For decades, a diagnosis of multiple myeloma was managed primarily through a linear relationship between a patient and their hematologist. The physician prescribed the chemotherapy, monitored the blood perform, and adjusted the dosage. But as the therapeutic landscape for this complex plasma cell cancer has expanded from a handful of options to a sophisticated arsenal of immunotherapies and targeted agents, the “solo doctor” model has turn into insufficient.
Today, collaborative care in multiple myeloma is redefining the boundaries of survival. The shift toward a multidisciplinary team (MDT) approach—where specialists in oncology, pharmacology, nursing, and supportive care synchronize their efforts—is transforming the disease from a rapid decline into a manageable chronic condition for many. This evolution is not merely about adding more people to a patient’s chart; it is about the integrated coordination of highly complex therapies that require precise timing and vigilant toxicity management.
The stakes for this coordination are high. Modern treatments, including CAR-T cell therapies and bispecific antibodies, offer unprecedented response rates but carry risks such as cytokine release syndrome (CRS) and neurotoxicity. Managing these risks requires a seamless loop of communication between the treating physician, the transplant team, and the intensive care unit. When these entities function as a single unit, patients experience fewer complications and more sustainable long-term outcomes.
The Architecture of the Multidisciplinary Team
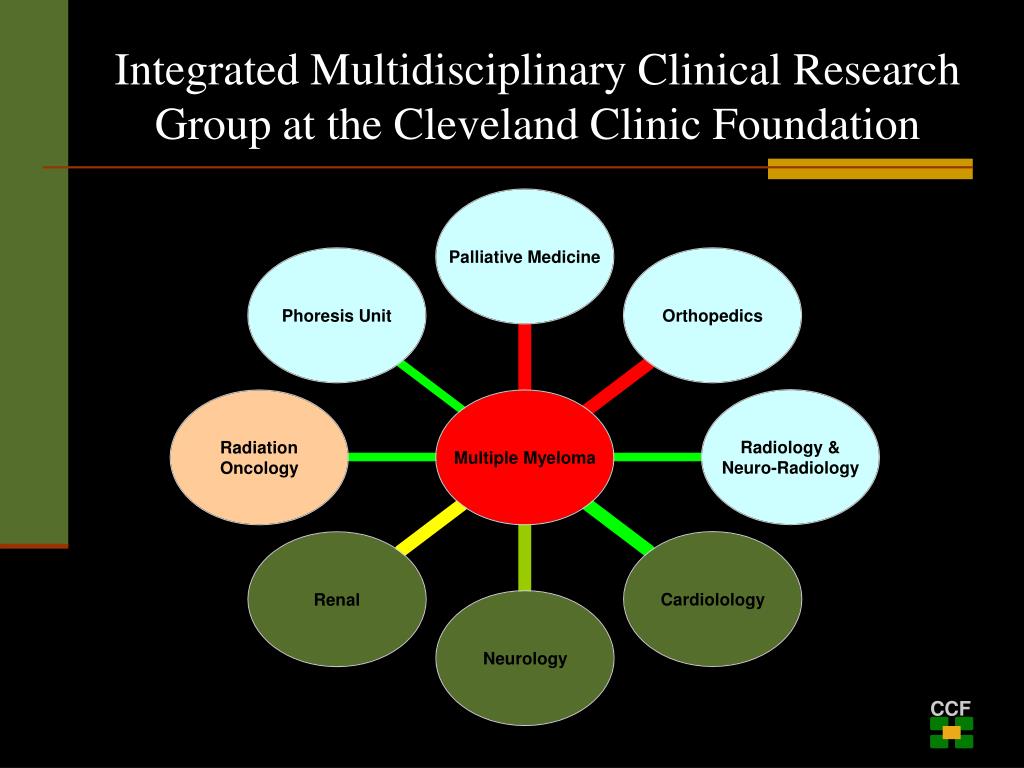
A collaborative care model replaces the traditional hierarchy with a hub-and-spoke system. At the center is the patient, surrounded by a team that addresses the biological, physical, and psychological facets of the disease. This team typically includes a hematologist-oncologist, a specialized oncology pharmacist, a nurse navigator, and often a bone marrow transplant specialist.
The role of the oncology pharmacist has become particularly critical. With the introduction of “quadruplet” therapies—combinations of four different drugs used to induce remission—the potential for drug-drug interactions and cumulative toxicity is significant. Pharmacists in a collaborative setting do more than dispense medication; they actively participate in dosing adjustments and patient education to ensure adherence and safety.
Equally vital is the nurse navigator. These professionals serve as the connective tissue of the care plan, ensuring that a patient doesn’t fall through the cracks between a biopsy appointment, a pharmacy refill, and a supportive care visit. By reducing the administrative burden on the patient, navigators help maintain the rigorous schedules required for the most effective outcomes.
Navigating the Complexity of Modern Therapies
The necessity of collaborative care is most evident in the administration of advanced cellular therapies. For patients who have failed multiple lines of treatment, CAR-T cell therapy represents a significant leap in survival potential. However, the process—which involves collecting a patient’s T cells, genetically modifying them, and re-infusing them—is a logistical and medical marathon.
Because CAR-T and bispecific antibodies can trigger systemic inflammatory responses, the collaborative model integrates “trigger protocols.” These are pre-arranged, multidisciplinary agreements that dictate exactly when a patient moves from a clinic setting to a hospital bed, who is notified, and which medications are administered first. This prevents the delays that can occur in fragmented care systems, where a patient might wait for a consulting physician to be paged whereas their condition deteriorates.
Beyond the acute phase, the team approach enables “precision medicine.” By integrating genomic sequencing and molecular profiling into the team’s discussions, specialists can tailor treatments to the specific genetic mutations of a patient’s myeloma, rather than relying on a one-size-fits-all protocol.
Addressing the “Whole Patient” and Quality of Life
Survival is no longer the only metric of success in multiple myeloma. As the American Society of Hematology and other leading bodies emphasize, the goal has shifted toward “survival with quality.” Multiple myeloma often attacks the skeletal system, leading to bone fractures and severe pain, while the treatments themselves can cause peripheral neuropathy and fatigue.

Collaborative care integrates supportive services directly into the primary treatment plan. This includes physical therapists to prevent falls, nutritionists to combat cachexia (muscle wasting), and palliative care specialists who manage pain and psychological distress from the moment of diagnosis. When these services are integrated, patients are more likely to stay on their primary cancer treatments because their side effects are managed proactively rather than reactively.
| Feature | Traditional Care Model | Collaborative (MDT) Model |
|---|---|---|
| Decision Making | Physician-led; linear | Team-based; consensus-driven |
| Toxicity Management | Reactive (treated as they arise) | Proactive (integrated monitoring) |
| Patient Coordination | Patient manages appointments | Nurse navigator coordinates care |
| Treatment Scope | Focused primarily on oncology | Holistic (Nutrition, PT, Psych) |
The Impact on Long-Term Survival
The data suggests that the synergy of a multidisciplinary approach correlates with improved progression-free survival (PFS). When treatment is coordinated, “treatment holidays” or unplanned interruptions due to toxicity are minimized, keeping the disease in remission for longer periods. The psychological support embedded in collaborative care reduces the incidence of treatment-related depression, which is a known factor in patient non-compliance.
According to data from the SEER database, the relative 5-year survival rate for multiple myeloma has seen a steady increase over the last two decades. While the development of new drugs is the primary driver, the ability to deliver these drugs safely and consistently through collaborative frameworks is what allows patients to actually reach those survival milestones.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Patients should consult with their own healthcare provider for diagnosis and treatment options.
The next frontier for collaborative care lies in the integration of real-world evidence (RWE) and AI-driven monitoring. Clinical teams are beginning to use wearable technology to track patient activity and sleep patterns in real-time, allowing the MDT to intervene before a side effect becomes a crisis. As these tools become standard, the definition of survival will continue to expand from merely extending life to optimizing the lived experience of every patient.
We invite readers to share their experiences with multidisciplinary care or ask questions in the comments below to help foster a community of informed support.