For a woman living with a heart condition, the desire to start a family often comes with a complex mixture of hope and apprehension. While most women with cardiovascular pathologies can have successful pregnancies, the physiological demands of gestation—which include a significant increase in blood volume and cardiac output—can place a profound strain on a compromised heart.
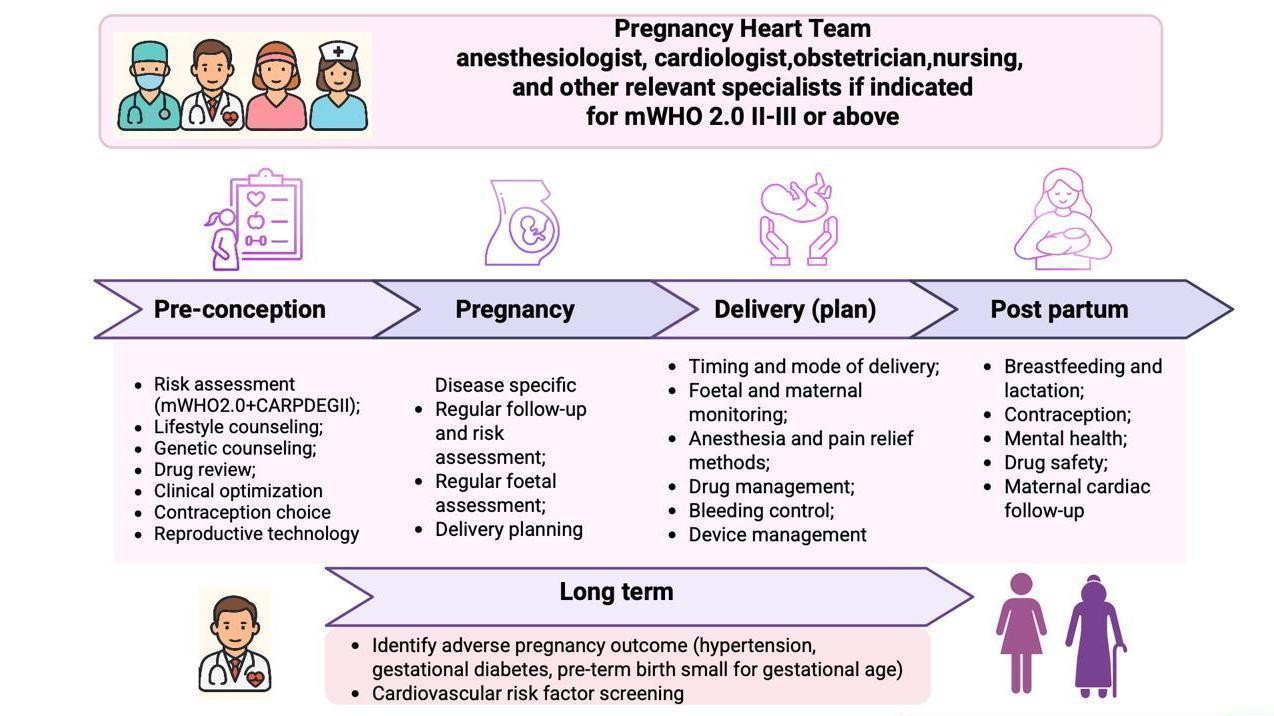
The modern medical consensus has shifted away from a fragmented approach toward a highly integrated model of care. Central to this is the grossesse et pathologies cardiovasculaires management strategy, which prioritizes a multidisciplinary approach known as the “Pregnancy Heart Team.” This team ensures that the decision to conceive is not made in isolation, but through a rigorous assessment of maternal risk and a tailored plan for prenatal and postnatal care.
The Pregnancy Heart Team typically comprises a cardiologist specializing in congenital or acquired heart disease, a maternal-fetal medicine specialist (obstetrician), an anesthesiologist, and often a neonatologist. By coordinating care before conception, this team can optimize maternal health, adjust medications that may be teratogenic, and provide a realistic outlook on the risks and benefits of pregnancy based on the patient’s specific cardiovascular profile.
The Framework of Risk: Understanding WHO Classifications
Not all cardiovascular conditions carry the same weight during pregnancy. To standardize care and communication, clinicians utilize the World Health Organization (WHO) classification of cardiovascular risk in pregnancy. This system allows the Pregnancy Heart Team to categorize patients based on the likelihood of maternal morbidity or mortality.
Patients in the lowest risk category (WHO I) generally experience pregnancies similar to those without heart disease, provided they are well-managed. However, as the classification moves toward WHO IV, the risks grow severe. For women in the highest risk categories, the team focuses heavily on intensive counseling, as pregnancy may be contraindicated due to the extreme risk to the mother’s life.
| Risk Class | Risk Level | Typical Examples/Status |
|---|---|---|
| WHO I | Low | Well-tolerated heart failure, mild valve disease |
| WHO II | Moderate | Mild to moderate systemic hypertension, some congenital defects |
| WHO III | High | Severe pulmonary hypertension, severe heart failure |
| WHO IV | Extremely High | Severe pulmonary arterial hypertension, severe systemic ventricular dysfunction |
This classification is not a static label but a tool for clinical decision-making. For more detailed clinical guidelines, the European Society of Cardiology provides comprehensive frameworks for managing cardiovascular diseases during pregnancy.
Physiological Shifts and Clinical Challenges
Pregnancy triggers a systemic overhaul of the cardiovascular system. By the second trimester, blood volume increases by nearly 50%, and the heart must pump more blood to support the growing fetus and placenta. For a healthy heart, this is a manageable adaptation. for a patient with a pathology, it can trigger decompensation or heart failure.

One of the most critical aspects of the Pregnancy Heart Team’s role is the “medication audit.” Many standard cardiac medications, such as ACE inhibitors and certain anticoagulants, are contraindicated during pregnancy because they can cause fetal malformations or complications. The team must transition the patient to pregnancy-safe alternatives—such as specific beta-blockers or low-molecular-weight heparin—well before the first trimester begins.
Monitoring throughout the pregnancy is intensified. Patients often undergo more frequent echocardiograms and fetal ultrasounds to ensure that the heart is compensating for the increased load and that the fetus is receiving adequate oxygen and nutrients. This vigilant surveillance allows the team to detect early signs of instability and intervene before a crisis occurs.
Planning for Delivery and the Postpartum Period
The climax of the pregnancy—delivery—is often the period of greatest cardiovascular stress. The sudden shift in fluid dynamics and the physical exertion of labor can lead to acute heart failure or arrhythmias. The Pregnancy Heart Team develops a precise delivery plan months in advance.
The decision between a vaginal delivery and a Cesarean section is based on the specific cardiovascular pathology. While vaginal delivery is generally preferred, certain conditions—such as severe aortic stenosis or certain types of congenital heart defects—may make a planned C-section safer to avoid the hemodynamic swings associated with pushing.
Care does not end at delivery. The immediate postpartum period is a high-risk window, as the fluid that accumulated during pregnancy is rapidly reabsorbed into the bloodstream, potentially overloading the heart. Close monitoring in a specialized unit is often required during the first 48 to 72 hours following birth.
Navigating the Path Forward
For patients, the most important takeaway is the necessity of early intervention. Seeking a consultation with a Pregnancy Heart Team before attempting to conceive can fundamentally change the outcome of the pregnancy. This proactive approach transforms a high-risk situation into a managed medical journey.
Advancements in cardiac imaging and fetal medicine continue to refine these risk assessments. As integrated care models become the standard in tertiary hospitals, more women with complex heart conditions are achieving healthy pregnancies and successful deliveries.
Patients are encouraged to consult their primary cardiologist to request a referral to a multidisciplinary pregnancy center. For further information on patient rights and healthcare standards, the World Health Organization offers global perspectives on maternal health and risk management.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Patients should always seek the guidance of their physician or a qualified health provider with any questions regarding a medical condition or treatment.
The next major milestone in this field will be the updated clinical registries focusing on long-term maternal outcomes five to ten years post-pregnancy, which are expected to further refine the WHO risk classifications. We invite readers to share their experiences or questions in the comments below to facilitate foster a community of support and information.