who face systemic barriers to healthcare. Community-based organizations often provide “mobile testing” or “peer-led” initiatives that the CDC funds, which are far more effective at reaching these populations than traditional hospital-based models.
The loss of these funds would likely result in a shift toward “symptomatic testing,” where patients only seek help once they are already ill. By that stage, the window for preventing transmission has already closed, and the patient’s own health is significantly more compromised, requiring more intensive and expensive medical intervention.
The Path Forward and Systemic Constraints
While the prediction of a 10% rise in infections serves as a warning, it similarly highlights the systemic fragility of the U.S. Public health model. Relying on discretionary federal grants for essential diagnostic services creates a cycle of instability for the non-profits and local health departments that execute the work.
To mitigate these risks, advocates suggest a shift toward more sustainable, permanent funding structures that are not subject to annual budget fluctuations. Integration of HIV testing into routine primary care is another goal, but this requires a level of provider education and reimbursement stability that currently does not exist in many parts of the country.
the rise of home-testing kits has provided some relief, but these are not a replacement for the comprehensive “test and link” services provided by CDC-funded organizations. A home test only works if the person has the means to follow up with a clinic for a confirmatory test and immediate treatment—a process that still relies heavily on the infrastructure the CDC supports.
Disclaimer: This article is provided for informational purposes only and does not constitute medical advice. Please consult a healthcare provider for personal medical concerns or testing.
The next critical checkpoint for these funding levels will be the upcoming federal budget appropriations process, where the allocation for the CDC’s HIV programs will be debated and decided. The outcome of these legislative sessions will determine whether the predicted rise in infections becomes a reality or if the current trajectory toward ending the epidemic can be maintained.
We want to hear from you. How has access to testing changed in your community? Share your thoughts in the comments below or share this article to spread awareness.