For many living with narcolepsy, the challenge is not simply a struggle to stay awake, but a fragmented existence defined by “sleep attacks,” sudden muscle weakness, and a persistent cognitive fog. While a single medication may address excessive daytime sleepiness, it rarely touches the full spectrum of the disorder, which often includes cataplexy, disrupted nighttime sleep, and comorbid mood disorders.
Clinicians are increasingly moving away from a “one-drug-fits-all” approach, instead optimizing narcolepsy treatment through polypharmacy. By strategically combining different classes of medications, providers can target multiple symptoms simultaneously—stabilizing the wake-sleep cycle while managing the psychiatric burden that often accompanies the condition. This tailored approach recognizes that narcolepsy is a complex neurological dysfunction rather than a simple sleep deficiency.
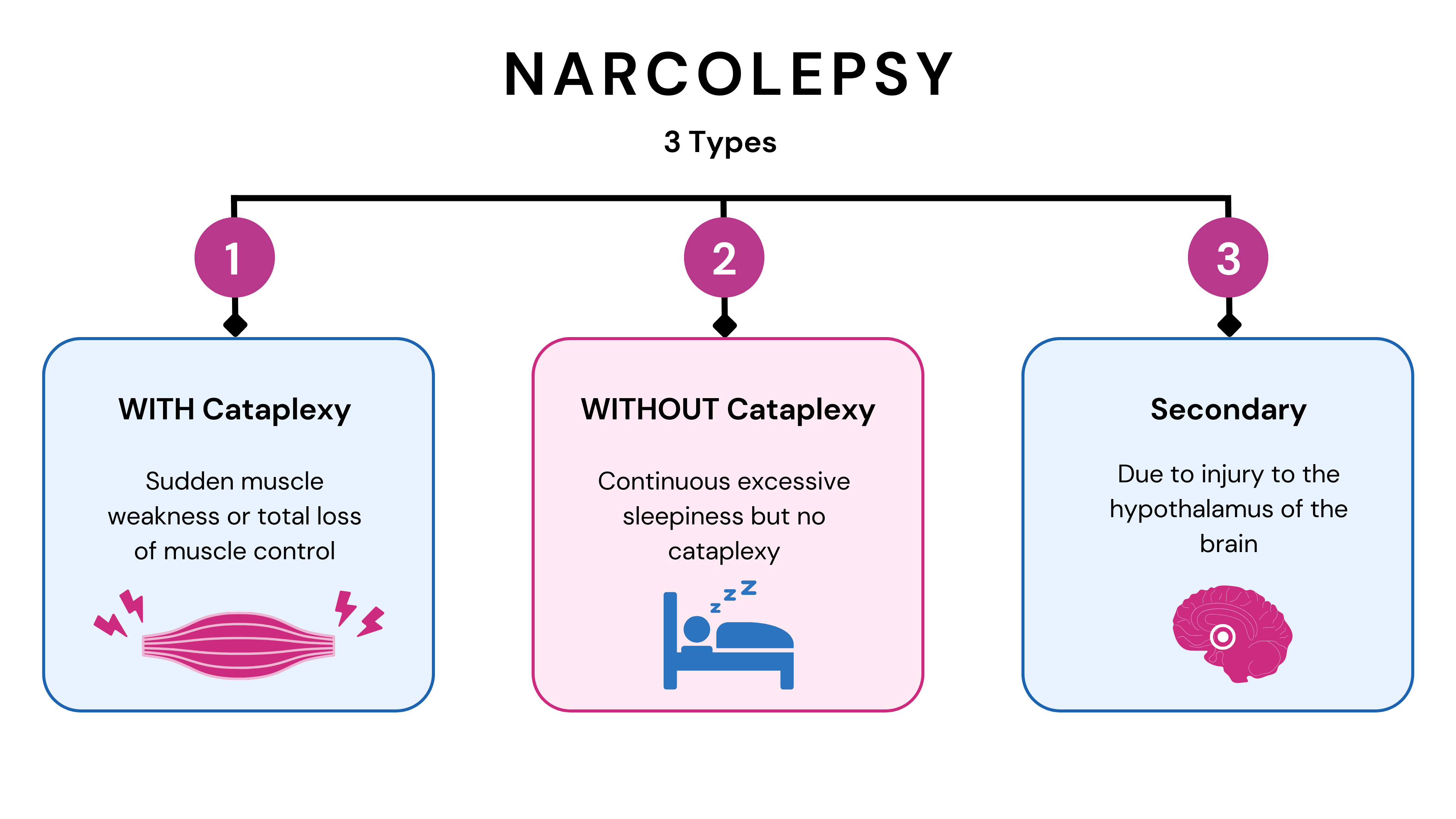
The shift toward combination therapy reflects a deeper understanding of the disease’s pathophysiology. Narcolepsy Type 1, characterized by the loss of hypocretin-producing neurons, and Narcolepsy Type 2, which lacks that specific biomarker, both require a nuanced balance of stimulants, wake-promoting agents, and REM-suppressing medications to restore a semblance of normal daily functioning.
Treating Narcolepsy as a Multisystem Disorder
To understand why polypharmacy is often necessary, it is essential to view narcolepsy as more than a sleep disorder. Patients frequently report a “cognitive haze” and emotional lability that can be mistaken for primary depression or anxiety. In reality, these are often secondary to the instability of the REM sleep boundary, where dream-like states bleed into wakefulness.
When a patient experiences cataplexy—the sudden loss of muscle tone triggered by strong emotions—stimulants alone are insufficient. Cataplexy is a manifestation of REM sleep intruding into wakefulness, requiring medications that suppress REM sleep, such as sodium oxybate or certain antidepressants. A patient may require one medication to maintain alertness during the workday and another to prevent physical collapse during an emotional moment.
the irony of narcolepsy is that while patients struggle to stay awake during the day, they often suffer from severe sleep fragmentation at night. This “sleep-wake instability” creates a vicious cycle where poor nocturnal sleep exacerbates daytime sleepiness, necessitating a dual-pronged pharmacological strategy to address both ends of the 24-hour clock.
The Pharmacological Toolkit for Combination Therapy
Optimizing treatment involves a careful selection of agents that complement rather than counteract one another. The goal is to maximize wakefulness and minimize cataplexy while avoiding the “crash” associated with traditional stimulants.

Wake-promoting agents, such as modafinil and armodafinil, are typically first-line treatments for excessive daytime sleepiness (EDS). Unlike traditional amphetamines, these agents generally have a lower potential for abuse and a more stable profile. However, they do not treat cataplexy. For those symptoms, clinicians often turn to pitolisant, a histamine H3-receptor antagonist, which serves the dual purpose of promoting wakefulness and reducing cataplexy episodes.
For more severe cases, sodium oxybate—a CNS depressant—is often prescribed for nighttime use. It is uniquely effective at improving nocturnal sleep architecture and drastically reducing daytime cataplexy. Because sodium oxybate is sedating, it is frequently paired with a morning stimulant or wake-promoting agent, creating a pharmacological “push-pull” system that mimics a natural circadian rhythm.
| Medication Class | Primary Target | Example Agents | Typical Timing |
|---|---|---|---|
| Wake-Promoting Agents | Excessive Daytime Sleepiness | Modafinil, Solriamfetol | Morning/Midday |
| REM Suppressants | Cataplexy / Sleep Stability | Sodium Oxybate, SSRIs | Nighttime |
| H3 Antagonists | Wakefulness & Cataplexy | Pitolisant | Daily |
| Traditional Stimulants | Acute Wakefulness | Methylphenidate | As Needed |
Managing Risks and Drug-Drug Interactions
The transition to a polypharmacy model requires rigorous clinical oversight to avoid adverse drug-drug interactions. The primary concern when combining stimulants with REM-suppressing agents is the risk of cardiovascular strain or psychiatric destabilization. For example, combining certain antidepressants with wake-promoting agents can, in rare cases, increase the risk of serotonin syndrome or trigger manic episodes in predisposed individuals.
Physicians must similarly monitor for “stimulant tolerance,” where the effectiveness of a wake-promoting agent diminishes over time. Rather than simply increasing the dose—which can lead to insomnia and anxiety—clinicians may rotate medications or introduce a complementary agent to maintain efficacy. This requires a patient-centered approach, utilizing sleep diaries and objective measures of alertness to fine-tune the regimen.
The National Institute of Mental Health and other health authorities emphasize that psychiatric comorbidities, such as major depressive disorder, must be treated concurrently. If a patient’s depression is not managed, the most potent wake-promoting agent may still fail to overcome the lethargy associated with mood disorders.
The Path Toward Personalized Sleep Medicine
The future of narcolepsy care is moving toward precision medicine. While polypharmacy is currently the gold standard for complex cases, researchers are exploring the role of orexin receptor agonists. These potential therapies aim to replace the missing hypocretin (orexin) in the brain, which could theoretically treat all core symptoms of Narcolepsy Type 1 with a single agent, reducing the reliance on multiple medications.
Until such therapies are widely available, the focus remains on the strategic integration of existing tools. Patients are encouraged to seek care from multidisciplinary teams—including neurologists, sleep specialists, and psychiatrists—to ensure that their medication cocktail is balanced and safe. For those seeking more information on current guidelines, the Mayo Clinic provides comprehensive resources on managing the condition’s diverse symptoms.
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition or treatment.
As clinical trials for latest orexin-based therapies progress, the medical community expects more data on their efficacy and safety profiles in the coming year. These developments may eventually simplify the complex polypharmacy regimens currently required to maintain patient quality of life.
Do you or a loved one manage narcolepsy through combination therapy? Share your experiences or questions in the comments below.

