Our bodies don’t simply reset after an injury or infection. Tissues retain a kind of “memory” of inflammation, mounting faster and stronger responses to subsequent threats. But how this immunological memory persists – not just in immune cells, but within the very tissues themselves – has been a longstanding mystery. New research published in Science sheds light on this process, identifying specific DNA sequence features in stem cells that appear to lock in these inflammatory responses, even across cell divisions. Understanding these mechanisms could open new avenues for treating chronic inflammatory diseases and improving vaccine efficacy.
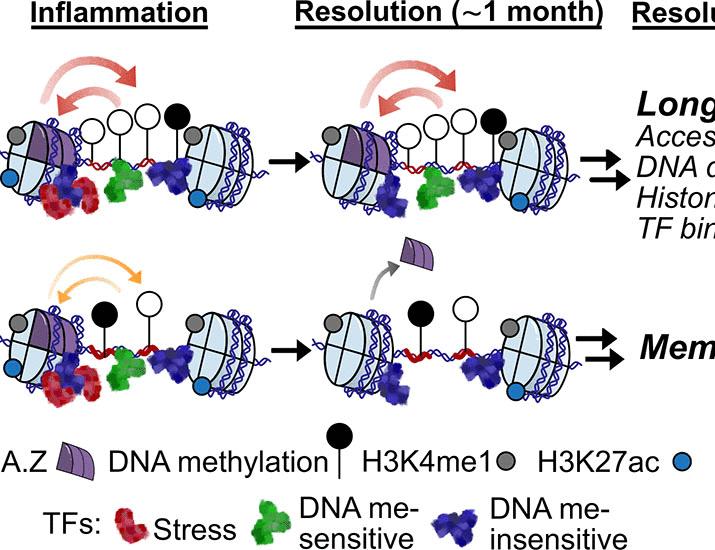
The study, conducted in mice, focuses on epidermal stem cells – the regenerative powerhouses of the skin. Researchers found that after an initial inflammatory event, these cells undergo epigenetic changes, alterations to DNA that don’t change the sequence itself but affect how genes are expressed. These changes aren’t random; they’re linked to specific DNA sequence features, essentially creating a lasting record of the inflammation. This is a significant finding because it suggests that inflammatory memory isn’t solely reliant on the lifespan of immune cells, but can be encoded within the tissue itself. The team demonstrated that these changes heightened the skin’s response to subsequent inflammatory challenges.
How Inflammatory Memory Takes Hold
The research team, led by Dr. Yasmine Belkaid at the National Institute of Allergy and Infectious Diseases (NIAID), part of the National Institutes of Health, investigated the molecular mechanisms behind this phenomenon. They discovered that certain DNA sequences, known as enhancers, develop into more accessible after inflammation. Enhancers are regions of DNA that boost gene expression, and their increased accessibility allows for heightened production of inflammatory molecules when the tissue is challenged again. NIAID has been at the forefront of immunological research for decades.
“What’s remarkable is that these epigenetic changes are maintained over time and through cell division,” explains Dr. Belkaid in a related NIAID news release. “This suggests that the tissue itself is ‘remembering’ the inflammatory event and preparing for future encounters.” The study pinpointed a specific protein, the histone methyltransferase MMSET, as playing a crucial role in establishing and maintaining these epigenetic marks. Blocking MMSET activity disrupted the inflammatory memory, demonstrating its importance in the process.
The Role of Epigenetics in Long-Term Immunity
Epigenetics is increasingly recognized as a key player in immunity and disease. These modifications to DNA can be influenced by environmental factors, such as infection and inflammation, and can have lasting effects on gene expression. The National Human Genome Research Institute provides a comprehensive overview of epigenetics and its implications.
This research builds on previous work showing that tissues can exhibit immunological memory. For example, studies have demonstrated that the lungs can “remember” previous viral infections, leading to a faster and more effective response upon re-exposure. However, the underlying mechanisms have remained largely elusive. This new study provides a crucial piece of the puzzle, identifying the specific DNA sequence features and epigenetic regulators involved in establishing and maintaining this memory in epidermal stem cells.
Implications for Chronic Disease and Vaccine Development
The findings have significant implications for understanding and treating chronic inflammatory diseases, such as eczema, psoriasis, and rheumatoid arthritis. In these conditions, persistent inflammation can lead to tissue damage and impaired function. If researchers can identify ways to modulate the epigenetic changes that drive inflammatory memory, they may be able to develop new therapies that dampen down the chronic inflammatory response.
this research could inform vaccine development. A key goal of vaccination is to create long-lasting immunological memory. Understanding how tissues store inflammatory memories could lead to strategies for enhancing vaccine efficacy and developing vaccines that provide more durable protection. The ability to prime tissues for a faster, more robust response could be particularly valuable for vaccines against rapidly evolving pathogens, like influenza or SARS-CoV-2.
The study also raises questions about the potential for “trained immunity,” where prior exposure to one pathogen can alter the immune response to subsequent, unrelated pathogens. Even as the benefits of trained immunity are clear – enhanced protection against infection – there is also the potential for unintended consequences, such as increased susceptibility to autoimmune diseases. Further research is needed to fully understand the complex interplay between inflammatory memory, trained immunity, and overall immune homeostasis.
What’s Next in Understanding Tissue Memory
The researchers plan to investigate whether similar mechanisms operate in other tissues and cell types. They also want to explore the role of environmental factors, such as diet and lifestyle, in shaping inflammatory memory. A key area of future research will be to determine how these epigenetic changes are transmitted across generations, potentially influencing the susceptibility of offspring to inflammatory diseases. The team is also working to identify potential therapeutic targets for modulating inflammatory memory in humans.
This research represents a significant step forward in our understanding of how tissues “remember” inflammation. By unraveling the molecular mechanisms involved, scientists are paving the way for new strategies to prevent and treat chronic inflammatory diseases and improve vaccine effectiveness. The field of epigenetic longevity and its impact on immune response is rapidly evolving, and continued investigation promises to yield further insights into the complex relationship between our genes, our environment, and our health.
Disclaimer: This article is for informational purposes only and should not be considered medical advice. Please consult with a qualified healthcare professional for any health concerns or before making any decisions related to your health or treatment.
Have thoughts on this research? Share your comments below, and please share this article with your network!