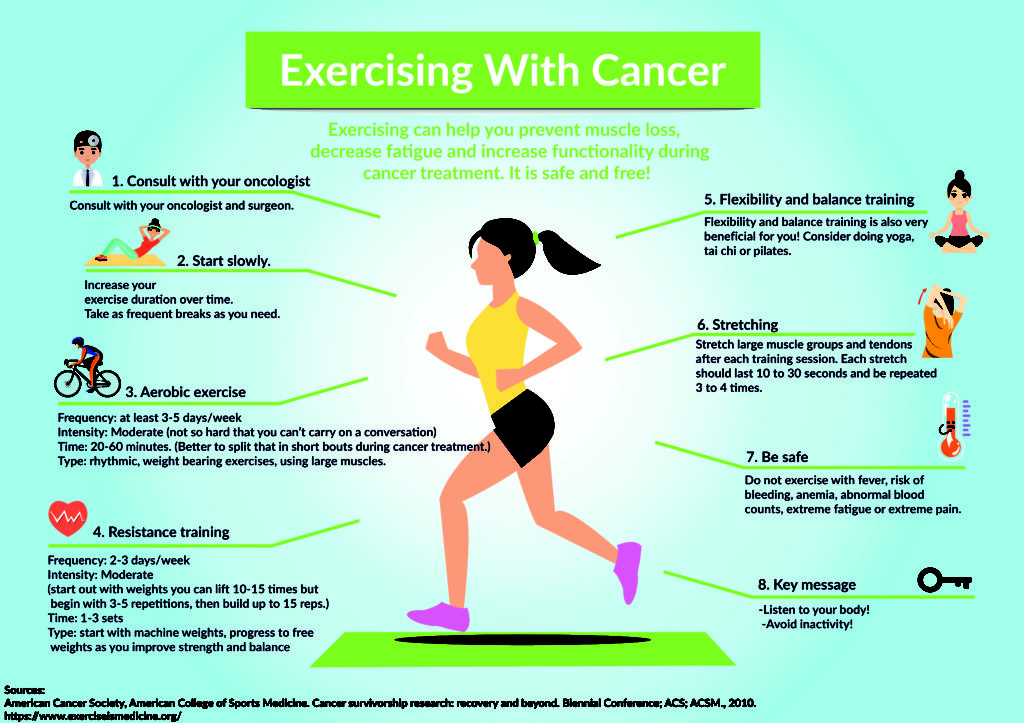
For many, the idea of a “cure” for cancer involves a breakthrough drug or a precise surgical intervention. Still, medical evidence increasingly suggests that one of the most potent tools for lowering cancer risk and improving survival outcomes is already available to nearly everyone: physical activity. From the perspective of clinical oncology, exercise is not merely a lifestyle suggestion but a critical component of preventative and rehabilitative medicine.
The relationship between movement and malignancy is rooted in the body’s systemic response to exertion. Regular physical activity helps regulate insulin levels, reduces chronic inflammation, and modulates hormone levels—all of which are known drivers of cellular mutation. By integrating consistent movement into a daily routine, individuals can significantly lower their risk of developing several types of the disease, including breast and colorectal cancers.
As a board-certified physician and medical writer, I have seen how translating complex research into practical health advice can change a patient’s trajectory. The shift toward “exercise oncology” represents a move away from the traditional “rest and recover” model, recognizing that the body is often more resilient and capable of healing when This proves kept active, even during the rigors of chemotherapy or radiation.
The Biological Mechanics of Risk Reduction
The impact of exercise on cancer risk is not accidental; it is a result of specific biological shifts. Physical activity influences the immune system by increasing the circulation of natural killer cells and T-cells, which are the body’s primary defense against aberrant cells. Exercise helps maintain a healthy weight and improves metabolic health, reducing the likelihood of obesity-related cancers.
Beyond weight management, exercise directly affects the endocrine system. For instance, regular activity can lower the levels of circulating estrogen and insulin-like growth factor (IGF-1), both of which can stimulate the growth of certain tumors. This makes physical activity a primary preventative strategy, particularly for those with a genetic predisposition to hormone-driven cancers.
For those already in treatment, the goals shift from prevention to mitigation. The phenomenon of cancer-related fatigue (CRF) is one of the most debilitating side effects of treatment, often leading patients to grow sedentary, which in turn exacerbates the fatigue. Breaking this cycle is essential for recovery.
Combating Treatment-Induced Fatigue
It may seem counterintuitive to suggest exercise to a patient experiencing profound exhaustion, but clinical data supports the efficacy of low-impact movement. Walking, in particular, has been identified as a highly effective way to reduce cancer-related fatigue. Unlike total rest, which can lead to muscle atrophy and increased lethargy, light aerobic activity stimulates blood flow and boosts mood-regulating endorphins.
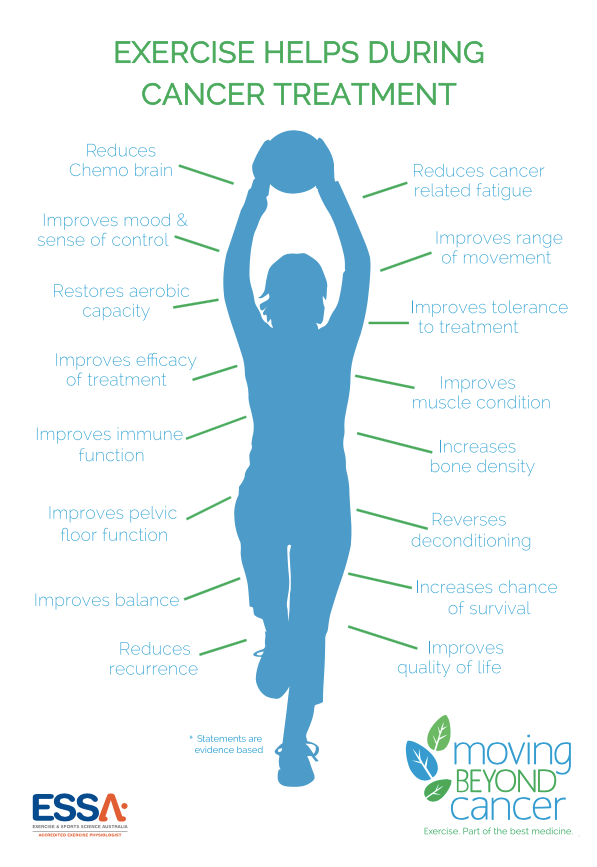
The American Cancer Society emphasizes that walking can help patients regain a sense of control over their bodies and improve their overall quality of life during and after treatment. The key is a gradual approach—starting with short, manageable distances and increasing intensity only as tolerated by the patient and approved by their medical team.
From Recovery to Recurrence Prevention
The benefits of exercise extend far beyond the immediate recovery phase. Emerging programs are now focusing on “exercise as medicine” to reduce the risk of cancer recurrence. By improving cardiovascular health and strengthening the immune system, survivors can create an internal environment that is less hospitable to returning cancer cells.
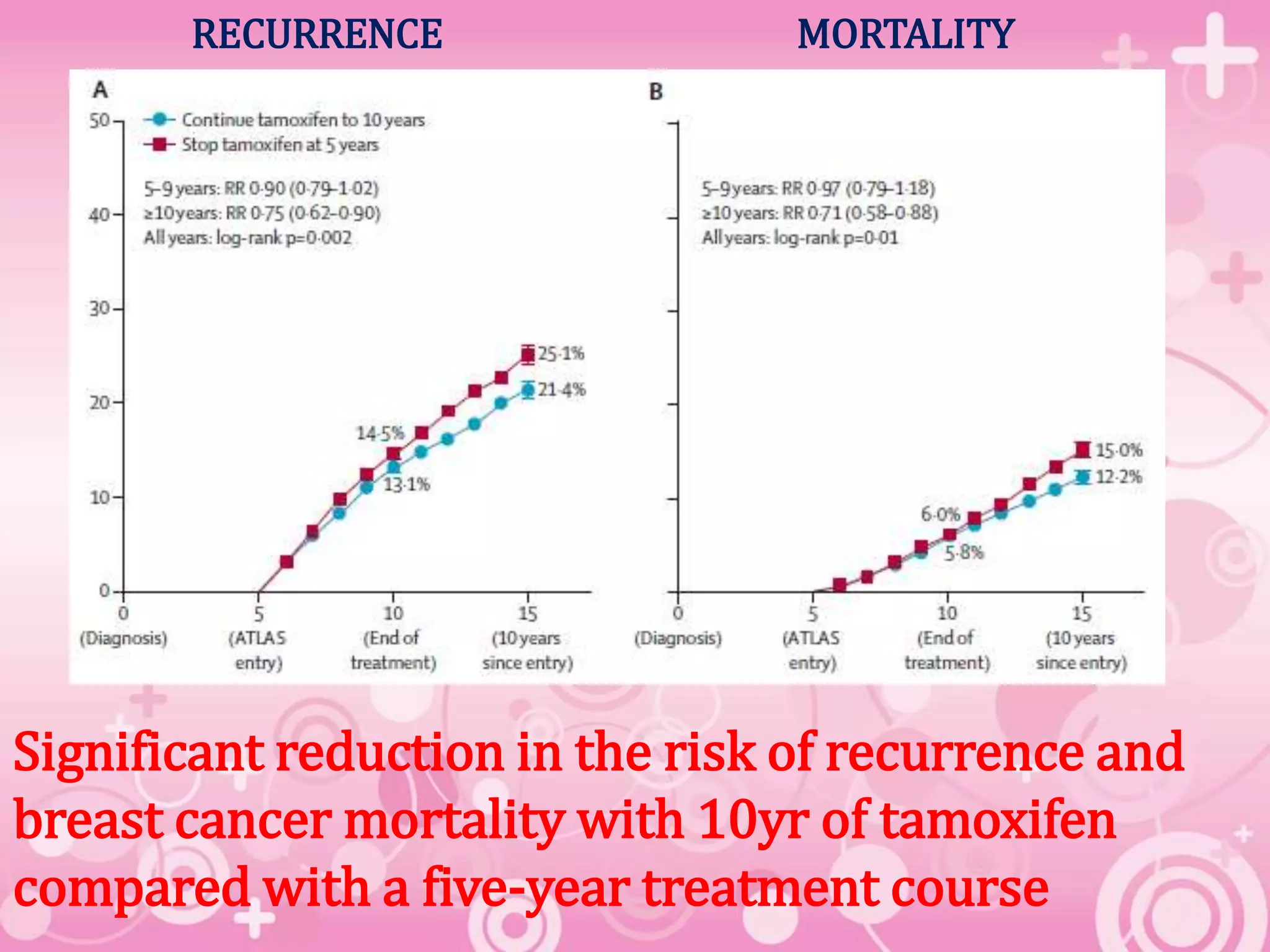
In South Florida, specialized programs have been implemented to help cancer patients recover their strength and lower the risk of recurrence through structured exercise. These programs often combine strength training with aerobic activity, tailored to the specific physical limitations caused by different types of treatment, such as lymphedema or neuropathy.
The transition from a patient to a survivor involves more than just the absence of disease; it involves the restoration of function. Strength training, in particular, helps combat the muscle loss (sarcopenia) often associated with chemotherapy, which is critical for maintaining independence and long-term health.
| Stage | Primary Goal | Recommended Activity | Key Biological Benefit |
|---|---|---|---|
| Prevention | Risk Reduction | 150+ min moderate aerobic/week | Hormonal & Insulin Regulation |
| Active Treatment | Symptom Management | Walking, Gentle Stretching | Reduction of Cancer-Related Fatigue |
| Survivorship | Recurrence Prevention | Strength Training & Aerobics | Immune Support & Muscle Recovery |
Practical Implementation and Safety
While the recommendation to exercise is broad, the application must be individualized. Not every patient can jump into a gym routine. The “dose” of exercise depends on the patient’s current health status, the type of cancer, and the specific side effects of their treatment.
For those starting a regimen, the following steps are generally recommended by health professionals:
- Consult the Oncology Team: Ensure Notice no contraindications, such as unstable blood pressure or severe anemia.
- Start Low and Gradual: Begin with 5–10 minute walks and gradually increase duration.
- Monitor Intensity: Employ the “talk test”—Consider be able to carry on a conversation, but be slightly breathless.
- Prioritize Consistency over Intensity: Frequent, light activity is often more beneficial for fatigue management than sporadic, intense workouts.
The psychological impact of movement is equally significant. Exercise provides a mental reprieve from the “patient identity,” offering a sense of agency and accomplishment that is often stripped away during a diagnosis. This mental fortitude is a critical component of the overall healing process.
Disclaimer: This information is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition or treatment plan.
As research continues to evolve, the integration of physical activity into standard oncological care is expected to become more formalized. The next step for public health officials and medical providers is the wider implementation of supervised exercise programs within hospitals, ensuring that movement is prescribed with the same precision as medication. For those seeking further guidance, the National Cancer Institute provides updated guidelines on physical activity for cancer survivors.
We invite you to share your experiences with exercise during recovery or ask questions about implementing these strategies in the comments below.