Postmenopausal bleeding, defined as any vaginal bleeding occurring six months or more after the cessation of menstruation, affects roughly 10% of women after menopause. While often benign, it can signal underlying conditions ranging from endometrial atrophy to, in a small percentage of cases, endometrial cancer. Accurate diagnosis relies heavily on a thorough evaluation, including histopathological examination of endometrial samples. A recent study published in Cureus investigated the patterns observed in these samples and how they correlate with clinical and radiological findings, aiming to refine diagnostic approaches for this common concern.
The study, conducted by researchers at multiple institutions in Pakistan, retrospectively analyzed data from 150 postmenopausal women presenting with postmenopausal bleeding. Researchers sought to determine the prevalence of different histopathological patterns in endometrial biopsies and to assess their relationship with factors like age, body mass index (BMI), ultrasound findings, and the presence of risk factors for endometrial cancer. Understanding these correlations is crucial for optimizing patient management and minimizing unnecessary procedures.
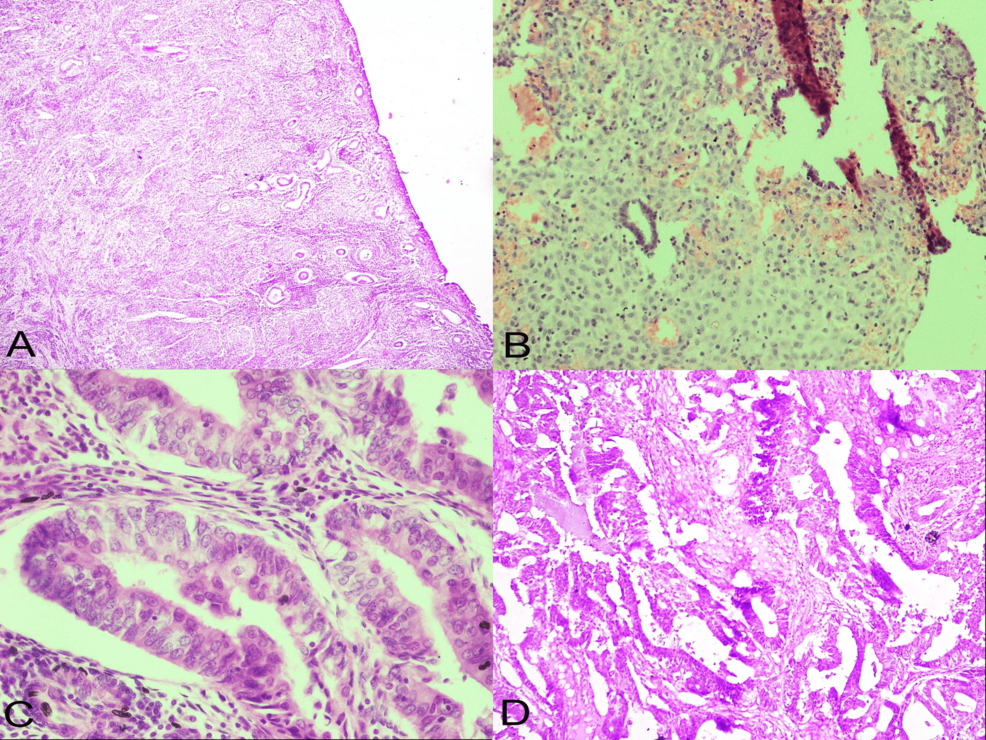
Histopathological Findings: A Spectrum of Patterns
The histopathological evaluation revealed a diverse range of endometrial patterns. The most common finding was proliferative endometrium, observed in 36% of the cases. This indicates the endometrium is thickening in response to estrogen, and while not cancerous, requires further investigation to rule out other causes. Endometrial atrophy, a thinning of the endometrial lining due to decreased estrogen levels, was found in 28% of the patients. Simple hyperplasia without atypia, a thickening of the endometrium without abnormal cell growth, was present in 16% of the samples.
More concerning findings included complex hyperplasia with atypia (8%), which carries a higher risk of progressing to cancer, and endometrial carcinoma (12%). The study also identified cases of endometrial polyps (10%) and other less common patterns. The researchers emphasized that the presence of atypia, whether in hyperplasia or carcinoma, is a critical factor in determining treatment strategies.
Correlation with Clinical and Radiological Features
The study found several significant correlations between histopathological findings and clinical and radiological characteristics. Women with endometrial carcinoma tended to be older, with an average age of 64.2 years, compared to those with benign findings. Obesity, with a BMI greater than 30, was also significantly associated with endometrial carcinoma and hyperplasia with atypia. This aligns with established knowledge that obesity is a risk factor for endometrial cancer due to increased estrogen production in adipose tissue. The National Cancer Institute details these risk factors further.
Ultrasound findings also proved valuable in predicting histopathological results. An increased endometrial thickness, measured by transvaginal ultrasound, was strongly correlated with hyperplasia and carcinoma. Specifically, an endometrial thickness greater than 4mm was associated with a higher likelihood of malignancy. However, the study noted that ultrasound is not foolproof, and false negatives can occur, highlighting the necessity of biopsy for definitive diagnosis.
The Importance of Endometrial Biopsy
The researchers underscored the critical role of endometrial biopsy in the evaluation of postmenopausal bleeding. While transvaginal ultrasound can provide valuable initial information, it cannot reliably differentiate between benign and malignant conditions. Histopathological examination of the biopsy sample remains the gold standard for diagnosis, allowing for accurate identification of cellular abnormalities and guiding appropriate treatment decisions.
The study also highlighted the importance of considering individual patient risk factors when interpreting biopsy results. Women with risk factors for endometrial cancer, such as obesity, diabetes, hypertension, and a history of infertility, may require more aggressive evaluation and management even in the presence of seemingly benign histopathological findings.
Limitations and Future Directions
The study acknowledged several limitations, including its retrospective design and the fact that it was conducted at a single center. These factors may limit the generalizability of the findings. The study did not include information on hormone replacement therapy (HRT) use, which is a known risk factor for endometrial cancer.
Future research should focus on larger, prospective studies that incorporate a wider range of clinical and radiological variables, including HRT use and more detailed ultrasound parameters. The development of more sensitive and specific biomarkers for endometrial cancer could also help to improve diagnostic accuracy and reduce the demand for unnecessary biopsies.
The findings from this study reinforce the importance of a comprehensive approach to the evaluation of postmenopausal bleeding. By integrating clinical assessment, radiological imaging, and histopathological examination, clinicians can provide optimal care for women experiencing this common symptom. The next step in improving care will likely involve refining risk stratification models and exploring novel diagnostic tools to further enhance the accuracy and efficiency of endometrial cancer detection.
If you are experiencing postmenopausal bleeding, We see essential to consult with your healthcare provider for a thorough evaluation. Early diagnosis and appropriate management can significantly improve outcomes.
Disclaimer: This article is for informational purposes only and should not be considered medical advice. Please consult with a qualified healthcare professional for any health concerns or before making any decisions related to your health or treatment.