- Jack Janter
- BBC News
Image source, A SOUND
An American man has become the first person to receive a genetically modified pig’s heart through transplant surgery.
David Bennett, 57, was too ill to qualify for the human heart. But doctors say he is still healthy three days after completing a seven-hour treatment for a pig’s genetically modified heart.
Many appreciate this experimental surgery as it is a medical breakthrough that can reduce the waiting time for humans for transplant surgery and change the lives of patients around the world. But some question whether this practice can be ethically justified in reality.
They point to potential ethical issues that this treatment could cause in patients’ care, animal rights, and religious concerns.
That’s right. How controversial are transplant surgeries that fit pig organs into humans?
Clinical implications
It is an experimental surgery and has the potential to pose a great risk to the patient.
Even well-fitting human organs can be discarded after they have been transplanted – thus putting them at greater risk when it comes to animal organs.
For decades, doctors have been trying to use animal organs, called geno-transplantation, for humans. They have also had mixed success.
In 1984, doctors in California tried to save the heart of a baby girl by fitting the heart of a baboon monkey, but the woman died 21 days later.
Although such treatments are very risky, some medical ethics medical experts say that if patients are aware of that risk they should still go ahead with that experimental treatment.
“You never know if the person is going to have a catastrophe soon after treatment – but you can not continue treatment without risking it,” said Professor Julian Chaulescu, head of the Department of Practical Ethical Medicine at Oxford University.
“I think people will agree to these serious tests until the individual fully understands the risks,” he added.
Professor Chaulescu says it is important that they are given all the options, including mechanical heart support or human transplant surgery.
Doctors who worked on Bennett’s case say the surgery was justified because he had no other treatment and he would have died if it had not.
Image source, University of Maryland School of Medicine
Professor Saulescu must have undergone “a very rigorous tissue and non-human animal examination” to ensure that the procedure is safe before any surgery.
Bennett’s transplant surgery was not performed as part of a clinical trial and is usually required for experimental treatments. And the drugs he was given have not yet been tested for use in non-human animals.
“We have been doing this in the laboratory, on animals for decades, trying to get to the point where we think it’s safe to give this to a human user,” he told the BBC.
AnimalOn Rights
With current progress Bennett’s treatment has re-ignited the debate about the use of pigs for human transplant surgery. However, this initiative is opposed by many animal rights groups.
The People for the Ethical Treatment of Animals (PETA), an animal welfare organization, has condemned Bennett’s pig transplant surgery as “unethical, dangerous and a waste of enormous resources.”
“Animals are not tools to be tested, but complex, intelligent creatures,” PETA said.
Proponents of her case have been working to make the actual transcript of this statement available online. Scientists have modified 10 genes from a pig whose heart was used for Bennett’s transplant, so it was not discarded by his body.
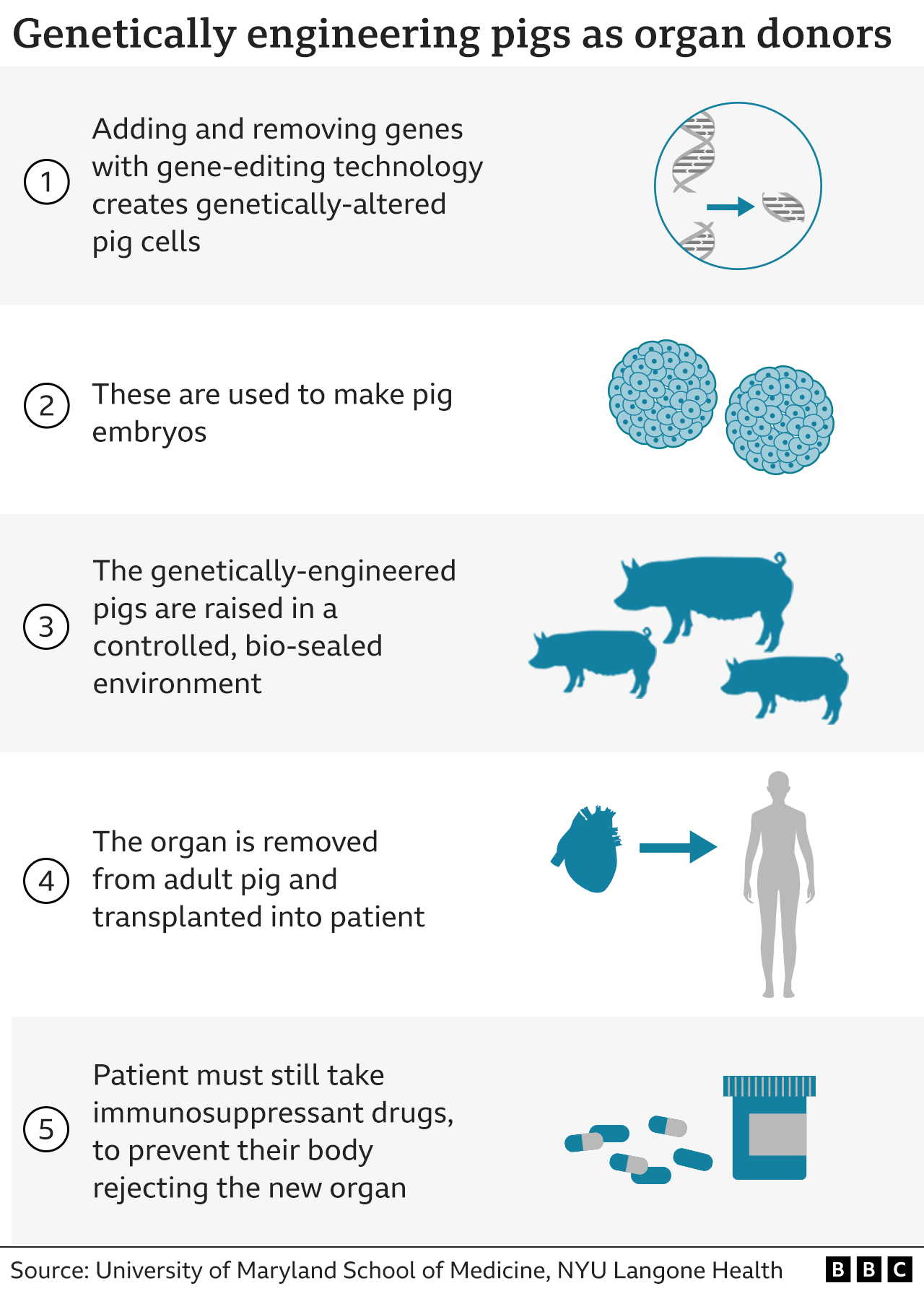

Earlier, on the morning of the operation, the pig’s heart was removed.
A spokesman for Animal Aid, a UK-based animal rights group, told the BBC he was opposed to altering animal genes or genotransplants “under any circumstances.”
“Animals have the right to live their lives without being genetically manipulated with all the pain and trauma, only to be killed and have their organs harvested,” the organization said.
Some campaigners are concerned about the unknown long-term effects of genetic modification on pig health.
Dr. Gatrian DeVolter, a member of the Oxford University Biosynthesis Medical Group, says that only genetically modified pigs should be used for organ transplants “if it is possible to make sure they are not unnecessarily harmful.”
“Using pigs to produce meat is more complicated than using them to save lives, but there is no reason to neglect animal welfare here,” he says.

Image source, Getty Images
Religion
In this case, there is another confusion surrounding those who believe that getting an animal organ is tricky. They have been chosen because the organs of pigs can be matched to humans. But how does this choice affect Jewish or Muslim patients? Which religion has strict rules against the use of animals? Although the Jewish law prohibits Jews from raising or eating pigs, getting a pig’s heart does not in any way violate their dietary laws, says Moshe Friedman, a senior physician on the UK Department of Health’s ethical and ethical advisory board. “Since the primary concern in Jewish law is to protect human life, a Jewish patient will be obliged to accept a transplant from an animal that will have a greater chance of survival and a better quality of life in the future,” said Rabbi Friedman. BBC.
In Islam, it is said that the animal organ can be used to fulfill a need to save a person’s life.
The Fatwa Organization of Egypt’s religious ruling, Dar al-Ifta, said: “Fear for the patient’s life, loss of one of his organs, exacerbation of the disease, or persistence may allow the pig to fit the heart valves.”
Even if someone rejects animal transplant surgery on the basis of religion or ethics, Professor Chaulescu says they should not be given the lowest priority on the waiting list for human organ donors.
Other News:
BBC Tamil on social media:
Source: BBC.com
