Identifying the early stages of Parkinson’s disease is often a complex journey, not because the symptoms are invisible, but because they are frequently mistaken for the natural effects of aging or unrelated health conditions. For many patients, the path to a correct diagnosis is delayed when initial Parkinson’s symptoms—such as a slight tremor or a change in gait—are dismissed as “just getting older.”
As a physician, I have seen how these subtle neurological shifts can be overlooked. The challenge lies in the fact that Parkinson’s does not always begin with the classic “pill-rolling” tremor. Instead, it often manifests as non-motor symptoms that affect a person’s quality of life long before the movement disorders become obvious to a casual observer or a general practitioner.
Early detection is critical because it allows for the implementation of neuroprotective strategies and symptom management that can significantly improve long-term outcomes. When we misinterpret these signs, we lose a vital window of opportunity to optimize a patient’s care plan and provide them with the necessary support systems.
The Hidden Signs: What Often Goes Unnoticed
While the medical community recognizes the “cardinal” symptoms of Parkinson’s—tremor, rigidity, and bradykinesia (slowness of movement)—there is a wide array of prodromal symptoms that appear years before the motor deficits. These are the signs most frequently misinterpreted by both patients and clinicians.
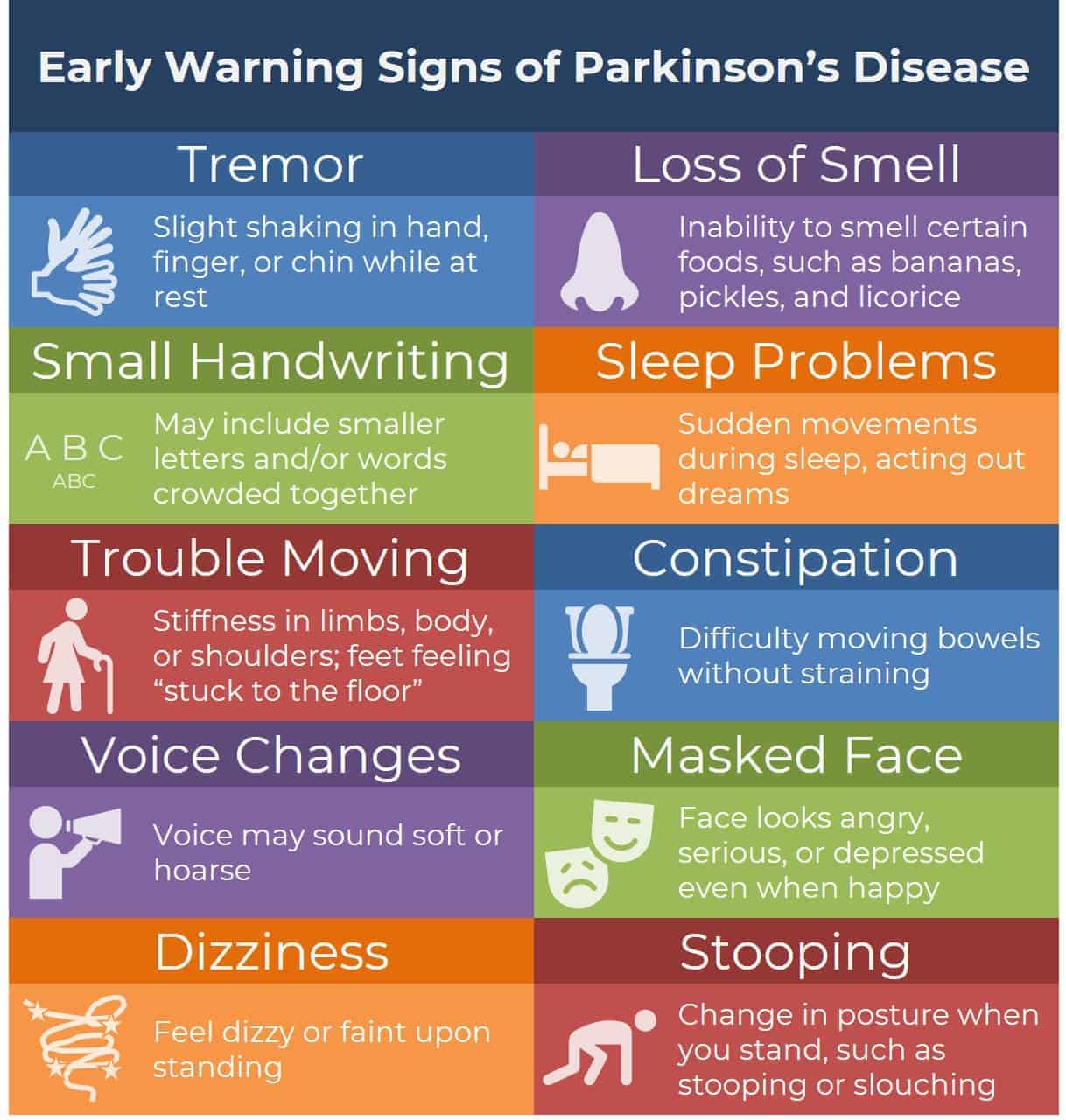
One of the most common overlooked signs is a diminished sense of smell, known as anosmia. While many people associate a loss of smell with a common cold or chronic sinusitis, in the context of Parkinson’s, This proves often one of the earliest indicators of the disease’s progression. Similarly, REM sleep behavior disorder, where patients physically act out their dreams, is frequently mistaken for simple insomnia or vivid dreaming, yet it is a strong predictor of future alpha-synuclein pathology.
Constipation is another frequent “invisible” symptom. Because gastrointestinal issues are so common across all age groups, chronic constipation is rarely linked to a neurological condition during a routine check-up. However, the dysfunction of the autonomic nervous system often precedes the movement issues that define the disease.
Distinguishing Aging from Pathology
The nuance between “normal aging” and “early Parkinson’s” can be slim. For example, a slight stiffness in the shoulders or hips is often attributed to arthritis. However, Parkinsonian rigidity is different; it is a systemic muscle stiffness that affects the trunk and limbs, often resulting in a “masked face” (hypomimia), where the facial expressions become less animated.
Micrographia, or the shrinking of handwriting, is another hallmark that is often ignored. A patient may notice that their writing has become smaller and more cramped, but they may simply assume their eyesight is failing or their hand is becoming less steady with age. In reality, this is a manifestation of bradykinesia affecting the fine motor skills of the hand.
The Impact of Misinterpretation on Diagnosis
When these signs are misinterpreted, the time to diagnosis can be stretched by years. This delay is not merely a matter of labeling; it affects the psychological well-being of the patient and the efficacy of early intervention. The Parkinson’s Foundation emphasizes that while there is no cure, early management of symptoms through medication and physical therapy can maintain independence for a longer period.
The diagnostic process remains primarily clinical, meaning it relies on a neurologist’s observation and the patient’s history rather than a single blood test. This makes the accuracy of the initial symptom report vital. If a patient does not mention their sleep disturbances or loss of smell because they believe these are irrelevant, the clinician may miss the full picture.
| Symptom | Common Misinterpretation | Neurological Reality |
|---|---|---|
| Loss of smell | Aging or nasal congestion | Early olfactory bulb degeneration |
| REM sleep disorder | Stress or vivid dreams | Brainstem dysfunction |
| Constipation | Dietary issues or aging | Autonomic nervous system failure |
| Small handwriting | General clumsiness | Fine motor bradykinesia |
| Stiff posture | Arthritis or “stiffness” | Muscle rigidity |
Navigating the Path to Care
For those observing these signs in themselves or a loved one, the next step is a comprehensive neurological evaluation. It is helpful to keep a “symptom diary” that tracks not just tremors, but changes in mood, sleep patterns, and balance. Depression and anxiety are also common non-motor symptoms that can appear years before the physical shakes, often leading patients to seek psychiatric help before neurological care.
Modern management focuses on a multidisciplinary approach. This includes not only the prescribing physician but also physical therapists to address gait and balance, and speech-language pathologists to help with the subtle softening of the voice (hypophonia) that often accompanies the disease. According to the Mayo Clinic, the goal of treatment is to manage symptoms and maintain the highest possible quality of life.
The integration of exercise, particularly aerobic activity and strength training, has been shown to potentially slow the progression of motor symptoms. When a diagnosis is made early, patients can establish these habits before the disease severely limits their mobility.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
Research continues into biomarkers that could allow for a definitive biological test for Parkinson’s, potentially replacing the current reliance on clinical observation. The next major milestone in this field is the ongoing validation of skin and spinal fluid tests designed to detect alpha-synuclein aggregates, which could revolutionize how we identify the disease in its earliest, most treatable stages.
We invite you to share this information with your community to help raise awareness of these hidden symptoms. Have you or a loved one experienced these early signs? Share your thoughts in the comments below.

