The landscape of cancer prevention is undergoing a subtle but significant shift, moving beyond lifestyle modifications and screenings toward the potential of preventive vaccines—not to *treat* cancer, but to stop it from developing in the first place, particularly in individuals with known hereditary predispositions. While still largely in the research phase, this emerging field offers a beacon of hope for those carrying genetic mutations that dramatically increase their risk of developing certain cancers. Understanding the potential of these vaccines and the challenges that lie ahead, is crucial for both patients and healthcare providers.
For decades, genetic testing has allowed individuals to identify inherited mutations in genes like BRCA1 and BRCA2, which are strongly linked to increased risks of breast, ovarian, and other cancers. Current management strategies typically involve increased surveillance—more frequent screenings—or, in some cases, prophylactic surgery to remove at-risk tissues. However, these approaches aren’t without drawbacks. Frequent screenings can lead to anxiety and false positives, while surgery carries its own risks and impacts quality of life. Preventive vaccines represent a potentially less invasive and more targeted approach to mitigating these risks. This emerging area of hereditary cancer syndromes is gaining momentum as research progresses.
How Preventive Cancer Vaccines Work
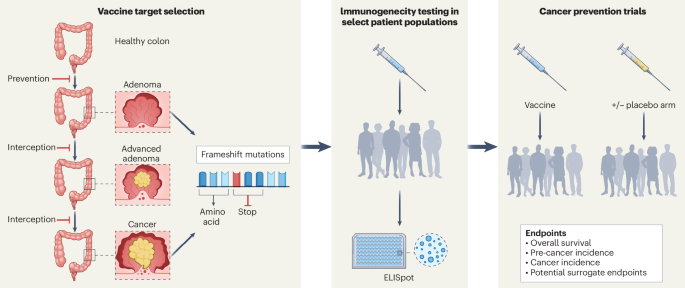
Unlike traditional vaccines that introduce weakened or inactive pathogens to stimulate an immune response, these preventive cancer vaccines aim to train the immune system to recognize and destroy cells *before* they become cancerous. The approach often centers on targeting specific proteins, or neoantigens, that are produced by cells carrying cancer-predisposing mutations. These neoantigens are essentially “flags” that mark cells as abnormal, allowing the immune system to identify and eliminate them.
Researchers are exploring several different vaccine platforms, including mRNA vaccines—the same technology used in some COVID-19 vaccines—and peptide vaccines. MRNA vaccines deliver genetic instructions to cells, prompting them to produce the neoantigen and trigger an immune response. Peptide vaccines, directly deliver fragments of the neoantigen to the immune system. The goal in both cases is to create a robust and long-lasting immune response that can prevent the development of cancer.
Loxo Oncology and Lilly’s Role in Advancing Cancer Research
The acquisition of Loxo Oncology by Eli Lilly in 2019 for approximately $8.0 billion underscores the pharmaceutical industry’s growing investment in targeted cancer therapies. While the initial focus of this acquisition was on RET inhibitor selpercatinib, which recently cleared a pivotal trial according to Pharmaphorum, the broader implications extend to the development of innovative cancer prevention strategies. Lilly’s resources and expertise are now being leveraged to explore new avenues in cancer research, including the potential of preventive vaccines.
Current Research and Clinical Trials
While still early days, several clinical trials are underway investigating the feasibility and safety of preventive cancer vaccines. Many of these trials are focused on individuals with Li-Fraumeni syndrome, a rare hereditary disorder caused by mutations in the TP53 gene, which significantly increases the risk of developing a wide range of cancers. Researchers are likewise exploring vaccines for individuals with mutations in BRCA1/2 and other cancer-predisposing genes.
Early results from these trials have been encouraging, demonstrating that these vaccines can elicit a robust immune response and, in some cases, show evidence of targeting pre-cancerous cells. However, it’s important to note that these trials are still ongoing, and more research is needed to determine the long-term efficacy and safety of these vaccines. The challenges include identifying the most effective neoantigens, optimizing vaccine delivery methods, and ensuring that the immune response is sustained over time.
Challenges and Future Directions
Developing effective preventive cancer vaccines is not without its hurdles. One major challenge is the heterogeneity of cancer. Even within individuals with the same genetic mutation, the specific neoantigens that are expressed can vary, making it difficult to design a “one-size-fits-all” vaccine. Personalized vaccine approaches, tailored to the individual’s specific genetic profile and neoantigen expression, may be necessary, but this adds complexity and cost.
Another challenge is the potential for immune evasion. Cancer cells can develop mechanisms to suppress the immune system, making it harder for vaccines to effectively target and destroy them. Researchers are exploring strategies to overcome immune evasion, such as combining vaccines with other immunotherapies. Identifying individuals who would benefit most from these vaccines—those at the highest risk of developing cancer—is crucial for maximizing their impact.
Looking ahead, the field of preventive cancer vaccines holds immense promise. As our understanding of cancer genetics and immunology continues to grow, we can expect to see more sophisticated and effective vaccines emerge. The ultimate goal is to transform cancer from a disease that is often detected at a late stage to one that can be prevented altogether, offering a new era of hope for individuals at high risk.
Disclaimer: This article is for informational purposes only and should not be considered medical advice. Please consult with a qualified healthcare professional for any health concerns or before making any decisions related to your health or treatment.
What are your thoughts on the potential of preventive cancer vaccines? Share your comments below, and please share this article with anyone who might find it helpful.