As the colder months approach, health officials in Tasmania are urging residents to take proactive steps to prepare, plan and protect against respiratory illness this winter. With the seasonal surge of influenza, COVID-19, and Respiratory Syncytial Virus (RSV), the Tasmanian Department of Health is emphasizing a multi-layered approach to prevention to reduce the burden on the state’s healthcare system and protect vulnerable populations.
The strategy focuses on a combination of immunization, hygiene, and early intervention. For many, this means updating vaccinations before the peak of the winter season, as the window for maximum efficacy is narrowest when the viruses are most prevalent. Health authorities are particularly concerned with “co-infections,” where an individual may contract two different respiratory viruses simultaneously, potentially complicating recovery and increasing the risk of severe illness.
This year’s guidance is designed to address the evolving nature of respiratory pathogens. While the public has become accustomed to COVID-19 protocols, the return of traditional seasonal flu and the impact of RSV—especially in infants and the elderly—requires a broader perspective on public health. The goal is to flatten the peak of winter admissions, ensuring that hospitals can maintain standard care levels without being overwhelmed by preventable respiratory cases.
From a clinical perspective, the timing of these interventions is critical. The Department of Health recommends that individuals consult their healthcare providers early to determine which vaccines are appropriate for their specific health profile, age, and risk level.
The Pillars of Winter Respiratory Protection
Preventing the spread of respiratory illness requires more than a single action; it necessitates a “Swiss cheese” model of defense, where multiple layers of protection work together to catch what others might miss. The primary defense remains vaccination, which serves to prime the immune system and reduce the likelihood of hospitalization.
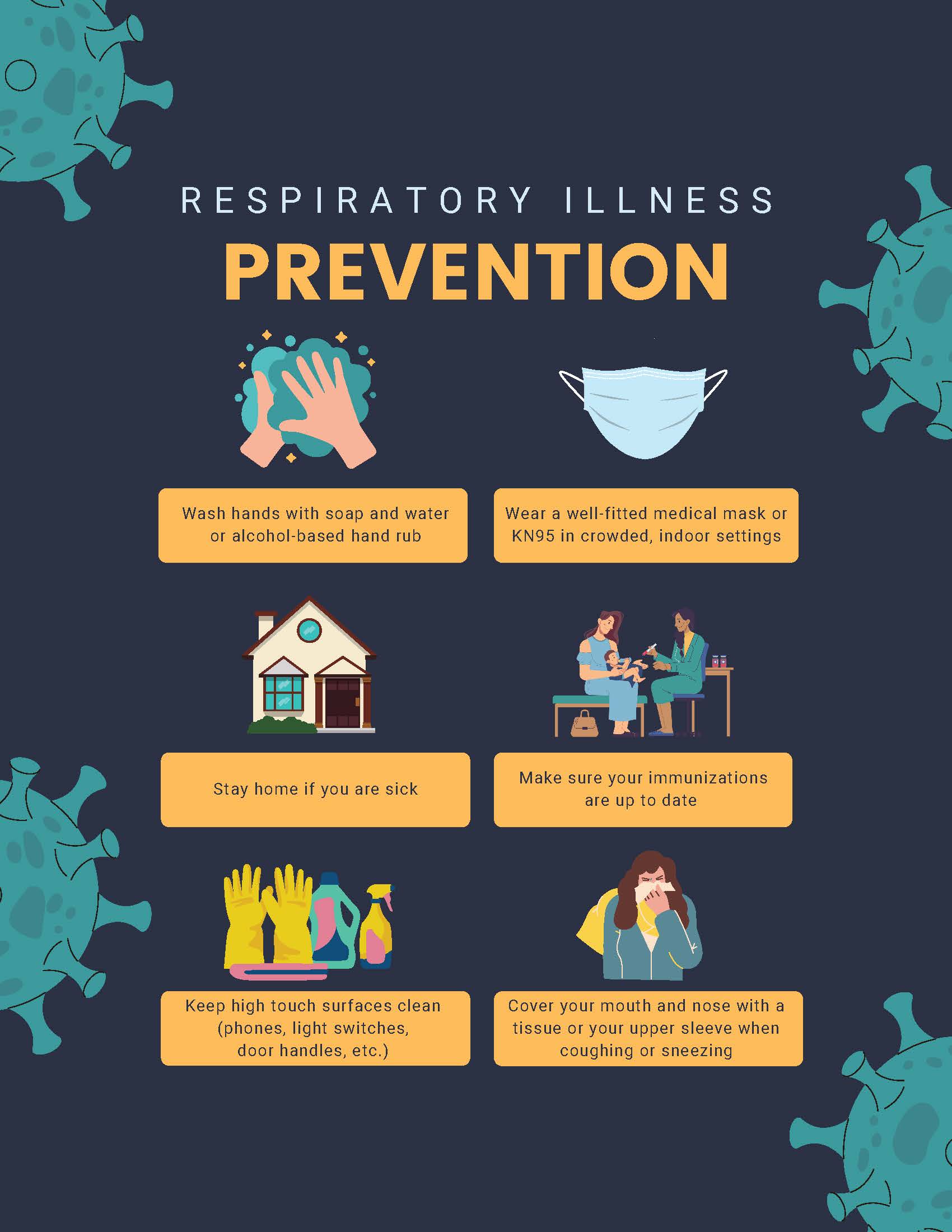
Beyond vaccines, the Department of Health highlights several non-pharmaceutical interventions that remain highly effective. These include regular handwashing with soap and water, using alcohol-based hand sanitizers when soap is unavailable, and practicing respiratory etiquette—such as covering coughs and sneezes with a tissue or the crook of the elbow.
Ventilation also plays a pivotal role in reducing viral load in shared spaces. Increasing airflow by opening windows or using air filtration systems can help disperse viral particles that linger in stagnant indoor air, a common occurrence during the winter when buildings are sealed tight to keep in the heat.
Understanding the Risks: Who is Most Affected?
While respiratory illnesses can affect anyone, certain groups face a significantly higher risk of severe complications. Identifying these high-risk cohorts allows for more targeted protection and prioritization of medical resources.
- Infants and Young Children: Particularly susceptible to RSV, which can cause bronchiolitis and pneumonia in very young lungs.
- The Elderly: Individuals aged 65 and over are at higher risk for complications from influenza and COVID-19 due to naturally waning immune function.
- Immunocompromised Individuals: Those undergoing chemotherapy, organ transplant recipients, or people with chronic conditions like diabetes.
- People with Chronic Lung Disease: Individuals with asthma or Chronic Obstructive Pulmonary Disease (COPD) may experience more severe exacerbations when infected.
For these groups, the “plan” part of the health department’s advice involves having a clear understanding of when to seek medical help and ensuring that their current medications are up to date. This prevents the “crisis-mode” visits to emergency departments that can be avoided with early GP intervention.
Navigating the Healthcare System During a Surge
When illness does strike, knowing where to move is as important as knowing how to prevent it. The Tasmanian health system operates on a tiered approach to manage the winter influx. The first point of contact should almost always be a primary care provider or a local pharmacy for initial assessment and advice.

If symptoms escalate, the Tasmanian Department of Health recommends monitoring for “red flag” symptoms. These include difficulty breathing, chest pain, or a high fever that does not respond to medication. In such cases, urgent care or emergency department visits are necessary.
To help residents organize their approach, the following table outlines the general triage and action plan for respiratory symptoms:
| Symptom Level | Common Indicators | Recommended Action |
|---|---|---|
| Mild | Runny nose, sore throat, mild cough | Rest, hydration, monitor symptoms |
| Moderate | Fever, muscle aches, persistent cough | Contact GP or pharmacist; isolate |
| Severe | Shortness of breath, confusion, blue lips | Immediate Emergency Department visit |
The Importance of Isolation and Testing
A critical component of protecting the community is the practice of staying home when unwell. The Department of Health stresses that “powering through” a cold or flu not only slows recovery for the individual but risks infecting colleagues, classmates, and vulnerable family members.
Testing remains a vital tool for clinical management. While many respiratory viruses present similarly, knowing whether a patient has COVID-19, influenza, or another pathogen allows doctors to prescribe the correct antiviral treatments if applicable. Rapid Antigen Tests (RATs) provide a quick first check, but PCR tests remain the gold standard for accuracy and subspecies identification.
The transition from a pandemic-era mindset to a seasonal-management mindset does not mean the risks have disappeared. It means the tools for management—vaccines, tests, and hygiene—are now integrated into standard winter health routines. By adhering to these guidelines, residents contribute to a collective effort to keep the state’s hospitals functioning efficiently.
Disclaimer: This article is for informational purposes only and does not constitute professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.
As the season progresses, the Tasmanian Department of Health will continue to monitor viral surveillance data to provide updates on vaccine efficacy and current infection rates. Residents are encouraged to check official health portals for the most recent data on local outbreaks and clinic availability.
We invite you to share this guide with your community and leave your thoughts or questions in the comments below to help others stay informed this winter.