COVID-19 Significantly Raises Risk of Post-Stroke Complications, New Study Finds
A new observational study reveals that patients with acute ischemic stroke (AIS) and a concurrent COVID-19 infection are significantly more prone to experiencing early neurological deterioration (END), particularly those with pre-existing conditions like diabetes and a higher initial stroke severity.
The research, conducted at a comprehensive tertiary hospital in Zunyi, Guizhou, China, enrolled 83 patients, with 22 ultimately developing END. The findings underscore the complex interplay between COVID-19 and cerebrovascular health, highlighting a heightened risk for those already vulnerable to stroke.
COVID-19 and the Rising Threat of Stroke Complications
Since its emergence in 2019, COVID-19 has been established as a global health crisis by the World Health Organization, impacting not only the respiratory system but also multiple organs, including the brain. While the overall prevalence of AIS appeared to decrease during the pandemic – potentially due to reduced healthcare seeking for mild symptoms or masking of stroke symptoms by COVID-19 – the study confirms that when stroke does occur in conjunction with COVID-19, the outcomes are often more severe.
“Data from clinical research has demonstrated that, compared with IS without COVID-19, IS patients with COVID-19 have more severe symptoms, worse functional prognosis, and a higher risk of death,” researchers noted.
The Role of Inflammation and Coagulation
The study points to a cascade of biological events triggered by COVID-19 that contribute to the increased risk of END. Ischemic stroke is fundamentally linked to thrombotic events, and COVID-19 is known to promote arteriovenous thromboembolism alongside a surge in proinflammatory cytokines. This “cytokine storm” activates endothelial cells and monocytes, leading to the formation of blood clots and disruption of the coagulation system.
Furthermore, the activation of the renin-angiotensin axis leads to an accumulation of angiotensin 2 (ACER2), inducing cerebrovascular constriction, oxidative stress, and breakdown of the blood-brain barrier. The combination of the SARS-CoV-2 virus and cerebrovascular ACER2 exacerbates the inflammatory response, resulting in significant brain tissue damage.
As one researcher explained, “when coagulation dysfunction occurs, SARS-CoV-2 virus aggravate vascular endothelial damage under the chemotactic storm of cytokine inflammation, resulting in the production of a large number of inflammatory factors…leading to acute inflammatory response of cerebral vessels.”
Key Risk Factors Identified in the Study
Researchers identified several key factors that correlated with an increased risk of END in AIS patients with COVID-19:
- Prior diabetes: Patients with a history of diabetes were more susceptible to END.
- Prior stroke: A previous stroke also increased the likelihood of END.
- High baseline NIHSS score: Patients admitted with higher scores on the National Institutes of Health Stroke Scale (NIHSS) – indicating greater stroke severity – were more likely to experience END.
- Abnormal ECG: An abnormal electrocardiogram (ECG) was more frequently observed in patients who developed END.
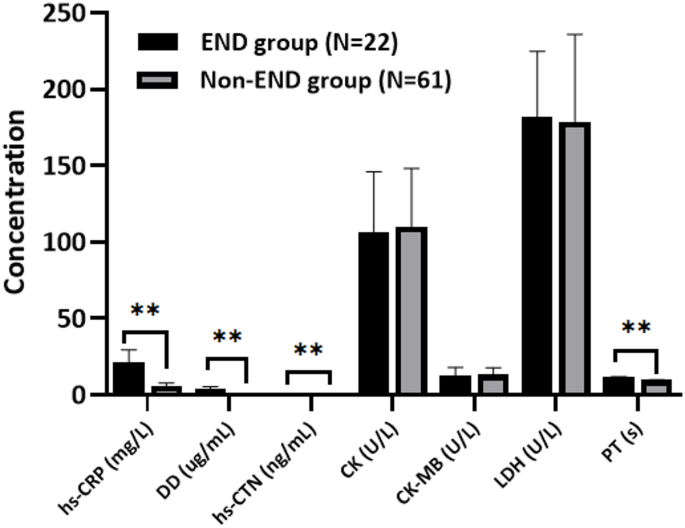
- Prolonged serum PT value: An extended prothrombin time (PT), a measure of blood clotting time, was associated with END.
- Elevated hs-CRP and DD levels: Significantly increased levels of high-sensitivity C-reactive protein (hs-CRP) and D-dimer (DD) – markers of inflammation and blood clot formation, respectively – were also strong predictors of END.
The study also noted that patients experiencing END had a significantly higher proportion of hs-cTn (high-sensitivity cardiac troponin) increases, suggesting potential heart injury. However, researchers cautioned that the relatively small sample size may have influenced this finding.
Thrombolysis and the Timing of Treatment
Of the 83 patients studied, 12 received intravenous thrombolysis, a common treatment for acute ischemic stroke. Five in the END group and seven in the non-END group underwent the procedure, with all experiencing early neurological deterioration. Researchers believe this deterioration may be linked to the abnormal clotting function induced by the combination of COVID-19 and the treatment itself.
“We analyzed that the possible reason is related to the relatively long time from the onset of the disease to the visit of the patient,” researchers stated, noting that delays in administering thrombolysis have been previously linked to poorer outcomes.
Limitations and Future Research
The researchers acknowledged several limitations to their study. The single-center design may introduce selection bias, and strict regional isolation policies during the COVID-19 outbreak hindered the collection of a larger, multi-center dataset. Additionally, the retrospective nature of the study limits the ability to observe detailed patient conditions throughout their illness.
Despite these limitations, the study provides valuable real-world data that can inform future research. “Despite these limitations, all our data are derived from real-world registration data of clinical patients,” the researchers concluded. “These research materials can provide important clinical reference value and further facilitate the conduct of multi-center, large-sample randomized controlled studies.” Further investigation is needed to fully understand the mechanisms driving the increased risk of END in AIS patients with COVID-19 and to develop targeted strategies for prevention and treatment.