For decades, the prevailing medical and social narrative surrounding obesity focused heavily on willpower, caloric restriction, and rigorous exercise. However, the rise of a new class of medications known as GLP-1 receptor agonists for weight loss has fundamentally shifted that conversation, moving the focus from behavioral failure to biological regulation.
These medications, including semaglutide—marketed as Ozempic for type 2 diabetes and Wegovy for chronic weight management—and tirzepatide, sold as Mounjaro and Zepbound, are not merely “diet pills.” They are sophisticated hormonal mimics that target the endocrine system to regulate appetite and blood sugar, offering clinical results that were previously only achievable through bariatric surgery.
As a physician, I have watched these drugs transition from specialized diabetes treatments to cultural phenomena. While the rapid weight loss is often the headline, the clinical reality is more complex, involving a delicate balance of metabolic benefits, significant gastrointestinal challenges, and a necessary rethinking of how we treat obesity as a chronic, lifelong disease.
The Biology of Satiety: How GLP-1s Work
To understand why these drugs are so effective, one must understand the glucagon-like peptide-1 (GLP-1) hormone. Naturally produced in the gut, GLP-1 is released after eating to signal the pancreas to secrete insulin and the liver to stop producing glucose. Crucially, it also acts on the hypothalamus in the brain to suppress appetite and increase the feeling of fullness.
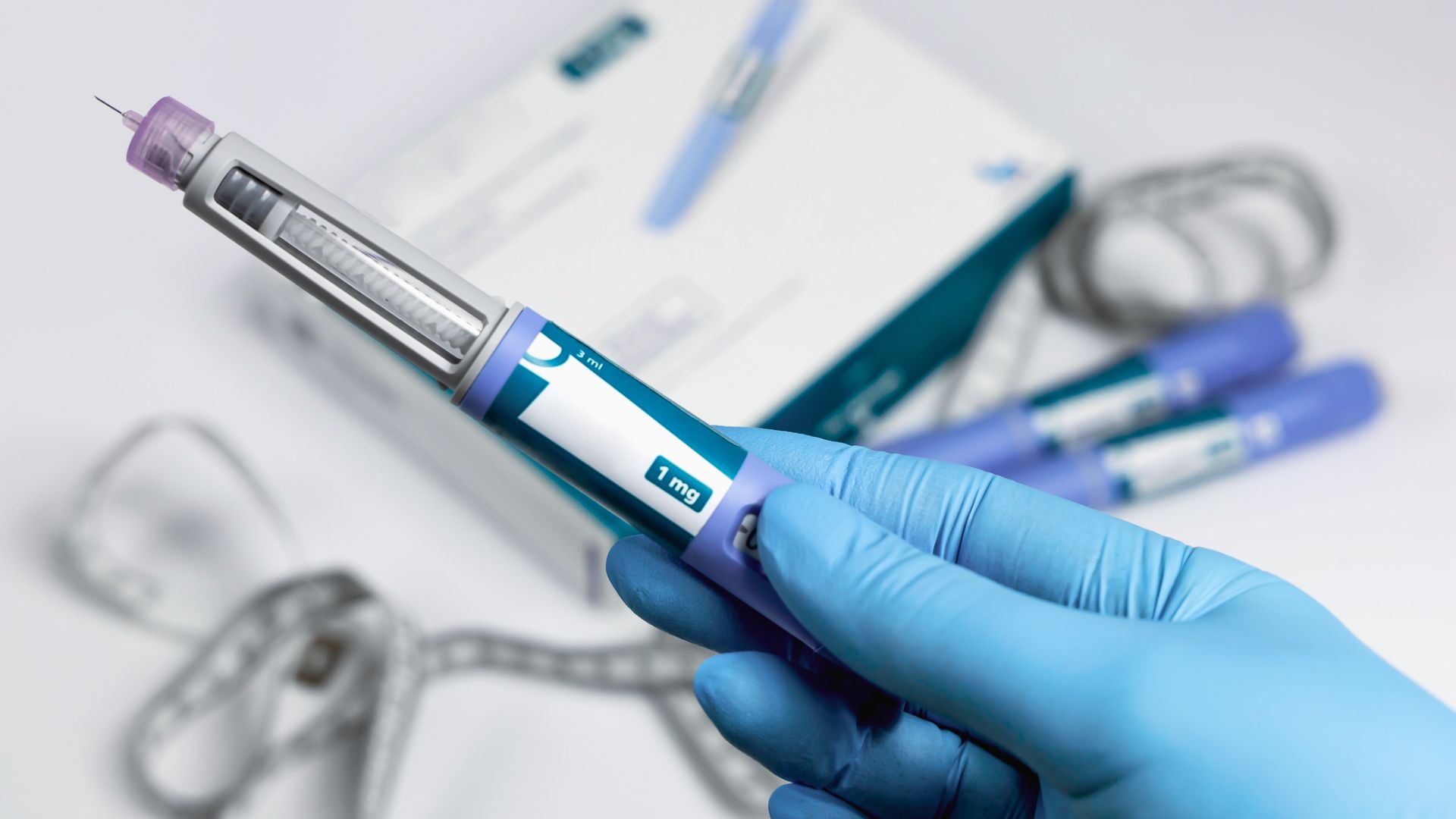
Medications like semaglutide mimic this hormone but are engineered to last much longer in the body than natural GLP-1. By maintaining high levels of this signal, the drugs slow gastric emptying—meaning food stays in the stomach longer—and diminish the “food noise” or intrusive thoughts about eating that many patients with obesity describe.
While semaglutide targets a single receptor, newer medications like tirzepatide are “dual agonists,” targeting both GLP-1 and glucose-dependent insulinotropic polypeptide (GIP) receptors. This dual action often results in even more pronounced weight loss and glycemic control, as noted in clinical trials published by the New England Journal of Medicine.
Clinical Benefits and the Cost of Rapid Loss
The primary appeal of these medications is their efficacy. In various clinical trials, participants using semaglutide experienced significant weight reduction, often ranging from 10% to 15% of their total body weight, depending on the dose and patient profile. Beyond the scale, these drugs have shown potential in reducing the risk of major adverse cardiovascular events, such as heart attack and stroke, in adults with overweight or obesity and established cardiovascular disease, according to FDA approvals.
However, the physiological transition is not without friction. The most common side effects are gastrointestinal, including nausea, vomiting, diarrhea, and constipation. These typically occur during the dose-escalation phase but can persist for some users.
More concerning to clinicians is the composition of the weight loss. When a person loses weight rapidly, they do not lose only fat; they also lose lean muscle mass. Without a high-protein diet and consistent resistance training, a significant portion of the weight lost can be muscle, which may lower the basal metabolic rate and make long-term weight maintenance more difficult.
Comparing Leading GLP-1 Medications
| Medication | Active Ingredient | Primary Target | Common Brand Names |
|---|---|---|---|
| Semaglutide | Semaglutide | GLP-1 Receptor | Ozempic, Wegovy |
| Tirzepatide | Tirzepatide | GLP-1 & GIP Receptors | Mounjaro, Zepbound |
| Liraglutide | Liraglutide | GLP-1 Receptor | Saxenda, Victoza |
Addressing “Ozempic Face” and Aesthetic Shifts
The speed of weight loss associated with these drugs has led to the emergence of “Ozempic face,” a non-medical term used to describe the gaunt, aged appearance that can occur after rapid fat loss in the cheeks and under the eyes. This is not a side effect of the drug itself, but rather a result of the rapid loss of subcutaneous facial fat, which provides structural support to the skin.
This phenomenon underscores a critical point: the body’s skin elasticity cannot always retain pace with the rapid metabolic changes induced by the medication. While cosmetic interventions can address these changes, the primary medical focus remains on the systemic health improvements—such as reduced blood pressure and improved insulin sensitivity—rather than aesthetic outcomes.
The Long-Term Reality: Maintenance and Access
One of the most pressing questions in the medical community is what happens when a patient stops the medication. Data suggests that for many, obesity is a chronic condition; without ongoing pharmacological support, the body often attempts to return to its previous “set point,” leading to weight regain.
This suggests that for a significant portion of the population, these medications may be long-term commitments rather than short-term fixes. This creates a secondary crisis of access and affordability, as insurance coverage for weight-loss medications remains inconsistent across different providers and employers.
the surge in demand has led to critical shortages of these drugs, sometimes depriving type 2 diabetes patients of essential glycemic control to make room for off-label weight loss use. This has prompted regulatory bodies to emphasize that these medications should only be used under strict medical supervision to avoid severe risks, such as pancreatitis or gallbladder disease.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition or treatment.
The next major milestone for this class of drugs will be the release of long-term cardiovascular and kidney outcome trials, which will determine if these medications can be transitioned from weight-loss tools to primary preventative treatments for metabolic syndrome. As research evolves, the goal remains a holistic approach that combines pharmacological intervention with sustainable nutritional and lifestyle changes.
We want to hear from you. Have you or a loved one navigated the transition to GLP-1 medications? Share your experiences in the comments below or share this article with your community.

