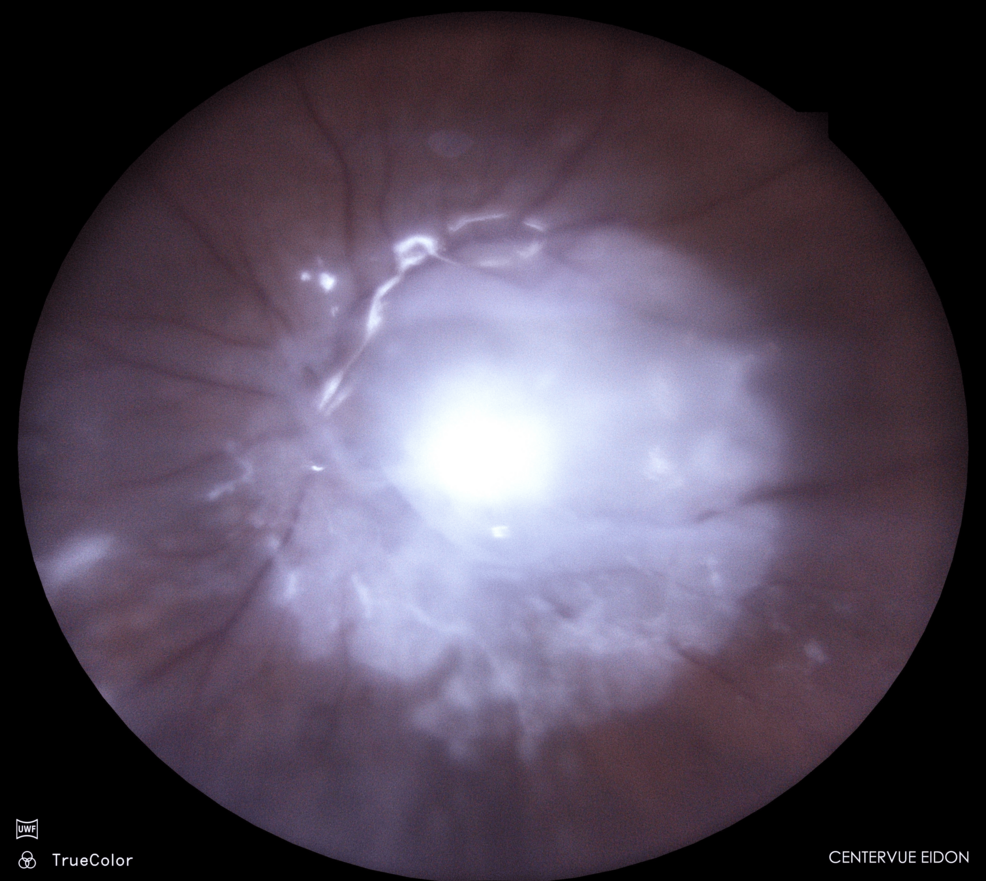
Early Vitrectomy Protocol Shows Promise in Combating Vision-Threatening Endophthalmitis
Table of Contents
A groundbreaking surgical protocol, the Complete Early Vitrectomy for Endophthalmitis (CEVE) protocol, is demonstrating significant potential in improving outcomes for patients suffering from endophthalmitis, a severe inflammation of the eye often leading to vision loss. The protocol emphasizes rapid diagnosis and aggressive surgical intervention, offering a new standard of care for this devastating condition.
The rising incidence of endophthalmitis, particularly following intravitreal injections, has prompted a critical need for refined treatment strategies. Traditionally, treatment involved intravitreal antibiotics, but emerging evidence suggests that early surgical intervention can dramatically improve visual outcomes.
The CEVE Protocol: A Proactive Approach
The CEVE protocol, detailed in a recent report, centers around a swift and complete approach to managing endophthalmitis. It outlines a standardized process encompassing immediate diagnosis, broad-spectrum antibiotics, and, crucially, early vitrectomy – a surgical procedure to remove the vitreous gel from the eye.
According to the report, the key components of the CEVE protocol include:
- Immediate and thorough clinical examination.
- Prompt vitreous aspiration and culture to identify the causative organism.
- Intravitreal injection of broad-spectrum antibiotics, including vancomycin and ceftazidime.
- Pars plana vitrectomy, ideally performed within 24-48 hours of diagnosis.
- Postoperative antibiotic therapy tailored to culture results.
“The speed of intervention is paramount,” stated a senior ophthalmologist involved in developing the protocol. “Delaying vitrectomy can lead to increased inflammation, retinal damage, and ultimately, poorer visual outcomes.”
Surgical Prophylaxis: Preventing Infection
Beyond treatment, the report emphasizes the importance of stringent surgical prophylaxis to minimize the risk of endophthalmitis in the first place. This includes meticulous sterile technique during all intravitreal procedures, including injections and surgeries.
Specific recommendations for surgical prophylaxis include:
- Use of povidone-iodine for periocular skin readiness.
- Draping the face to create a sterile field.
- Strict adherence to aseptic technique during the procedure.
- Consideration of prophylactic antibiotics, even though the optimal regimen remains a subject of ongoing research.
Addressing the Rise in Post-Injection Endophthalmitis
The increasing use of intravitreal injections – a common treatment for conditions like age-related macular degeneration and diabetic retinopathy – has been linked to a rise in post-injection endophthalmitis cases. This has spurred research into preventative measures and optimized treatment protocols.
One analyst noted, “The sheer volume of intravitreal injections being administered necessitates a heightened focus on infection control and rapid response protocols. The CEVE protocol directly addresses this growing concern.”
Visual Outcomes and Future Directions
Early data suggests that the CEVE protocol is associated with improved visual outcomes compared to traditional treatment approaches. Patients undergoing early vitrectomy demonstrate a higher rate of visual acuity recovery and a lower risk of severe vision loss.
Though, further research is needed to validate these findings in larger, multi-center clinical trials. Future studies will focus on refining the protocol,identifying optimal antibiotic regimens,and exploring the potential role of adjunctive therapies.
The CEVE protocol represents a significant advancement in the management of endophthalmitis, offering hope for improved vision and quality of life for patients facing this challenging condition. Continued vigilance in surgical prophylaxis and rapid implementation of the CEVE protocol are crucial steps in combating this sight-threatening disease.