For many patients, the decision to undergo a cholecystectomy—the surgical removal of the gallbladder—comes as a sudden necessity, often triggered by the sharp, debilitating pain of gallstones. Once the anesthesia wears off and the surgical incisions initiate to heal, a common and pressing question emerges: how does the body function without an organ that seemed so vital to digestion?
The short answer is that while the gallbladder plays a helpful role in processing fats, it is not essential for survival. Millions of people live healthy, active lives after removal, though the transition requires a biological shift in how the body manages bile. Understanding the mechanics of living without a gallbladder allows patients to navigate their recovery with less anxiety and better dietary choices.
As a physician, I often observe patients who worry that they have lost a primary digestive engine. In reality, the gallbladder is more of a storage warehouse than a factory. The actual production of bile happens in the liver, and it is this continuous production that ensures the digestive system continues to function long after the gallbladder is gone.
The biological role of the gallbladder
To understand life after surgery, one must first understand what the gallbladder does. The liver produces bile, a greenish-brown fluid that acts as a detergent, breaking down large globules of fat into smaller droplets—a process called emulsification. This allows enzymes from the pancreas to digest those fats more efficiently.
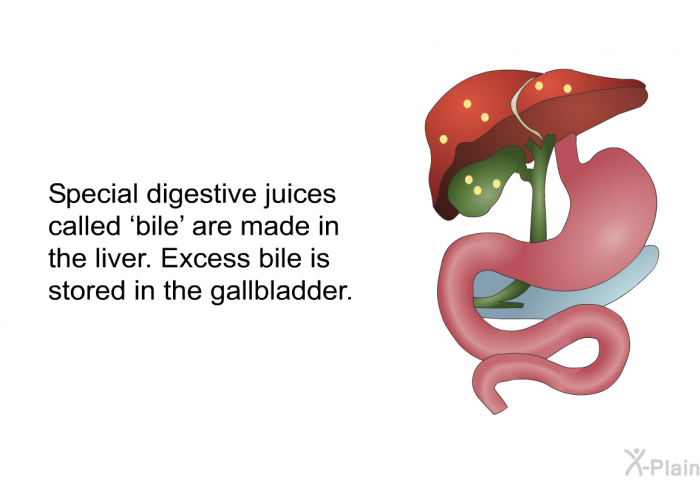
The gallbladder’s primary job is to store this bile and concentrate it, removing water to produce it more potent. When you eat a meal containing fats, the small intestine releases a hormone called cholecystokinin (CCK), which signals the gallbladder to contract and squeeze a concentrated dose of bile into the common bile duct and then into the duodenum.
When the gallbladder is removed, this “on-demand” delivery system is eliminated. Instead of a concentrated burst of bile arriving exactly when a fatty meal hits the stomach, bile now drips continuously and slowly from the liver directly into the small intestine, regardless of whether food is present. This change in delivery is the root of most post-surgical digestive adjustments.
Adapting to a recent digestive flow
The human body is remarkably adaptable. Following a cholecystectomy, the common bile duct—the tube that carries bile to the intestine—often undergoes a process of slight dilation. This allows the duct to hold a small amount of bile, partially mimicking the storage function of the missing gallbladder.
Yet, due to the fact that the bile is no longer concentrated, the body may struggle to process very high-fat meals. This can lead to a variety of gastrointestinal symptoms, most commonly steatorrhea (fatty stools) or urgent diarrhea. This happens because undigested fats reach the large intestine, where they draw in water and are fermented by bacteria, leading to bloating and loose stools.
Most patients discover that these symptoms are temporary. As the digestive tract adjusts to the steady drip of bile, the body typically reaches a new equilibrium. According to the Mayo Clinic, the majority of people experience no long-term digestive issues after the procedure.
Comparing bile delivery systems
| Feature | With Gallbladder | Without Gallbladder |
|---|---|---|
| Bile Source | Liver | Liver |
| Storage | Stored and concentrated in gallbladder | No storage. continuous flow |
| Delivery Method | Concentrated burst during meals | Steady, dilute drip into intestine |
| Fat Processing | Highly efficient for large fat loads | Best suited for moderate/small fat loads |
Navigating post-surgical recovery and diet
The immediate post-operative period is the most critical time for dietary management. Jumping straight back into a high-fat diet can overwhelm the liver’s steady drip of bile, leading to nausea, cramping, and severe diarrhea.
Medical professionals generally recommend a gradual reintroduction of fats. Starting with a low-fat diet for the first few weeks allows the digestive system to calibrate. Patients are encouraged to eat smaller, more frequent meals rather than three large ones, which prevents the small intestine from being overloaded with more fat than the available bile can handle.
Key dietary adjustments typically include:
- Prioritizing soluble fiber: Foods like oats, barley, and certain fruits can aid regulate bowel movements and reduce the likelihood of diarrhea.
- Monitoring fat triggers: Keeping a food diary to identify which specific fats (e.g., fried foods, heavy creams) trigger discomfort.
- Gradual introduction: Slowly adding healthy fats, such as avocado or olive oil, to test the body’s tolerance.
Understanding Post-Cholecystectomy Syndrome
While most recoveries are seamless, a small percentage of patients experience what is known as Post-Cholecystectomy Syndrome (PCS). This is not a single disease but a collection of symptoms—such as upper right abdominal pain, bloating, and indigestion—that persist or develop after the gallbladder is gone.
PCS can be caused by several factors, including bile leaking into the digestive tract, a retained stone in the common bile duct, or sphincter of Oddi dysfunction, where the valve controlling the flow of bile does not open and close correctly. Because these symptoms mimic the original gallbladder pain, it is essential for patients to seek a professional diagnosis to rule out complications.
Research published by the National Institutes of Health (NIH) suggests that while PCS is relatively uncommon, it requires a tailored medical approach, which may include medication to relax the bile duct or further imaging to ensure the biliary tree is clear.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition or surgical recovery.
The path forward for most patients is one of gradual return to normalcy. The next critical checkpoint for those recovering from surgery is the six-week post-operative follow-up, where surgeons typically assess the healing of the abdominal wall and evaluate the patient’s digestive tolerance. By focusing on mindful eating and listening to the body’s signals, most individuals find that the absence of a gallbladder is a small price to pay for the end of chronic gallstone pain.
Have you or a loved one navigated life after gallbladder removal? Share your experiences and recovery tips in the comments below.

